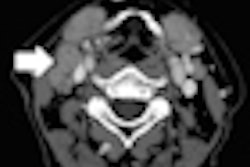
Intracerebral hemorrhage is becoming less deadly and more surgically treatable, thanks to a new CT-guided technique that applies drugs directly to clots in patients' brains via a catheter, dissolving them within a couple of days, according to a new study presented this week at the International Stroke Conference in New Orleans.
Approximately half of people who suffer from intracerebral hemorrhage die from it, said researchers from Johns Hopkins University in a statement accompanying release of the study, which was also performed at the University of Cincinnati and the University of Chicago. Most patients receive only supportive care in an intensive care unit; craniotomy surgery is risky and undertaken in only about 10% of patients.
The paper by lead author Dr. Daniel Hanley and colleagues describes a procedure in which the surgical team makes a dime-sized hole in the skull near the clot and then guides a catheter through the hole and directly into the clot. The catheter is then used to drip small doses of clot-dissolving tissue plasminogen activator (t-PA) into the clot for a couple of days.
The researchers treated 93 patients (ages 18 to 80 years), who were randomized to receive either the new treatment or traditional "supportive" therapy that gives clots time to dissolve on their own.
According to the results, patients treated with the new CT-guided therapy saw their clots shrink about 20% per day, versus 5% for patients who received standard supportive therapy. The new technique also broke the clots without the potentially injurious side effects associated with craniotomy, Hanley said.
The procedure, performed in about two dozen centers in the U.S., doesn't require special equipment and appears to protect the brain better than craniotomy, Hanley said in the statement.