CHICAGO – F-18 fluciclovine PET/CT shows promise detecting metastatic lesions in women with invasive lobular carcinoma (ILC), according to research presented November 27 at RSNA 2023.
Presenter Aliza Mushtaq, MD, a postdoc research fellow at Emory University, discussed a study comparing use of two PET radiotracers (F-18 fluciclovine and gallium-68 PSMA) versus conventional imaging in 20 women with new or suspected recurrent Invasive lobular carcinoma (ILC). Both tracers were superior to conventional imaging, with F-18 fluciclovine detecting more metastatic disease, she noted.
“Is this a red herring or a clue deserving further study?” Mushtaq said, in a session on molecular imaging for breast cancer.
ILC is a type of invasive breast cancer that begins in the milk-producing glands (lobules) of the breast. It is the second most common invasive breast cancer, accounting for 10 percent of all invasive breast cancers. Patient survival rates drop dramatically from nearly 100% if detected early to 22% if the cancer metastasizes.
PET tracers F-18 fluciclovine and gallium-68 PSMA-11 are both commercially available in the U.S. for imaging suspected cases of prostate cancer relapse. However, ILC also overexpresses similar proteins as prostate cancer, and thus researchers are exploring use of the tracers in these cases.
In this study, Mushtaq and colleagues enrolled 20 women with new or suspected recurrent ILC from a previous trial at Emory University. Patients had undergone PET/CT scans after IV administration of F-18 fluciclovine and Ga-68 PSMA on separate days. For comparison, conventional imaging included CT or bone scans in 13 patients and F-18 FDG-PET in seven patients.
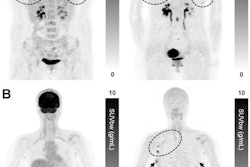
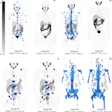
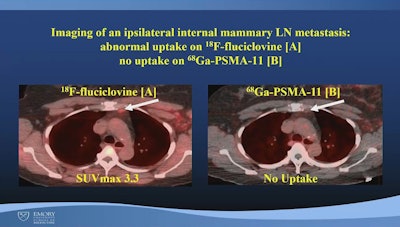 An image from Mushtaq's presentation showing a comparison between PET radiotracers in a patient with ILC. Image courtesy of Aliza Mushtaq, MD, Emory University.
An image from Mushtaq's presentation showing a comparison between PET radiotracers in a patient with ILC. Image courtesy of Aliza Mushtaq, MD, Emory University.
Three experts assessed radiotracer uptake per patient as well as in three regions per patient: ipsilateral axillary lymph nodes (LN), extra-axillary LNs (ipsilateral supraclavicular, internal mammary), and distant lesions (metastases).
Conventional imaging detected metastasis in five patients and in seven out of 60 regions of interest (two axillary, two extra-axillary, and three distant); Ga-68 PSMA-PET/CT detected metastasis in seven patients and in seven of 60 regions (four axillary and three distant); and F-18 fluciclovine detected metastasis in nine patients and in 13 of 60 regions (five axillary, three extra-axillary, and five distant).
“F-18 fluciclovine PET/CT has higher detection for metastases compared to [conventional imaging] and Ga-68 PSMA on a patient and region level,” Mushtaq said.
Moreover, F-18 fluciclovine PET was positive in all regions positive on PSMA-PET, while in six regions positive on F-18 fluciclovine, Ga-68 PSMA was negative, Mushtaq added. Ultimately, while promising, the study was limited by the small number of patients and larger trials are warranted, Mushtaq said.
“In the management of patients with ILC, novel molecular imaging, especially with F-18 fluciclovine PET-CT seems to result in greater metastases detection and deserves further study,” she concluded.










![A 53-year-old patient (patient number four) with a recurrent pituitary adenoma with extension of a cystic component of disease to the medial temporal lobe apparent on MRI (contoured in blue), and extension of disease to the left sphenoid bone and orbital apex apparent on [68Ga]Ga-DOTA-TATE (contoured in yellow).](https://img.auntminnie.com/mindful/smg/workspaces/default/uploads/2026/04/pituitary-tumor.QGsEnyB4bU.jpg?auto=format%2Ccompress&fit=crop&h=112&q=70&w=112)