Dear AuntMinnie Member,
Is the gastroenterology community finally ready to accept virtual colonoscopy (VC)? After years of pooh-poohing the technology, gastroenterologists appear ready to admit that VC (also known as CT colonography) has a role to play in colon screening.
That's the word from this week's International Symposium on Virtual Colonoscopy in Boston, where staff writer Eric Barnes is on hand to report for our Virtual Colonoscopy Digital Community.
In a presentation on Monday, the president of the American Gastroenterological Association's education arm talked about how gastroenterologists and radiologists can work together to bring VC to the masses. Dr. Nicholas LaRusso discussed training, reimbursement, and which technology -- VC or optical colonoscopy -- should be used for which kind of patients. Get the rest of the story by clicking here.
In another article we're featuring in the community, we address the importance of training in achieving adequate diagnostic accuracy in VC screening. A new study by researchers from the Mayo Clinic in Rochester, MN, found that a good training program could increase the sensitivity of novice readers to that of more experienced radiologists.
Read about that story by clicking here, or get the rest of our VC news in the Virtual Colonoscopy Digital Community at vc.auntminnie.com.






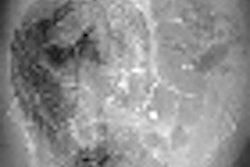






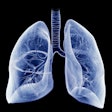

![Images show the pectoralis muscles of a healthy male individual who never smoked (age, 66 years; height, 178 cm; body mass index [BMI, calculated as weight in kilograms divided by height in meters squared], 28.4; number of cigarette pack-years, 0; forced expiratory volume in 1 second [FEV1], 97.6% predicted; FEV1: forced vital capacity [FVC] ratio, 0.71; pectoralis muscle area [PMA], 59.4 cm2; pectoralis muscle volume [PMV], 764 cm3) and a male individual with a smoking history and chronic obstructive pulmonary disorder (COPD) (age, 66 years; height, 178 cm; BMI, 27.5; number of cigarette pack-years, 43.2, FEV1, 48% predicted; FEV1:FVC, 0.56; PMA, 35 cm2; PMV, 480.8 cm3) from the Canadian Cohort Obstructive Lung Disease (i.e., CanCOLD) study. The CT image is shown in the axial plane. The PMV is automatically extracted using the developed deep learning model and overlayed onto the lungs for visual clarity.](https://img.auntminnie.com/mindful/smg/workspaces/default/uploads/2026/03/genkin.25LqljVF0y.jpg?auto=format%2Ccompress&crop=focalpoint&fit=crop&h=112&q=70&w=112)