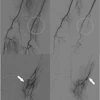
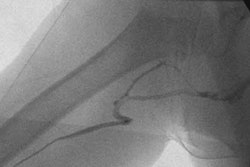
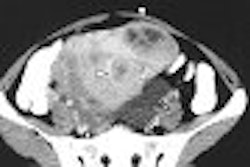
NEW ORLEANS - A number of uterine fibroid embolization (UFE) studies presented this past weekend at the Society of Interventional Radiology (SIR) meeting drove home an important message: Fibroid volume, as well as the size of the spherical polyvinyl alcohol (SPVA) particles used in treatment, can determine the success of UFE, also known as uterine artery embolization (UAE).
In the first reported long-term study, UFE was as durable as myomectomy, although women with large fibroids or uterine volume may not be good candidates for the procedure, according to Dr. James Spies, professor and chair of radiology at Georgetown University Hospital in Washington, DC.
"This means that UFE is comparable to myomectomy for treatment of symptomatic uterine fibroids. In this series, 73% of women said their symptoms were improved by UFE, and that improvement was sustained for five years," Spies explained in an interview with AuntMinnie.com. In myomectomy trials, "the reoperation rate at five years varies widely -- 15% to 50%."
But he cautioned that there are no data to confirm superiority of either UFE or myomectomy, which "would require a direct comparison, and that study has not yet been done."
However, these long-term results also offer the first clinical data to "suggest that some women will do better with UFE than other women. We can use these data to help select women for UFE," Spies said.
Spies reported on 182 women of an original cohort of 200 women. Outcomes were assessed by questionnaire, patient symptom scales, and menstrual cycle regularity. Treatment failure was defined as hysterectomy, myomectomy, repeat embolization, or failure of symptom control.
He said that 20% of the women experienced treatment failure or had recurrent fibroids at five years. Among those failures were 25 hysterectomies, six myomectomies, and three repeat embolizations.
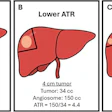
Patients who reported less reduction in fibroid volume at one year were more likely to fail (odds ratio 3.02; 95% CI: 1.02-8.93), and patients with baseline fibroid volumes of more than 151.5 cc were more likely to require interventions (surgery or repeat UFE) after one year (RR 3.33; 95% CI: 1.30-8.53).
The women in the study with fibroid volume of more than 150 cc were more likely to require additional surgery to successfully treat the fibroids, Spies stated. Likewise, women with a uterus greater than 20 weeks' gestation may also require additional surgery, even though UFE may provide symptomatic relief of bleeding and pressure from fibroids.
"I will use this information to counsel women. So if a woman has larger fibroids or if she has significant abdominal wall distortion, I would suggest that she might consider surgical options," he said. But because UFE is a nonsurgical procedure that requires at most only an overnight hospital stay, "many women may still opt for UFE because they can't take the time for surgery, or they just don't want surgery."
Supersize it
While those long-term results were reassuring for UFE proponents, a number of other studies suggested that some sizes of SPVA may be too small to effectively infarct fibroids to achieve durable results.
Boston Scientific, the makers of Contour SE Microspheres, recently responded to these criticisms by recommending a "Refined Protocol for UFE," using 700-900 µg particles (or even 900-1,200 µg particles) to near or complete stasis. Previous literature suggested using 500-700 µg particles.
"The problem is that you can get an excellent clinical result by just infarcting a third of the fibroid," Spies explained. "But what happens is that the remaining fibroid grows back, and you have recurrence." He told AuntMinnie.com that he was one of several UFE researchers who informed Boston Scientific and the FDA about the drawbacks of the smaller size spheres in terms of treatment outcomes.
He said the particle size problem was not apparent in clinical trials submitted to the FDA because "those studies relied upon clinical results -- symptom relief and reduction of uterine/fibroid volume measured by traditional MRI. Now, we have the availability of functional MRI, and we can clearly see the extent of the infarct."
While Spies acknowledged Boston Scientific's effort to inform physicians of the particle size issue, he cautioned that the change would take time.
"This is like trying to change the direction of an ocean liner. Once something has been incorporated into clinical practice, you can't turn that practice around on a dime," he said.
A Boston Scientific company representative at the SIR meeting declined to comment on the matter.
An alternative to larger microspheres is classic nonspherical polyvinyl alcohol (NPVA) particles, which do achieve good infarct, Spies said. This was illustrated in a late-breaking SIR presentation on the difference between PVA boulders and spheres in UAE.
Dr. David Levin and colleagues at the Hospital of the University of Pennsylvania in Philadelphia performed a retrospective study that compared two groups of women who underwent UAE with either traditional NPVA or SPVA particles.
Uterine size decreased by a mean of 28% from baseline in the 23 women treated with NPVA, compared with a 16% decrease in uterine size among women treated with SPVA. Moreover, the women treated with SPVA were "3.7 times more likely to have fibroids that escaped treatment, which was significant (p = 0.036)," Levin said.
The women in the SPVA group were treated with 500-700 µg particles, while the NPVA particles were 350-500 µg.
In a second paper examining particle size, Dr. Jean-Pierre Pelage from Hospital Ambroise Pare in Boulogne, France, made the case for larger particles for treatment to stasis.
He reported that when women were treated with 500-700 µg particles, complete devascularization of the dominant fibroids "was present in only one of 13 women (8%), but in a second group of women treated with particles larger than 700-900 µg, 83% -- 19 of 23 women -- had complete devascularization at 24 to 72 hours by contrast MRI (p < 0.05)."
"To obtain satisfactory fibroid devascularization, the use of PVA microspheres larger than 700-900 µm and embolization of the uterine arteries to stasis seems more effective than a limited uterine artery embolization using 500-700 µm microspheres," Pelage said.
The final particle size paper was presented by Dr. Gary Siskin of Albany Medical Center in Albany, NY. He reported contrast-enhanced MRI findings from a series of 124 women who underwent UAE using 500-700 µg microspheres. All women were treated to near stasis.
Sixty-nine of the women had follow-up contrast-enhanced MR, and of those women only half had 100% infarction on MR, while a third achieved 81% to 99% infarction. The remaining 16% had achieved infarction of less than 80% of the fibroid, and among these women more than half (seven of 11) experienced persistent symptoms and four women had evidence of persistent fibroid growth.
Since most of the women (84%) achieved fibroid infarct of more than 80%, UAE using 500-700 µg particles and treating to near stasis is a success, Siskin concluded.
But upgrading to larger particles may not be the magic answer. Spies pointed out "that when the procedure failed to achieve complete infarct, outcome was not durable." A combination of larger particles and better technique is required to achieve complete stasis, he said.
By Peggy Peck
AuntMinnie.com contributing writer
April 5, 2005
Related Reading
Fibroid embolization does not seem to complicate pregnancy, April 4, 2005
Suture-mediate closure puts UAE patients back on their feet sooner, March 30, 2005
IR, ob/gyns square off in UAE performance debate, March 25, 2004
Copyright © 2005 AuntMinnie.com