
Preoperative breast MRI improves the surgical planning and outcomes of ductal carcinoma in situ (DCIS), according to a new study published online July 5 in Academic Radiology.
The findings offer clinicians a valuable tool for treating women with pure DCIS diagnosed by core-needle biopsy, wrote a team led by Dr. Diana Lam of the University of Washington School of Medicine and the Seattle Cancer Care Alliance.
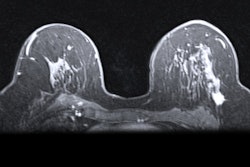
"Because over 90% of DCIS lesions are clinically asymptomatic, appropriate management options are reliant on accurate determination of DCIS extent on imaging," the group wrote. "Preoperative breast MRI can provide more sensitive and accurate assessments of DCIS disease extent compared to mammography alone, which theoretically could assist with determining the optimal surgical approach and allow for improved breast-conserving surgery outcomes."
The use of preoperative breast MRI to evaluate the scope of DCIS has been widely debated, according to the researchers. So they investigated the modality's effect on surgical management of pure DCIS diagnosed by core-needle biopsy.
The study included 373 women diagnosed with DCIS via core-needle biopsy between January 2004 and December 2013. The women did not have prior breast cancer, and all underwent surgery within 180 days of diagnosis. Lam's team compared patient features, number of core-needle biopsies and surgeries, and successful breast-conserving surgery rate between two cohorts: a group of 332 women who had preoperative breast MRI and a group of 41 women who did not. The researchers noted no clinical differences between the two groups.
The preoperative MRI group had higher additional core-needle biopsy rates (30% compared with 7%, p = 0.002) but fewer total surgeries, the researchers found. Women who had preoperative breast MRI also had a greater success rate for breast-conserving surgery.
| Surgical outcomes of women who did and did not have preoperative breast MRI | |||
| Measure | Women who underwent preoperative breast MRI | Women who did not undergo preoperative breast MRI | p-value |
| Total number of surgeries per woman | 1.2 | 1.5 | < 0.001 |
| Total number of surgeries overall | 1.3 | 1.7 | < 0.001 |
| More than 1 surgery | 15.1% | 39% | < 0.001 |
| Successful breast-conserving surgery | 89.4% | 75% | 0.058 |
| Single breast-conserving surgery | 77% | 42.9% | < 0.001 |
The results suggest that preoperative breast MRI can improve treatment planning and also surgical outcomes in women diagnosed with DCIS, according to Lam and colleagues.
"Preoperative breast MRI may improve the surgical management of DCIS at an academic institution that routinely performs [it] for new breast cancer diagnoses, leading to higher success rates of first breast-conserving surgery and lower reexcision rates, without causing a rise in mastectomies or delays in surgical treatment," the group wrote. "Further studies are needed to understand the impact of preoperative breast MRI on both short- and long-term outcomes across a variety of practice types."














![Overview of the study design. (A) The fully automated deep learning framework was developed to estimate body composition (BC) (defined as subcutaneous adipose tissue [SAT] in liters; visceral adipose tissue [VAT] in liters; skeletal muscle [SM] in liters; SM fat fraction [SMFF] as a percentage; and intramuscular adipose tissue [IMAT] in deciliters) from MRI. The fully automated framework comprised one model (model 1) to quantify different BC measures (SAT, VAT, SM, SMFF, and IMAT) as three-dimensional (3D) measures from whole-body MRI scans. The second model (model 2) was trained to identify standardized anatomic landmarks along the craniocaudal body axis (z coordinate field), which allowed for subdividing the whole-body measures into different subregions typically examined on clinical routine MRI scans (chest, abdomen, and pelvis). (B) BC was quantified from whole-body MRI in over 66,000 individuals from two large population-based cohort studies, the UK Biobank (UKB) (36,317 individuals) and the German National Cohort (NAKO) (30,291 individuals). Bar graphs show age distribution by sex and cohort. BMI = body mass index. (C) After the performance assessment of the fully automated framework, the change in BC measures, distributions, and profiles across age decades were investigated. Age-, sex-, and height-adjusted body composition reference curves were calculated and made publicly available in a web-based z-score calculator (https://circ-ml.github.io).](https://img.auntminnie.com/mindful/smg/workspaces/default/uploads/2026/05/body-comp.XgAjTfPj1W.jpg?auto=format%2Ccompress&fit=crop&h=112&q=70&w=112)




