Dear AuntMinnie Member,
A new study presented at this week's San Antonio Breast Cancer Symposium (SABCS) indicates that an alternating screening schedule of breast MRI and mammography may catch cancers earlier in high-risk women.
The patients alternated between breast MRI and mammography every six months, rather than the standard approach of having both an MRI and a mammogram each year, according to an article in our Women's Imaging Digital Community. The researchers found that using the alternating schedule uncovered more cancers than the conventional approach. For more information, click here.
In other reports from the SABCS, researchers found that ultrasound measurement of breast skin thickness can be used to diagnose breast lymphedema after mastectomy. Another study showed that women with early-stage HER2-positive breast tumors of 1 cm or less are at high risk of recurrence and should be considered for adjuvant therapy.
Get these stories and more coverage from the San Antonio conference in our Women's Imaging Digital Community, at women.auntminnie.com.
Colonoscopy misses right-sided cancer
In other news, a new study published today by Canadian researchers is adding fuel to the debate between optical and virtual colonoscopy. The study of more than 10,000 patients found that patients who underwent optical colonoscopy screening had a 67% reduction in deaths from left-sided colon cancer, but no statistically significant reduction in deaths from right-sided cancer.
An accompanying editorial offers several explanations for the results. But virtual colonoscopy proponents may be wondering if there could be a fundamental flaw in optical colonoscopy that may not occur with the virtual technique. Get more details by clicking here.
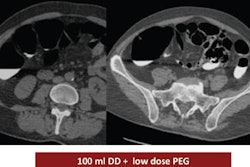
In other virtual colonoscopy news, read about research presented at this month's RSNA meeting in Chicago that analyzed three different types of same-day preparation regimens. Click here for that story, or visit our Virtual Colonoscopy Digital Community at vc.auntminnie.com.













![Images show the pectoralis muscles of a healthy male individual who never smoked (age, 66 years; height, 178 cm; body mass index [BMI, calculated as weight in kilograms divided by height in meters squared], 28.4; number of cigarette pack-years, 0; forced expiratory volume in 1 second [FEV1], 97.6% predicted; FEV1: forced vital capacity [FVC] ratio, 0.71; pectoralis muscle area [PMA], 59.4 cm2; pectoralis muscle volume [PMV], 764 cm3) and a male individual with a smoking history and chronic obstructive pulmonary disorder (COPD) (age, 66 years; height, 178 cm; BMI, 27.5; number of cigarette pack-years, 43.2, FEV1, 48% predicted; FEV1:FVC, 0.56; PMA, 35 cm2; PMV, 480.8 cm3) from the Canadian Cohort Obstructive Lung Disease (i.e., CanCOLD) study. The CT image is shown in the axial plane. The PMV is automatically extracted using the developed deep learning model and overlayed onto the lungs for visual clarity.](https://img.auntminnie.com/mindful/smg/workspaces/default/uploads/2026/03/genkin.25LqljVF0y.jpg?auto=format%2Ccompress&crop=focalpoint&fit=crop&h=112&q=70&w=112)