The U.S. Food and Drug Administration (FDA) on August 1 published a list of proposals to further ensure the safety of patients and staff in MRI environments and bolster both safety testing and MRI information in medical device labeling.
Recommendations in the FDA's draft guidance document would apply to "all implanted medical devices, external medical devices that are fastened to or carried by a patient ... and all medical devices that are intended to enter the MRI environment," the FDA stated.
While the draft does not apply to the manufacture of MRI scanners themselves, the agency adds guidance on labeling information that should be included in premarket approval (PMA) applications, humanitarian device exemption applications, 510(k) premarket notification submissions, investigational device exemption applications, and de novo requests.
The proposal reviews and adds recommendations for a variety of MRI safety issues, including the following:
- Heating
- Medical device malfunction
- Extent of image artifacts
- Reporting results
- MRI safety labeling
Relative to heating, the document discusses the interaction between the radiofrequency (RF) coils, RF transmit mode, the scanner's magnet, a patient's anatomy, and any implanted devices. RF safety evaluations "should take into consideration all these variables to ensure that a clinically relevant worst-case heating scenario is assessed," the FDA wrote. "Such evaluation can include appropriate experimental measurements, computational modeling, and simulations."
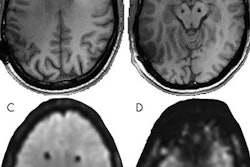
Metallic implants or other medical devices can adversely affect MR image quality and falsely mimic the presence of disease. The FDA suggests that facilities perform a qualitative assessment of image quality and measurement of signal-to-noise ratio using standardized test methods from organizations such as the National Electrical Manufacturers Association (NEMA), with and without the medical device present.
"For medical devices that come in multiple sizes, the largest medical device or the medical device with the largest proportion of magnetic material to total mass can generally serve as a worst case for assessing image artifact," the FDA added. "For multicomponent medical devices, all clinically relevant configurations should be considered."
While the agency already provides guidelines on what information to include in safety test reports, the FDA's proposed guidelines emphasize that imaging facilities should specifically detail the hazard and/or reason for the test and the equipment used for the evaluation, as well as provide details on the scanner's field strength, software, manufacturer, and model.
The FDA also is proposing more thorough information on PMAs and other applications. Beyond the current requirements, device labeling "should include sufficient information for a healthcare professional to determine whether a device can safely enter the MR environment ... in a separate section of your labeling entitled 'MRI Safety Information.' "
The need to designate "MRI unsafe" medical devices remains, and they should be kept outside of the MRI scanner room. In these cases, the FDA recommends an "MR unsafe" icon be placed directly on the medical device, if possible, with text suggesting the device could represent a "projectile hazard."
The FDA's document is scheduled for publication on August 2 in the Federal Register. This will trigger the start of a 60-day comment period. Once the entire process is completed, the final document will replace FDA guidance from December 2014 titled Establishing Safety and Compatibility of Passive Implants in the MR Environment.