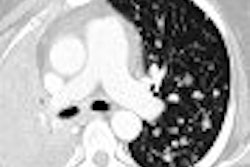
Two papers presented at the 2007 American Society for Therapeutic Radiology and Oncology (ASTRO) meeting in Los Angeles evaluated the management of postradiation head and neck cancer.
In one study, the investigators asked if response to radiotherapy can be used to determine the extent of surgical dissection in positive lymph nodes. A second paper inquired if adjuvant neck dissection can be deferred in patients with complete response to chemoradiation.
Lymph node-positive
"The current approach to the management of the postradiation neck in patients with node-positive squamous cell carcinoma of the head and neck is to either perform a planned neck dissection for all patients with advanced nodal disease, or to evaluate each patient's response to radiation treatment and perform a neck dissection only for those with residual adenopathy," explained Dr. Anamaria Yeung from the Shands Davis Cancer Center at the University of Florida in Gainesville.
"Whether you decide one or the other, neck dissection after radiation usually includes levels I through IV, the idea being that there is a higher risk of microscopic disease throughout the neck," she added. "The downside to this approach is that there is significant morbidity associated with the extent of neck dissection, especially shoulder pain and dysfunction, as well as neck fibrosis."
The question they sought to answer was: "Can we safely dissect only level II and leave the remaining neck levels intact?" Yeung said.
For their retrospective study, Yeung and colleagues included data on 274 patients with lymph node-positive squamous cell carcinoma of the head and neck who were treated between 1990 and 2004 with radiation therapy (median dose of 74.4 Gy). Sixty-nine percent were on a twice-daily hyperfractionated radiation schedule and about half also had chemotherapy, Yeung said.
In addition, the majority of the patients had primary oropharynx cancer, with most patients (71%) exhibiting advanced nodal disease (stage N2B or greater). The minimum follow-up for all patients was two years, while the minimum follow-up among living patients was five years. All patients underwent a postradiation CT scan at four weeks, and the images were read by neuroradiologist Dr. Anthony Mancuso.
"The criteria that we used for a positive lymph node on CT was a size greater than 1.5 cm in greatest axial dimension or the presence of any internal focal defects -- i.e., lucency enhancement or calcifications," Yeung said.
According to the results, 211 heminecks underwent dissection, either planned or because of residual adenopathy on postradiotherapy CT. "For all of these dissections, correlation of nodal response on CT to neck dissection pathology indicated a negative predictive value (NPV) of 100% for level I, 95% for level II, 98% for level III, 96% for level IV, and 96% for level V," the group wrote in its ASTRO abstract.
A subset analysis was done in 61 hemineck levels with initially positive lymph nodes, which responded completely to radiotherapy. In this high-risk scenario, the NPV of post-treatment CT was 95%. Finally, in 71 heminecks that underwent limited dissection, the five-year control rate was 100%.
"If we limit the dissection to level II and leave the remaining levels intact, there's a 5% risk of leaving residual disease behind in the neck," Yeung stated. "This leaves us with one remaining question to answer: Is the potential decrease in morbidity worth the 5% risk of recurrence?"
An ASTRO audience member asked Yeung about the challenge in bringing the idea of partial, targeted dissection to head and neck surgeons. "As you know, there can be a little bristling from asking a surgeon to just dissect level II," he said. "It's akin to a surgical case where someone presents for an oral cavity resection with a couple of small positive nodes in level II and the radiation oncologist (is asked) to only irradiate level II. It would make us bristle. How do you think we can successfully convey this information to head and neck surgeons?"
Yeung replied that at her institution surgeons are willing to consider new options that are in the patient's best interest. She also acknowledged that the best way to convince surgeons of the validity of this approach would be a prospective, randomized trial.
Chemoradiation
In the second talk, Dr. Susannah Yovino and colleagues from the University of Maryland Medical System in Baltimore looked at the clinical data from 145 patients who underwent definitive chemoradiation for locally advanced squamous cell carcinoma of the head and neck.
"At the University of Maryland, our treatment philosophy has been to treat all gross disease, including neck nodes, to definitive radiation doses of 70 Gy. All patients are evaluated two months following the completion of treatment," said Yovino, adding that the clinical evaluation included CT studies. "Patients achieving complete clinical response at the two-month evaluation are observed. Neck dissection is reserved for those patients with residual disease."
The team's goal was to analyze this treatment paradigm by determining survival data, she said. In the study population, the most common disease site was the oropharynx (75%). Almost 72% of the patients had T3 and T4 primary tumors.
In addition to a median dose of 70.2 Gy for radiotherapy, 90.6% of the 145 patients received platinum-based chemotherapy. Of the 145 patients, 72 with N2 or greater disease obtained a complete response to chemoradiation and were selected for observation.
According to the results, 66.7% of the patients marked for observation had no evidence of local or distant disease at a median follow-up of 36 months. Of the remaining patients 29.2% failed, with the most common cause of failure being isolated, distant metastatic disease (11.1%). About 6% of the patients had simultaneous local and distant failures. The median overall survival was 69.8 months.
"Analyzing the failure patterns by end stage shows that advanced nodal disease of the neck did not predict for a higher incidence of isolated neck failure among complete responders, although it is clearly a marker for higher risk, with an increased risk for distant metastases, as well as higher rates of failures at the primary site among N2 and N3 patients," Yovino explained. Among partial responders to treatment, the incidence of nodal failure in the neck was extremely low, she added.
As a result, the authors pointed out that "the predominant site of failure is distant metastatic disease, and it is unlikely that surgical interventional in the neck would alter this pattern of failure."
Eight patients in the cohort ultimately had surgical evaluations of the neck for disease recurrence and four were found to have no evidence of malignancy. They remain disease-free and alive, Yovino said. Three patients underwent neck dissection and therapy, which failed, and they died of squamous cell carcinoma of the head and neck.
"We have concluded that observation following clinically complete response in patients receiving definitive chemoradiation is associated with long-term locoregional control," Yovino said. "We continue to advocate for observation in this patient population."
By Shalmali Pal
AuntMinnie.com staff writer
November 16, 2007
Related Reading
Docetaxel added to standard therapy improves survival in head and neck cancer, October 25, 2007
PET/CT reveals occult metastasis of head and neck cancer, September 7, 2007
Boron neutron capture therapy safe, effective for recurrent head and neck cancer, September 5, 2007
Copyright © 2007 AuntMinnie.com