An ongoing debate in the scuba diving community involves people who have never suffered from type II decompression sickness (DCS), but who may still be at risk for cerebral damage because of "silent" gas embolisms. These paradoxical arterial gas embolisms are particularly problematic in divers who have patent foramen ovale (PFO), but are otherwise healthy, according to German researchers.
"In diving, (right-to-left) shunting may transport nitrogen bubbles analogous to paradoxical embolism of venous thrombi through a PFO," explained Dr. Andreas Koch and colleagues in Undersea and Hyperbaric Medicine, the journal of the Undersea and Hyperbaric Medical Society (Summer 2004, Vol. 31:2, pp. 261-268).
Koch and his co-authors, including radiologist Dr. Michael Reuter, are from the German Naval Medical Institute in Kiel-Kronshagen and the Christian-Albrechts-University of Kiel.
They re-examined previously published research that found a correlation between the presence of PFO and abnormal cerebral findings (ACF) on MRI. Dr. Michael Knauth and colleagues from the University of Heidelberg Klinikum in Mannheim, Germany, suggested that PFO seems to be an important risk factor for the development of multiple brain lesions in sport divers, and that paradoxical gas embolism is a possible cause of neurologic sequelae after decompression (British Journal of Medicine, March 8, 1997, Vol. 314:7082, pp. 701-705; Neurology, January 15, 1999, Vol. 52:2, pp. 401-404).
"In this study, we challenged Knauth's findings in a random group of 50 healthy divers who had amassed a broad range of diving experience and never suffered DCS," they wrote. The 47 males and three females, mean age 34.7, had logged between 21 and 5,500 dives.
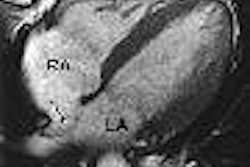
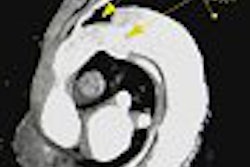
The subjects underwent cranial T1-weighted MRI on a 1.5-tesla scanner (Magnetom Vision, Siemens Medical Solutions, Erlangen, Germany). PFO detection was done using transcranial Doppler ultrasound (TCD) and transthoracic echocardiography (TEE) with contrast (Multi-Dop X4, DWL Elektronische Systeme, Sipplingen, Germany; SSD 807 and PhD 5500 Aloka, Wallingford, CT; Echovist 300, Schering AG, Berlin). Imaging was performed during a Valsalva maneuver.
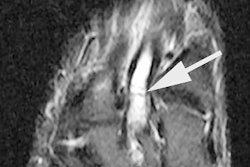
Hyperintense lesions on MRI, such as demyelinated white matter and cerebral lacunae, were considered possibly sequelae or prior paradoxical gas embolism, and counted as an ACF. On TCD and TEE, PFO was considered present if detection occurred within 10 seconds of Valsalva maneuver release.
The results showed that PFO was detected in 36% (18 of 50) of the divers. Of these, 61% demonstrated a right-to-left shunt only after a Valsalva maneuver, and 39% showed shunting without the maneuver. A total of 136 ACFs were found with MRI, including 122 white matter lesions. The majority were found in the brain stem. There was significant correlation between the number of dives and the number of ACFs, the authors reported.
"The fraction of MRI-positives was 56% in the PFO-positive group and 44% in the PFO-negative group," they explained. "The 50 healthy divers examined in this study may have had an overall high incidence of ACFs, but the detection of a PFO ... did not correlate with the prevalence and number of ACFs." These results are in contrast to earlier reports that there is a highly significant correlation between PFO and MRI-detected lesions.
Another study that was released at the same time as the Koch research found that 29% percent of divers with PFO had experienced at least one major episode of decompression sickness. The cardiologists from the University Hospital in Bern, Switzerland, used contrast-enhanced TEE to detection and grade PFO in 230 divers. They concluded that the odds of a diver with PFO suffering from DCS were five times higher and that PFO size parallels DCS (European Heart Journal, June 2004, Vol. 25:12, pp. 1014-1020).
One advantage of MRI over TEE for assessing asymptomatic divers is the fact that it is a noninvasive and less stressful test, Koch's group noted.
By Shalmali Pal
AuntMinnie.com staff writer
January 14, 2005
Related Reading
Pilot study indicates MRI pulls double duty for PFO, atrial septal aneurysm, January 14, 2005
Cluster headache linked to patent foramen ovale, October 22, 2004
Heart defect poses scuba diving risk, July 14, 2004
Copyright © 2005 AuntMinnie.com