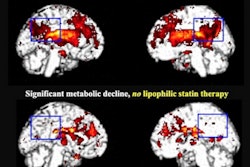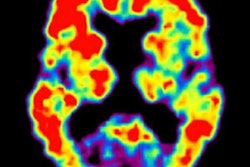
Patients who were on cardiovascular medications like cholesterol-lowering drugs seem to have lower levels of amyloid burden on PET scans, according to a study published February 7 in JAMA Network Open. The question is whether these findings indicate the individuals are at lower risk for Alzheimer's disease.
Canadian researchers found that patients who took medications for vascular conditions, such as high cholesterol levels and blood pressure, had muted results on PET for beta-amyloid accumulation. Conversely, individuals who were not on vascular medication exhibited greater levels of several vascular risk factors, as well as increased beta-amyloid deposition in the brain.
"The findings of this cross-sectional study suggest that an individual's use of vascular medications is an important consideration when studying any association of vascular risk factors and Alzheimer's pathogenesis," wrote lead author Theresa Köbe, PhD, and colleagues from McGill University in Montreal. "Our findings also suggest the importance of targeting both systemic vascular burden and amyloid-beta burden in interventional studies of healthy individuals at risk of Alzheimer's."
The presence of beta-amyloid plaque in certain brain regions is one of the telltale signs that a person might develop dementia or Alzheimer's disease. Concurrently, vascular risk factors such as hypertension are believed to contribute to beta-amyloid accumulation and cardiovascular disease. However, previous research has produced mixed results as to whether poor vascular health and the development of beta-amyloid protein are definitively connected.
"Such inconsistent results might be explained by potential moderation by vascular medications," the authors suggested. "Depending on treatment duration and type, the use of statins and antihypertensive drugs may be associated with providing protection against beta-amyloid deposition."
The question is: Do these types of vascular medications really provide a deterrent to beta-amyloid buildup? Köbe and colleagues hypothesized that PET would indicate more beta-amyloid in people who did not take vascular medications compared with patients who took medications to control their vascular irregularities.
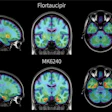
To test their theory, the researchers analyzed a total of 215 cognitively normal adults (mean age, 62.3 ± 5.0 years; range 55 to 82 years). Of those subjects, 120 people (56%) underwent PET with either the radiotracer NAV4694 (Navidea Biopharmaceuticals) or flortaucipir (Avid Radiopharmaceuticals), 75 of whom (62%) were not taking vascular medications. A variety of participants' vascular risk factors, including cholesterol levels, blood pressure, and cardiac risk profile score, were evaluated prior to PET scans.
Among the subjects not taking vascular medications, PET measured higher levels of beta-amyloid deposition, which were associated with significantly higher total cholesterol and low-density lipoprotein (LDL) cholesterol levels, systolic blood pressure, and coronary risk profile score. The researchers, however, could find no statistically significant associations between vascular risk factors and beta-amyloid accumulation among the adults taking the medications.
Interestingly, the authors also found no significant difference in the mean beta-amyloid burden or association with vascular risk factors when they combined results for all subjects, regardless of whether the patients were on medication or not.
Perhaps most importantly, Köbe and colleagues noted that the findings could have "clinical implications," and that future researchers should be aware that "cardiovascular medication might reduce Alzheimer's risk by lowering arterial stiffness, leading to increased cerebral blood flow and [beta-amyloid] clearance."