In March 2005 a major trial of accelerated partial-breast irradiation (APBI) was initiated. The goal of this four-and-a-half-year trial is to assess the effectiveness of APBI compared to whole-breast irradiation (WBI) for local tumor control following lumpectomy in more than 4,000 women. The trial is sponsored by the National Surgical Adjuvant Breast and Bowel Project and the Radiation Therapy Oncology Group (NSABP B-39/RTOG 0413).
While phase II of the trial is currently under way, other investigators have used its APBI protocol in their own studies. Last year, a group based at Brown University School of Medicine in Providence, RI, conducted a dose-modeling study to compare the external beam techniques from NSABP B-39/RTOG 0413 for patients with highly unfavorable cardiac anatomy. They found that the 3D conformal external beam accelerated partial-breast irradiation (3D-CRT APBI) resulted in a reduced risk of cardiac morbidity and mortality (International Journal of Radiation Oncology, Biology, Physics, August 1, 2006, Vol. 65:5, pp. 1368-1374).
More recently, at the 2007 American Society for Therapeutic Radiology and Oncology (ASTRO) meeting in Los Angeles, a group from the Ohio-based Cleveland Clinic discussed the role of breast MRI in the management of early breast cancer in patients treated with the trial's APBI protocol.
In other ASTRO research, investigators from Baltimore and Charleston, SC, shared the results of their phase I/II trial of APBI in conjunction with chemotherapy. Using a slightly different APBI protocol, they assessed skin toxicity and cosmetic outcome.
Finally, radiation oncologists from the Washington University School of Medicine in St. Louis tested three different image guidance systems for APBI.
Breast MRI
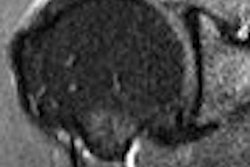
"Breast MRI is a sensitive tool for the evaluation of disease extent in comparison to mammography," said Dr. Rahul Tendulkar in his ASTRO talk, adding that at the Cleveland Clinic patients undergo preoperative bilateral contrast-enhanced breast MRI on a 1-tesla scanner (Harmony, Siemens Medical Solutions, Malvern, PA). The images are interpreted by breast radiologists in conjunction with computer-aided detection software.
For this retrospective review, data from 260 patients with early invasive breast, who also met NSABP B-39/RTOG 0413 eligibility criteria, were included. The median age was 57 years and the majority of women were postmenopausal. The tumor was palpable in 30% of the cases, and one-fourth of the tumors were ductal carcinoma in situ (DCIS). Other tumor characteristics included ER-positive, PR-positive, and HER2-negative. Most of the tumors were stage T1, N0, Tendulkar said. Any suspicious lesions identified on MRI were evaluated with targeted ultrasound and, if appropriate, MR-guided stereotactic biopsy.
According to the results, "MRI in this cohort of patients identified suspicious, additional lesions in the ipsilateral breast in 36 patients and in the contralateral (breast) in 16 patients," Tendulkar said. "Based on targeted imaging, biopsy was recommended and conducted in 27 patients. Biopsy-proven multifocal disease was found in three (patients), multicentric in nine, and contralateral in four. One patient had multifocal and multicentric disease so there was a total of 15 patients with additional lesions that were mammographically occult." The authors defined multicentric disease as lesions in a separate quadrant or greater than 5 cm away from primary lesions.
MRI findings altered surgical management in these 15 patients. Tendulkar also noted that in all cases in which infiltrating lobular carcinoma (ILC) was the primary tumor, MRI found secondary tumors with the same histology. "Also, the secondary tumors tended to be rather small. Only two cases were found in which the tumor size was greater than 2 cm. Both of those secondary (lesions) were DCIS," he said.
MRI's sensitivity for multifocal and multicentric disease in this patient population was 85%, specificity was 87%, positive predictive value was 26%, and negative predictive value was 99%. MRI's overall accuracy was 87%.
"Patients being considered for APBI with infiltrating lobular histology should probably undergo MRI prior to definitive treatment," Tendulkar concluded. "The utilization of breast MR may influence failure rates or patterns of patients ... the hypothesis being that patients (in whom) MR is conducted pretreatment may have lower failure rates."
APBI and ddAC
In another study, Dr. Richard Cedric Zellars and colleagues evaluated the toxicity of APBI with concurrent dose-dense doxorubicin and cyclophosphamide (ddAC). Their goal was to generate preliminary local control data for a larger, randomized efficacy trial.
"With concurrent chemo and radiation, you have shorter overall duration of therapy. Both chemo and radiotherapy start temporally closer to surgery, theoretically maximizing the benefits of both modalities, and improving local control via the radiation-sensitizing effects of chemo," Zellars explained. "Unfortunately, WBI and chemotherapy concurrently has been associated with prohibitive toxicity."
Zellars and co-authors are from the Johns Hopkins Oncology Center in Baltimore and the Medical University of South Carolina in Charleston.
For this study, women with T1, N0 breast cancer with 3-mm lumpectomy margins were enrolled. They received PBI to the lumpectomy bed plus the margin for a total dose of 40.5 Gy (2.7 Gy delivered daily for 15 fractions). PBI was administered in conjunction with two out of four cycles of ddAC (60 mg/m² and 600 mg/m²) delivered every 14 days with colony-stimulating factor support.
The clinical target volume (CTV) was defined as the lumpectomy cavity plus 1.5 cm, and the planning target volume (PTV) was the CTV plus 0.5 cm, Zellars said. In terms of dosimetric limits, the group followed the protocol set by NSABP B-39/RTOG 0413, although they did place tighter restrictions on the dose to the heart: no more than 10% of the heart received more than 5% of the radiation dose, he added.
The primary end point of skin toxicity was graded according to the National Cancer Institute's Common Terminology Criteria for Adverse Events, while the end point of cosmetic outcome was determined by the Fitzpatrick Classification Scale. A frequency of grade 4 radiation dermatitis of 20% or greater was considered unacceptable and would have prompted early closure of the trial, Zellars' group wrote in its ASTRO abstract.
The results were based on 22 women (median tumor size of 1.8 cm) who met the inclusion criteria and had completed radiotherapy as well as chemotherapy. Based on a median follow-up of 16 months, there were no reports of local or systemic recurrences. Of the 22 patients, 82% developed grade 1 radiation dermatitis, but no patient developed anything higher than grade 1. The cosmetic outcome at six months was graded good in 95% of the patients. As of late October, there were no reports of late soft-tissue or skin toxicity, Zellars said.
APBI with concurrent ddAC treatment was feasible with a low latent toxicity and good local control, the group concluded. Moving ahead with their study, the researchers will need to look at other commonly used chemotherapeutic agents as well as conduct a randomized trial comparing sequential to concomitant APBI/chemotherapy, Zellars said.
Image guidance
In the third study, Dr. Sasha Wahab and colleagues evaluated patient positioning using three image-guidance methods: 3D video surface mapping (AlignRT, Vision RT, London), kV on-board imaging (OBI, Varian Medical Systems, Palo Alto, CA), and internal fiducial markers (IFM).
"As we transition from WBI to APBI, we worry about the increased risk of target miss and possible, subsequent tumor recurrence. We want to identify one method to improve accuracy compared with alignment lasers alone," Wahab said in his ASTRO talk introduction.
The study cohort consisted of 26 patients and data from 226 APBI treatment fractions (nine fractions of 4 Gy per patient over the course of one week). For each treatment, the patient was first positioned by alignment lasers.
The on-boarding imaging system was used to acquire orthogonal views, and projected couch offsets using 2D/2D image matching software were recorded although the couch was not moved. Then the 3D surface mapping system was used and the couch was shifted to the final treatment position as laid out by automated topographical matching. Finally, 14 patients had IFMs placed at the time of surgery; the markers were identified on orthogonal images of the patient in the final treatment position.
"When you compare the systems, you see a difference between projected coordinates, averaging about 4 mm. This led us to the questions: Which is the most appropriate surrogate for an internal target within a deformable structure such as the breast? Is it a surface map of skin or is it a deep internal structure, perhaps a fixed structure like skeletal anatomy? We tried to answer this question by looking at residual setup error with reference to our IFMs," Wahab explained.
According to the results, the average 3D isocenter shift from the initial setup position using laser alignment was 8.5 mm with the surface mapping system and 8.45 mm with the on-board imaging system, which Wahab's group called a "striking discrepancy."
Using IFMs as a gold standard for accuracy, the residual setup error was less with the surface mapping system compared to the on-board imaging system. The average isocenter shift needed for IFM alignment was 2.9 mm postsetup for surface mapping and 7.5 mm postsetup for on-board imaging.
In response to several ASTRO attendees' questions, Wahab said his group used a combination of vertebral bodies and the ribs as skeletal landmarks. Also, their protocol did not account for motion due to breathing, and the surface mapping system was not gated for breathing. Finally, the IFMs consisted of an average of six surgical clips that were placed by the surgeons at the time of lumpectomy.
The authors concluded that laser alignment alone was suboptimal for patient positioning, but that surface mapping provided patient positioning accuracy within 2 mm in any one dimension.
"kV (on-board) imaging matched to skeletal anatomy was only accurate to 5 mm," Wahab stated. "We recommend that, if using orthogonal imaging, IFMs should be placed. Surface mapping provided positioning accuracy within 2 cm. When using surface mapping, you don't need IFMs."
By Shalmali Pal
AuntMinnie.com staff writer
November 21, 2007
Related Reading
Cosmetic results good, toxicity mild with accelerated partial-breast irradiation, March 20, 2006
APBI variables affect late tissue toxicity, cosmetic outcome, February 13, 2006
Copyright © 2007 AuntMinnie.com