Monday, November 27 | 11:20 a.m.-11:30 a.m. | SSC06-06 | Room N230B
Radiologists can combine subjective and quantitative analyses of CT scans to help them grade chromophobe renal cell carcinomas, Canadian researchers will report in this Monday morning presentation.The Fuhrman nuclear grading system has long been used to predict the outcome of renal cell carcinomas, but this prognostic tool cannot be applied to chromophobe tumors, Dr. Nicola Schieda from Ottawa Hospital told AuntMinnie.com.
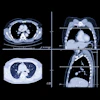
The investigators set out to determine to what extent data from CT scans could help determine the grade of chromophobe renal cell carcinomas. Two radiologists first evaluated the tumor margin, homogeneity, and calcification of renal cell carcinomas on CT scans. A third radiologist then measured the size and attenuation of the tumors on the same scans.
They found that high-grade tumors consistently turned out to be larger, show higher attenuation, contain more calcification, be more heterogeneous, and have more irregular margins than low-grade tumors. The differences were statistically significant (p < 0.05), and interobserver agreement was moderate.
"CT is accurate in differentiating low-grade from high-grade [chromophobe] renal tumors," Schieda said. "A priori knowledge of tumor grade diagnosed on CT may be useful to surgeons when deciding between partial or total nephrectomy and surveillance in renal masses."