Contrast enhancement of normal tissue on breast MRI scans is more effective than tissue density as an imaging biomarker of breast cancer and could make existing risk models more accurate, according to a new study published online May 12 in Radiology.
Researchers from the University of Washington found that women with an MRI assessment of mild, moderate, or marked background parenchymal enhancement (BPE) were nine times more likely to develop breast cancer than women with minimal BPE. In contrast, tissue density measured by both MR and mammography was not a statistically significant indicator.
"Our results suggest that this breast MR imaging feature [BPE] has the potential to improve upon standard clinical models to more accurately determine a woman's individual breast cancer risk," wrote lead author Dr. Brian Dontchos and colleagues.
How to assess risk?
The American Cancer Society (ACS) suggests that women with a 20% or greater lifetime risk of breast cancer undergo annual MR screening in addition to annual mammography. But figuring out the best way to evaluate risk can be tricky, according to the authors. Population models such as Gail, Claus, and Tyrer-Cuzick are good for assessing risk at a population level but not necessarily at the individual level, because the factors used for these models have weak predictive value and are common in the general population (Radiology, May 12, 2015).
So Dontchos' group decided to explore imaging markers that could improve breast cancer risk assessment, investigating whether there were any associations between breast cancer risk and imaging features such as BPE, the amount of fibroglandular tissue (FGT) on MR, and breast tissue density.
 Dr. Habib Rahbar from University of Washington.
Dr. Habib Rahbar from University of Washington."Density is an imaging biomarker for breast cancer, but it hasn't been very accurate," co-author Dr. Habib Rahbar told AuntMinnie.com. "Many women with dense breasts don't end up developing cancer. So we wanted to explore whether other biomarkers that appear on MR could be more effective cancer risk indicators."
The researchers identified all screening breast MR studies acquired between January 2006 and December 2011 in women ages 18 years or older who were at high risk for breast cancer. They evaluated risk based on family history, known genetic mutations, and history of chest radiation between age 10 and 30.
Among 487 eligible women, 23 received a breast cancer diagnosis after undergoing initial MR; these women were the study's cancer cohort. Control subjects were chosen from the remaining women and matched to the cancer group by age and BRCA status. The researchers then assessed each woman's degree of BPE and its pattern (peripheral or central), the amount of fibroglandular tissue at MRI, and mammographic density.
Of the 23 women diagnosed with cancer, 12 had invasive cancer and 11 had ductal carcinoma in situ. There was no statistically significant association between MR-assessed FGT or mammographically assessed breast density and the development of cancer in the 23 women.
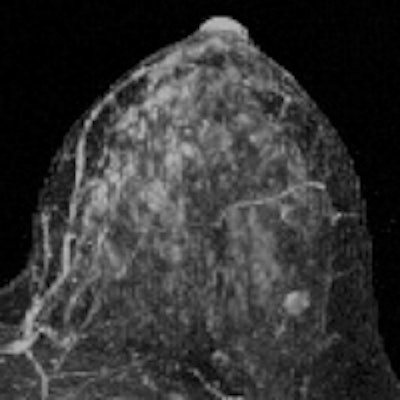
BPE, however, was significantly linked to cancer: The women with mild, moderate, or marked background parenchymal enhancement made up the majority of the cancer cohort.
"We found that a significantly higher percentage of women in the cancer cohort had either mild, moderate, or marked BPE (78%) than did women in the control cohort (43%)," the authors wrote.
| BPE of cancer cohort, controls | ||
| MRI assessment of BPE | Cancer group (n = 23) | Control group (n = 23) |
| Minimal | 22% | 57% |
| Mild | 39% | 26% |
| Moderate | 22% | 13% |
| Marked | 17% | 4% |
The researchers didn't expect that there would be no significant association between fibroglandular tissue or dense breast tissue and the development of cancer, according to Rahbar.
"It was surprising to us that density on MR and mammography didn't correlate with risk for these patients," he said. "Density may be a good enough marker to put a woman into the high-risk category, but it isn't so helpful for figuring out risk level after that."
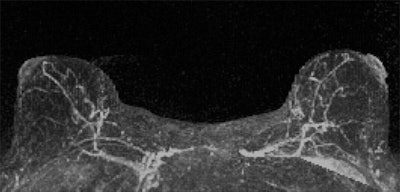
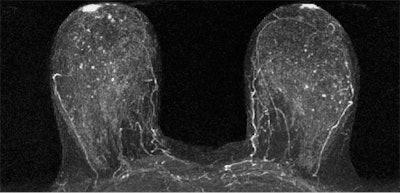
The results suggest that qualitative MRI assessment of BPE may be useful for predicting breast cancer risk -- even more so than MR assessment of fibroglandular tissue or mammographic assessment of density, the researchers concluded. And if the results are confirmed by larger studies, integrating BPE into breast cancer risk assessment tools could help customize options for individual women, according to Rahbar.
"We think these findings could be really important as the imaging community tries to determine how to tailor breast cancer prevention, screening, and treatment strategies," he said.