
Your organization's patient radiation dose management program is under scrutiny. There is an increasing amount of articles, legislation, and litigation regarding the key components of your patient-care performance surrounding radiation safety, and your healthcare system's business vision. If you think that you have a robust radiation safety program -- think again!
Proactive, patient-focused, and competitively savvy organizations are assessing their existing radiation dose management programs and realizing, based on the backdrop of today's healthcare environment, that they don't measure up to industry standards. Patient radiation dose safety should not just be about meeting compliance, it should also be about implementing good patient-care practices, which makes that organization a leader in the industry.
Your organization can measure up to the industry standard regarding its internal radiation dose management program. Building a robust radiation safety program requires evaluating and updating existing patient-care processes, evaluating and integrating technological solutions, and educating both staff and patients about radiation safety practices and how to recognize and acknowledge potential areas of risk through reporting.
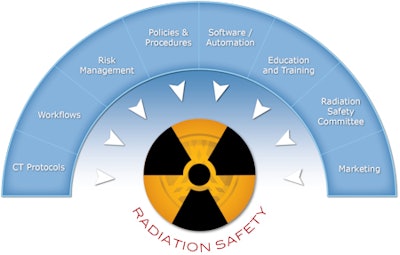 Image courtesy of Ascendian Healthcare Consulting.
Image courtesy of Ascendian Healthcare Consulting.While reviewing the categories below, conduct a short analysis of your organization and answer the following question: "What is our organization's status for each category, and how will we plan to get there?" Evaluate your current activities to identify the gaps to be filled in building comprehensive patient radiation dose safety management.
Check box 1: Building a radiation safety committee
A successful radiation safety program will begin with your organization's key stakeholders, who share a collective goal in patient care for implementing changes, updates, and enhancements to the current clinical environment to drive the formation of your new radiation safety goal. When building the team that will ultimately become your radiation safety committee, it is important not only to select the appropriate resources, but also to include members of your organization to become advocates of the organization's radiation safety objectives.
Of course, there are key team members who immediately come to mind -- a C-suite sponsor, chief legal counsel, radiology directors, your organization's physicist, and a radiologist. Although this small group may be sufficient to get the job done, it is recommended that you expand your considerations to include additional resources who may be affected by the implementation of this new program, and who may even play a critical role in rolling out the enterprise radiation dose safety program.
For example, your IT staff will be very important if you intend to purchase any software or automation solution as part of your radiation safety program. Other valuable resources to consider are your radiologic technologists, who will be responsible for adopting new radiation safety procedures and workflows; referring physicians, who will have to make key imaging decisions when ordering exams; biomed personnel; and quality assurance representatives at your facility.
Perhaps your organization already has a radiation safety committee, but have you taken the next steps to implement patient safety into their roles and daily practices? The radiation safety committee that you create will ultimately drive the successful development and implementation of your patient radiation safety program. Ensure you have your key resources on board!
Check box 2: Full understanding of workflows
In developing a robust radiation safety program, it is imperative to clearly outline the current clinical and technical workflows within your organization. This will include a full assessment of the workflows of the departments and staff members who will be impacted as part of your program.
 Neomi Mullens of Ascendian Healthcare Consulting.
Neomi Mullens of Ascendian Healthcare Consulting.
The purchase of an automated radiation dose management software solution may further affect your future workflows and should be identified early on. Understanding existing processes while considering the identified workflows of a particular solution will allow your organization to strategize the full measure of a radiation safety program.
Capturing current imaging procedures and workflows allows for review and assessment of your existing environment, which will assist you in determining the changes and enhancements that need to be incorporated and give you a strategy to implement these new processes. Adoption of new processes related to an automated system will rely heavily on a clear understanding of new clinical routines to be introduced into the radiology department.
In addition to any IT changes, a workflow analysis allows for all procedural components to be evaluated for efficiency and best-practice methodologies for all members supporting the radiation safety program.
Check box 3: CT protocol review
It is essential that your organization addresses standardizing and password-protecting your CT imaging protocols. Through regular review of CT protocols and imaging techniques utilized by technologists, the radiation safety committee will ensure patients are being scanned using ALARA (as low as reasonably achievable) radiation standards, while maintaining high-quality diagnostic images.
Dose thresholds should be evaluated and maintained in alignment with recommended industry standards. The American College of Radiology (ACR) and American Association of Physicists in Medicine (AAPM) are two excellent resources that can provide information regarding imaging radiation dose threshold and imaging protocol best practices. However, organizations should implement CT radiation dose thresholds based on the perfect balance of good image quality and delivering the lowest radiation dose to the patient.
Check box 4: Software/automation
Radiation monitoring and dose data-collection software is a highly desirable and efficient method of standardizing radiation safety procedures within healthcare organizations. By capturing patient and imaging modality radiation dose data and providing a detailed report of your current imaging procedures, thresholds, and protocols, these automated solutions empower your radiation safety committee to evaluate current imaging practices and determine where inefficiencies can be addressed or changes can be made.
Automated dose management solutions can empower your employees to become actively engaged in maintaining a safe environment for your patients. By implementing a radiation dose management software solution into the physician's workflow, you will be arming your clinicians with a powerful decision-making tool to determine when and if to image a patient using CT or other imaging modalities based on the patient imaging and radiation dose history.
An automated radiation dose management system will allow your organization to receive consistent data, thus increasing efficiency in gaining a snapshot into your current environment. This information can then be utilized to educate physicians and employees and consistently re-evaluate your radiation safety program on a regular basis.
Check box 5: Policy, procedure, and risk management
To gain organizational support and participation in your radiation safety program, it is imperative to develop organizationally approved and clearly defined roles and responsibilities in your program's policies and procedures. This should be a codified set of processes that address all components of a radiation safety program -- from imaging standards and dose thresholds to dose incident management and patient communication.
The rules and practices for all individuals supporting the radiation safety program should be clearly defined. In particular, the policies and procedures should directly outline a process for tracking and reporting events where patient dose exposure exceeds the thresholds or guidelines developed and implemented by your organization. This risk-management guide should be followed to ensure all patient-safety incidents are properly addressed and rectified in a timely manner with the proper resources involved.
Check box 6: Communication, education, and training
Communication, communication, communication! As mentioned earlier, building a strong radiation safety committee that represents your organization is critical to ensuring the success of a radiation safety program -- but don't stop there.
Education and training among your organization's executives, clinicians, technologists, patient-care advocates, nursing staff, and everyone else involved in your radiology workflows are critical to the adoption of an effective radiation safety program and for providing your staff with a knowledge base to lead a successful transformation. Utilizing workflow analysis and data collected by radiation dose measurement software products to educate your staff will be a key component to ensuring the appropriate changes are adopted into imaging routines and scanning techniques.
Routine reports can be generated to track dose management practices within the radiology department, and they may be used by all clinical staff to address outliers (you will find them), inconsistencies, or imaging practices that may not be up to your organization's standards. Utilize the program and the data driven from a software system as a teaching tool within your organization. Educating your staff on radiation safety practices and organizational goals will help advance your organization as a leader in the industry.
Check box 7: Marketing plan
Legislation and legal ramifications may have been the stimulus behind the initial dive into radiation safety awareness within the medical community. However, today's urgency and demand for the adoption of a safety program is coming directly from healthcare organizations themselves and their mission through radiation dose management and patient safety initiatives.
A fully codified radiation awareness initiative and strong dose management program are invaluable additions to any healthcare organization striving to be competitive in the national and international healthcare market. Organizations with streamlined processes, genuine interest in patient safety, and a solid foundation in best practices regarding radiology and imaging services are highly coveted by patients and also by physicians and clinicians desiring to work in a medical environment that offers such enhanced services and a reputation for being at the forefront of this emerging culture.
A radiation safety program is very attractive in today's highly competitive world of healthcare, so make sure your organization is at the top of the list when it comes to providing the best possible radiology services and patient care and safety.
Now, more than ever, radiation safety initiatives are on display as healthcare organizations drive their patient-centric missions and competitive differentiation. Patients are beginning to ask all the right questions when it comes to understanding their radiation exposure and the medical decisions being made by their physicians.
Healthcare providers are also being questioned by their quality assurance teams and employees as to how to respond with proactive patient safety measures, postincident management solutions, and thought leadership surrounding radiation dose exposure. Building a radiation safety program that incorporates all of the critical components for success will bridge the gaps between healthcare providers, their patients, and the emerging technologies that make radiation dose monitoring an essential part of healthcare.
Neomi Mullens is a project manager at Ascendian Healthcare Consulting and a frequent contributor to the subject of enterprise dose management and tracking. You may contact her directly at [email protected] or visit the Ascendian website for more information.
The comments and observations expressed herein are those of the author and do not necessarily reflect the opinions of AuntMinnie.com.




















