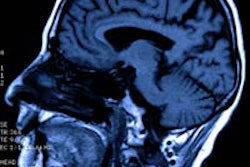
Researchers at Nationwide Children's Hospital in Columbus, OH, are using MRI to better understand how concussion symptoms evolve in young patients and what cases may have lingering aftereffects.
So far, their study has found that one of every four children who suffered a traumatic brain injury or concussion displayed significant postconcussive symptoms more than one year after the injury.
In addition, youngsters with more severe concussions, which result in a loss of consciousness, post-traumatic amnesia, or an abnormal CT scan or MRI, were more likely to have symptoms that persisted. Results from the study were published in the March 2009 issue of Pediatrics (Vol. 123:3, pp. 735-743).
The prospective study recruited children from 8 to 15 years of age who were treated in the emergency departments at Nationwide Children's Hospital and Rainbow Babies & Children's Hospital in Cleveland. There were two groups in the study: 185 children with mild traumatic brain injury or concussion and approximately 100 children with mild orthopedic injury.
 |
| Keith Yeates, Ph.D., lead study author and director of Nationwide Children's Hospital's Center for Biobehavioral Health. All images courtesy of Nationwide Children's Hospital. |
Enrollment criteria
Three criteria for enrollment into the study were that the children had lost consciousness, had a Glasgow Coma Scale (GSC) score of 13 or 14, and showed some sign of impairment from the concussion, such as disorientation, persistent vomiting, or headache. If either of the first two criteria were not present, then the youngsters had to have at least two concussion symptoms.
Glasgow Coma Scale score is a measure of postinjury neurological status, with 15 considered normal, intact, and functioning. "Mild traumatic brain injury has been defined as scores of 13 to 15," Yeates said. "We specified 13 or 14, because, if they were going to qualify by that criteria, we wanted them to show some evidence of impairment."
Of the more severe concussion cases in the study, a child could have loss of consciousness for as long as 30 minutes, plus a GCS of 13 or 14 (unconscious for 10 or 15 minutes and other symptoms) and lesions detected on both CT and MRI.
The rationale behind the expanded criteria was "to make the argument that all concussions are not the same," Yeates added. "Based on what has been defined as mild traumatic brain injury, there is still a fair amount of range in terms of the severity and how we have to evaluate that influence."
Scanning techniques
1.5-tesla MRI scans were performed on all children in the study, primarily because the modality is known to be more sensitive to smaller, more discreet intracranial lesions of traumatic brain injuries than CT.
The imaging sequences for data collection included sagittal T1-weighted and axial T2-weighted imaging, coronal 2D and fluid-attenuated inversion recovery (FLAIR) gradient-echo imaging, and axial diffusion-weighted imaging, all of which were state-of-the-art in 2002 when the study began. All but four children were able to complete an MRI scan. In those four cases, there was too much motion artifact to produce acceptable images.
CT scans also were conducted at the discretion of hospital emergency department personnel; approximately 63% of children in the concussion group received a CT scan. "We found intracranial abnormalities in 8% of those kids with CT," Yeates noted, "compared with 17% on MRI, which is not surprising. We expected to find more on MRI than we did on CT."
In terms of detecting lesions, all but one child with an abnormality on CT showed on MRI, whereas there were children who showed abnormalities on MRI that were not present on CT scans.
MRI abnormalities
 |
| Dr. Karl Klamar of Nationwide Children's Hospital conducts a routine postconcussion exam on a young patient. |
"We knew MRI would be more sensitive than CT; that has been documented in multiple cases of traumatic brain injury," Yeates said. "The question was: Does [MRI] have any clinical value? I think it does, and clearly there are kids with lesions that don't show up on CT, and kids with lesions are at risk for somewhat poorer outcomes than kids without. We may not be identifying all kids at risk by relying solely on CT."
Yeates conceded that MRI scans are more costly and would not be used in an emergency department setting, because CT is more sensitive to some lesions that require more emergent neurosurgical intervention.
"Some subdermal hematomas are easier to visualize on CT than MRI," he added. "So, CT is the preferred imaging modality for the kid who needs emergent neurosurgical care, but it may not necessarily be the best imaging modality for predicting which kids will have functional problems after the injury."
1.5 tesla versus 3 tesla
Although the researchers used 1.5-tesla MRI for the study, Yeates believes that 3-tesla MRI would be more beneficial for these types of lesions and in imaging techniques now being developed, such as susceptibility-weighted imaging and MR spectroscopy.
"Most of the lesions we found, not surprisingly, were often small contusions in the frontal or temporal lobes; those were the most common findings," he said. "If you extrapolate that we are picking up only the most obvious lesions, there are probably even more discreet lesions we can pick up under 3 tesla that we won't see at 1.5 tesla."
The bottom line with MRI is that the data give healthcare providers some reassurance that among higher-risk children with severe mild traumatic brain injury, the majority seem to do very well and largely are asymptomatic within about three months of their injury, Yeates said. There also is a subgroup of higher-risk adolescents who continue to be symptomatic as much as one year after their injury.
Kids at risk
"The trick now is to get a better handle on who they are, and either through imaging or other methods to do a better job of identifying which kids are at risk," Yeates said. "There are some fairly simple interventions that could help to prevent or ameliorate these sorts of problems, if we could identify who those kids are."
With more than half a million children treated for concussions in the U.S. annually, Yeates conceded that not all of them can receive an MRI scan. "You can't closely follow all of them, so we have to get better at figuring out who is at risk," he said.
By Wayne Forrest
AuntMinnie.com staff writer
March 5, 2009
Related Reading
MRI, CT remain front and center in head trauma imaging, April 18, 2007
Brain stem lesion on MRI bodes ill for comatose head trauma patients, April 27, 2006
MRI finds long-term concussion effects, August 29, 2004
Brain damage in boxers occurs long before symptoms, November 15, 2002
Imaging is rarely definitive in concussion, February 21, 2002
Copyright © 2009 AuntMinnie.com