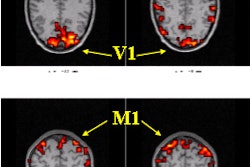
CANCÚN, MEXICO - Radiologists from around the world, gathered here for the opening of the International Congress of Radiology, learned how imaging is addressing a global health crisis.
Their teacher was Dr. Peter Corr, a professor of radiology at the University of Natal, Nelson R. Mandela School of Medicine, in South Africa. Corr talked about AIDS -- specifically the imaging of AIDS-related central nervous system (CNS) disorders. Radiologists can play a crucial role in managing HIV disease, he said.
Worldwide, an estimated 47 million people are now living with HIV; the total has grown by about 7 million just since late 2001, when the World Health Organization released its most recent figures, Corr said. Moreover, an estimated 28 million of those HIV cases are in Africa, where the epidemic has recently shifted from north to south due to people moving around the continent.
"Thirty percent of patients with AIDS have neurological disease in some form," Corr said. "It causes significant morbidity and mortality in these patients, and you as radiologists can often make a difference, in that there are antiretroviral drugs available, and infections can be treated."
Radiology has its greatest impact in the early stages of disease. The role of the radiologist is to detect and characterize focal lesions, perhaps direct stereotactic biopsy in the central nervous system, and to assess the response to treatment. Corr discussed the spectrum of neurological complications of AIDS, from acute encephalitis to peripheral neuropathy, beginning with early HIV infection of the brain.
HIV, a rapidly mutating RNA retrovirus, doesn't infect the neurons, Corr said. Rather, it attacks the brain's supporting cellular structures, the microglia and the macrophages, he said. In the disease’s early stages, patients presenting with clinical manifestations such as headache, stiffening, mononucleosis or glandular fevers, may have normal CT and MRI scans. Sometimes abnormalities such as acute disseminated encephalomyelitis can be seen, however.
In early HIV disease there is often perivenular lymphocytic infiltration, particularly at the gray-white matter interface, Corr said. The infiltration is often seen in MRI as patches in the subcortical white matter and in the basal ganglia.
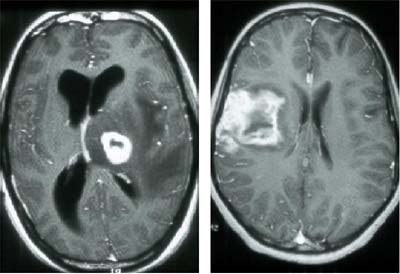 |
| Perivenular infiltration in the brain of an HIV patient. Images courtesy of Dr. Peter Corr. |
HIV encephalopathy corresponds with dementia, and particularly affects the deep white matter of the brain. It occurs in a third of all HIV-infected patients, particularly when the lymphocyte (CD-4) count is less than 100 cells per cubic millimeter, Corr said.
The capsular antigens resulting from HIV are neurotoxic, resulting in the formation of microglial nodules around the neurons, which leads to progressive leukoencephalopathy, he said.
"What you see is cerebral atrophy developing with time. So you may get a young patient in their 40s, and they may have the brain of a 70-year-old," Corr said. "On MR you will see periventricular hyperintensities which do not enhance after gadolinium." Similarly, CT can show marked global atrophy of the white matter.
Toxoplasmosis is a protozoal intracellular parasite, which is probably the most common opportunisitic infection seen in AIDS patients. It is especially important to identify toxoplasmosis, because it responds well to treatment. CT and MR can be nonspecific, but the radiologist can sometimes find a telltale rim-enhancing abscess, particularly in the basal ganglia, and with cortical involvement.
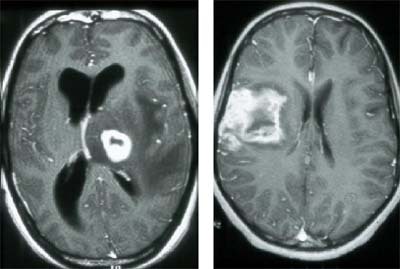 |
| Toxoplasmosis infection in the brain of an HIV patient. Images courtesy of Dr. Peter Corr. |
Tuberculosis is also common in AIDS patients, Corr said. The HIV-infected lymphocyte produces less gamma interferon than its normal counterpart, and therefore has less resistance to the microbacterium that causes TB.
"In TB we classically see a meningitis, a vasculitis is very common, we see granulomas or tuberculomas, and we see a TB abscess," he said. "We see many atypical appearances of TB in AIDS patients." However, the administration of gadolinium during MR can often aid diagnosis by showing rim enhancement of TB lesions.
Syphilis is another common infection in HIV-infected patients. The classic meningovascular syphilis is often seen in combination with stroke and meningitis, Corr said. Many patients also have gummas or parenchymal masses in the brain and spine.
PML is caused by the Papova virus, which destroys the brain's oligodendrocytes, and causes a breakdown of myelin. It a progressive lesion, but dementia is uncommon. The lesions are typically seen in the occipital lobes. They are asymmetrical, and do not enhance with the administration of contrast in MRI. Patients with PML often die within six months of diagnosis, Corr said.
Cytomegalovirus (CMV) is extremely common, and is typically seen when the patient’s lymphocyte count is below 100 cells per cubic millimeter. CMV results in acute encephalitis and ventriculitis, as well as involvement of the retina.
"If you suspect (CMV), always look at the retina for small white lesions. But more commonly, it causes a painful radiculomyelitis. Initially, the imaging may be normal, but if you suspect the diagnosis you must give contrast," Corr said. CMV is best detected with gadolinium-enhanced T1-weighted MR. The gadolinium enhances the root sleeves in the thecal sac.
The most common fungal infection in AIDS patients is cryptococcosis, and though this infection can mimic TB meningitis, sometimes the two can be distinguished in imaging. Cryptococcosis tends to spread up the perivascular spaces from the base of the brain, forming small cysts or occasionally masses, which can be seen on CT and MRI. In the lab, it's important to check for cryptococcal organisms with an India ink stain. Treatment is lengthy but often effective, he said.
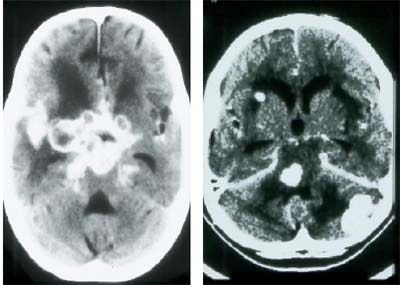 |
| Cryptococcal infection of the brain in HIV. Images courtesy of Dr. Peter Corr. |
Non-Hodgkin's B-cell lymphoma is a differential diagnosis of toxoplasmosis. MR spectroscopy can aid in diagnosis, because in lymphoma the choline peak is elevated, unlike in toxoplasmosis, Corr said. Lymphoma most often involves the basal ganglia and corpus collosum. It can be intimal or meningeal, and importantly, can be multicentric, Corr said.
Vasculopathy is another important component of neurological AIDS presentation, and can be caused by any infection, Corr said. In children there may be calcification of the cerebral cortex, or commonly aneurysm in the Circle of Willis, or in the extracranial carotid artery. Embolic disease, including endocarditis and cardiomyopathy, are among the commonest vascular pathologies, as are aneurysms in the medium-sized arteries of the head and neck.
Spinal-cord involvement also occurs in HIV infection. Autopsies of AIDS patients show that 40% had spinal-cord infection, Corr said. The HIV virus can cause a vacuolar myelopathy, which resembles subacute combined degeneration of the spinal cord similar to that seen in vitamin B-12 deficiency.
However, myelitis due to CMV, HIV, or the varicella (chicken pox) virus are more common forms of spinal cord involvement. When imaging such patients, it’s important to use contrast and image the entire spinal cord, Corr said. Look for swelling of the myelin sheaths and vacuoles appearing between them.
Intradural lesions, especially resulting from CMV and TB, are also seen in HIV patients. Leptomeningeal granulomas are common, and are seen as low-intensity lesions on T2-weighted MRI.
Peripheroradicular neuropathy is a painful condition that is very disabling, Corr said.
"Importantly, when you image (peripheroradicular neuropathy) you must do axial, pre- and post-gadolinium T1-weighted scans," he said. "They almost light up like light bulbs, and this is very characteristic of CMV radiculomyelopathy."
The spectrum of opportunistic infections is one that Corr hopes to change as antiretroviral drugs become more widely available in South Africa.
"Our patients are certainly living longer, and are coming back for more and more scans," he said. "It's important to realize that these often have multiple infections, and you must correlate your imaging findings with the clinical signs, and CSF and laboratory signs when interpreting imaging."
By Eric Barnes
AuntMinnie.com staff writer
July 2, 2002
Copyright © 2002 AuntMinnie.com