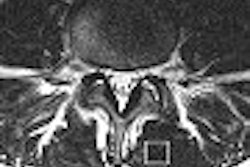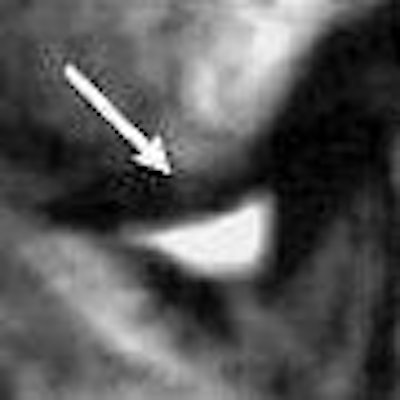
Chances are that dentists won't have to worry about siting a magnet in their offices in the near future, but can the specialty use MRI to its advantage? Yes, if the structure in question is the temporomandibular joint (TMJ).
"Particularly, we look at this disk in the TMJ because (MRI) is the only way we can see the disk. MRI gives you exquisite soft-tissue imaging that you can't get with other imaging," said Dr. Edwin Parks in a talk at the 2006 California Dental Association meeting in San Francisco.
Indeed, over the latter half of the 20th century, MRI has replaced arthrography and arthrotomography as the go-to modality for visualizing the soft tissues of the TMJ, as well as the overall integrity of the structures.
Specifically, dentists need to look at the relationship of the articular disk to the head of the condyle and the head of the glenoid fossa, added Parks, who is director of dental radiology at the Indiana University School of Dentistry in Indianapolis.
Parks recommended that dentists consider MRI for assessing soft-tissue alterations in the TMJ, inflammation, disk displacement, and joint effusion. Researchers in Japan did exactly that, using MRI to pinpoint TMJ disorders and then comparing them to discrepancies of the glenoid fossa.
But not everyone is sold on TMJ MRI. A recent paper analyzed published research on TMJ MRI, questioning whether enough evidence existed to make MRI part of the routine clinical protocol.
RGF and TMJ on MRI
To determine if thickness of the roof of the glenoid fossa (RGF) correlated with TMJ disorders found on MRI, Japanese dentists studied 87 patients with TMJ disorder symptoms who were referred for MRI.
"Little is known about changes in the thickness of the RGF under different normal and pathological conditions. It might be that an increase in joint thickness is a natural response of the body in order to maintain proper joint function," wrote Dr. Kazuya Honda, Ph.D., from Nihon University School of Dentistry in Tokyo. "The present report ... measured the minimum thickness of the RGF in relation to MRI observations of TMJ structure" (Dentomaxillofacial Radiology, September 2006, Vol. 35:5, pp. 357-364).
The MR protocol consisted of T1- and T2-weighted images, in the sagittal and coronal planes, in a closed mouth. T2*-weighted images were also obtained in the sagittal plane with a closed mouth and the mouth open to maximum. A 1-tesla scanner was used (Magnetom Harmony, Siemens Medical Solutions, Malvern, PA). Three-dimensional conebeam CT images (3DX Accuitomo, Morita, Kyoto, Japan) were also acquired to measure the thickness of the RGF at its thinnest point.
According to the authors, the "results showed that there was no significant difference in the minimum thickness of the RGF between normal joints and those classified as ADWR (anterior disk displacement with reduction) or ADWOR (anterior disk displacement without reduction)."
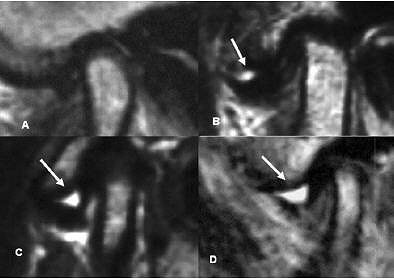 |
| Classification of "with" and "without" joint effusion. Arrows indicate joint effusion. (A) no effusion, (B) minimal effusion, (C) moderate effusion, (D) marked effusion. Panel A was without joint effusion. Panels B-D are examples with joint effusion. K Matsumoto, K Honda, K Sawada, T Tomita, M Araki, and Y Kakehashi. "The thickness of the roof of the glenoid fossa in the temporomandibular joint: relationship to the MRI findings," Dentomaxillofac Radiol 2006 35: 357-364. |
More specifically, there were 70 normal joints, 53 joints with ADWR, and 51 joints with ADWOR. The average minimum thickness of the RDF was 0.85 mm in normal joints, 0.90 mm in ADWR joints, and 0.93 mm in ADWOR joints.
Based on additional analysis, there were 21 joints with osteoarthritis (OA), 153 without OA, 61 with joint effusion, and 113 without joint effusion. The RGF thickness in the OA group was 0.99 mm versus 0.87 mm in the group without OA. RGF thickness in 33 joints with disk deformation was 0.87 mm compared to 0.89 in 141 joints without disk deformation.
However, there was a significant RGF thickness between the groups with joint effusion (0.97 mm) and those without joint effusion (0.84 mm), the authors stated, indicating that RGF thickness is influenced by joint effusion.
While the minimum thickness of the RGF in TMJ did not correlate with disk position or configuration, the increased RGF thickness in OA and joint effusion might indicate a relationship between that thickness and pain, which could be relevant clinical information for treatment planning, the authors stated.
MR results equal better outcome?
In another study, a group from Sweden performed a systematic literature review of the efficacy of MRI in TMJ disorders. While their results did not dismiss the use of MRI in these patients, they did point out the current paucity of high-quality studies on MRI in TMJ.
"Although MRI of the TMJ has now been used for many years, its diagnostic and therapeutic efficacy -- the value of MRI for supporting clinicians in their diagnoses and treatment decisions -- remains unclear," wrote Dr. Napat Limchaichana and colleagues from the faculty of odontology at Malmö University in Malmö, Sweden (Oral Surgery, Oral Medicine, Oral Pathology, Oral Radiology, and Endodontology, October 2006, Vol. 102:14, pp. 521-536).
For this study, the authors mined the PubMed database from January 1988 to July 2005 and found 494 titles. Two reviewers looked these titles over, assessing the level of evidence in favor of TMJ MRI as high, moderate, or low. They also graded the studies for diagnostic efficacy as strong, moderately strong, limited, or insufficient. Ultimately, 22 papers met the study criteria for level of evidence and diagnostic efficacy.
Of those 22 articles, none offered a high level of evidence on the value of MRI in TMJ disorders, according to the authors. Only a dozen offered moderate evidence and 10 had low levels of evidence. More specifically, the studies did not demonstrate a consistent likelihood that MRI could diagnose TMJ disk position.
In terms of TMJ disk configuration, studies showed that the specificity (50%) and positive predictive value (56%) of MR sagittal images were low for identifying biconcave versus deformed disks. Finally, MR turned in only moderate results for identifying osseous changes of the TMJ and bone marrow changes.
"We ... conclude that evidence for observer performance is limited, and evidence for diagnostic efficacy ... is insufficient," the authors wrote. "However, insufficient scientific evidence for a method's efficacy does not necessarily imply that the method is ineffective or should not be used."
Instead, they called for additional studies based on validated methodology for determining diagnostic and therapeutic efficacy. In the 22 studies they reviewed, there was too much variation between diagnostic criteria, the authors stated.
"An ideal appraisal should check observer reproducibility.... Confidence intervals for sensitivities, specificities, and predictive values should also be determined.... At present, it is (impossible) to draw any conclusion about when the results of an MRI examination will result in better treatment outcome for the (TMJ disorder) patients," they concluded.
By Shalmali Pal
AuntMinnie.com staff writer
October 13, 2006
Related Reading
Steroid injection effective for TMJ arthritis, December 15, 2005
Sophisticated 3D volumetric imaging has a place in everyday orthodontics, July 4, 2005
3D diagnosis and planning bring orthodontists closer to 'anatomic truth', June 2, 2005
MRI clicks with TMJ diagnosis and treatment, October 15, 2004
Copyright © 2006 AuntMinnie.com