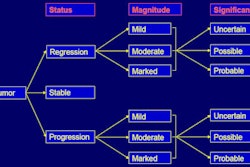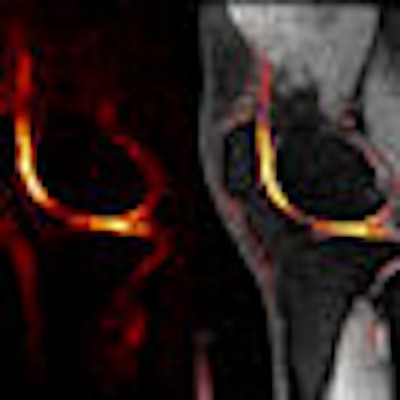
Using an imaging technique known as sodium MRI, researchers at Stanford University in Stanford, CA, are detecting signs of cartilage deterioration soon after a knee injury that could lead to osteoarthritis.
In the 15 years Dr. Garry Gold, associate professor of radiology at Stanford, has been working with MRI and osteoarthritis, the technique of sodium MRI "has always been intriguing, but difficult to do," he said. But newer 3-tesla scanners could turn sodium MRI into a viable clinical application.
Conventional MRI works by using radiofrequency pulses to excite hydrogen protons in the body. Sodium MRI focuses instead on sodium, which occurs in complex with glycosaminoglycan, an elemental metal that has its own set of excitation and relaxation frequencies and is more restricted to cartilage than hydrogen is.
The barrier to sodium MRI, however, is that the element is more than 1,000 times less common in the body than hydrogen, thus producing a lower signal-to-noise ratio.
A possible solution
Three years ago, British pharmaceutical firm GlaxoSmithKline approached Stanford to develop newer MRI methods for detecting osteoarthritis at an early stage. "We proposed developing the sodium MRI methodology because there had been recent advances to hardware and software that we felt would make this clinically practical at 3 tesla," Gold said.
High-field MRI is required to achieve the appropriate signal-to-noise ratio, Gold said. "Three-tesla MR is practical, clinically widely available, and we felt we could get the imaging quality we needed," he added. Three tesla is probably the minimum field strength at which sodium MRI is practical for cartilage, Gold said.
The scan procedure itself is very similar to a conventional MRI. The only difference is a specialized coil developed by Stanford that transmits and receives frequencies to and from the scan. Specialized software, developed in Stanford's electrical engineering department initially for conventional hydrogen-based MRI, controls the image acquisition strategy because sodium has a short T2 relaxation time.
The software currently is in the development stage. Stanford is working with GE Healthcare of Chalfont St. Giles, U.K., to "make it more of a commercial application," Gold said.
Scan time
Clinicians must scan for a longer period of time to get sufficient signal and resolution for osteoarthritis applications of sodium MRI. A 3D image of one knee takes about 20 minutes, Gold estimated.
One advantage of sodium MRI is that no contrast agents are required, as Stanford researchers take advantage of sodium's high natural abundance in normal articular cartilage. "In unhealthy cartilage, sodium is depleted," Gold said. "When we look at healthy cartilage, we see a nice thin, bright area of sodium signal in the cartilage, but when we look at unhealthy cartilage we see asymmetric appearances and irregular signal intensity. This is simply a pure measure of the sodium that is there."
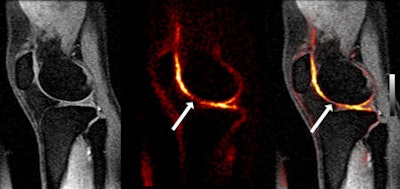 |
| Image courtesy of Dr. Garry Gold. |
Previous methods of imaging for osteoarthritis have used gadolinium contrast agents. In patients who are older than 50, gadolinium "becomes problematic," Gold said, "because of concerns about NSF [nephrogenic systemic fibrosis]. It is also logistically challenging because there has to be a 90-minute delay between the injection of contrast and the acquisition of the images."
So far, the biggest logistical challenge encountered with Stanford's sodium MRI technique was changing the coil between sodium MR and hydrogen proton MR imaging. A Stanford coil engineer recently designed a prototype dual-tuned coil, which works for both sodium and proton imaging, so a patient can be scanned with the same coil.
As of February 2, Stanford has scanned 17 patients with anterior cruciate ligament injuries in the past 10 years or so. The researchers are looking for differences in sodium signal between a patient's injured knee and the healthy knee "because these patients are at high risk for the progression to osteoarthritis in the knee that was injured, even if it was surgically repaired," Gold said.
Early diagnosis
Gold and colleagues hope that sodium MRI becomes a beneficial tool for detecting the onset of osteoarthritis in its early stages. While it is too soon to use the technique for that purpose, Gold said, sodium MRI's immediate future looks promising to help orthopedists determine the efficacy of conventional treatments, such as physical therapy and exercise, on osteoarthritis and to aid pharmaceutical companies in drug development.
GlaxoSmithKline and the National Institutes of Health (NIH) are funding the project.
Sodium MRI's applications also go beyond osteoarthritis. Gold noted that researchers at the University of Pittsburgh Medical Center in Pennsylvania are looking at the brain with 7-tesla sodium MRI to detect tumor recurrence.
Stanford has also been investigating the use of 7-tesla MRI for sodium imaging. Gold believes that sodium MRI is one of the most important applications of 7-tesla MRI in humans, due to the need for a high field strength to produce the necessary resolution.
In addition, Gold's colleague on the sodium MRI project, Brian Hargreaves, Ph.D., assistant professor of radiology at Stanford, is among researchers exploring whether sodium MRI will provide better specificity than proton MRI for diagnosing benign or malignant breast cancer lesions.
To see Gold's explanation of sodium MRI with osteoarthritis, click here.
By Wayne Forrest
AuntMinnie.com staff writer
February 5, 2009
Related Reading
CAD shows potential for knee MR studies, May 26, 2008
U.K. study finds direct access to knee MRI is cost-effective, April 3, 2008
AAOS study: MRI overused for knee osteoarthritis, March 6, 2008
Presence of osteoarthritis influences bone bruise prognosis, August 22, 2007
Plain x-rays not recommended for confirming osteoarthritis, March 31, 2006
Copyright © 2009 AuntMinnie.com