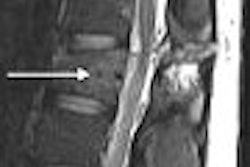
First the good news: Over the past five years, colorectal cancer (CRC) screening rates have risen dramatically among patients at Veterans Affairs (VA) healthcare facilities. The bad news is that more patients than ever are choosing the least accurate test available, the fecal occult blood test (FOBT). Fewer are opting for optical colonoscopy, and the findings stand in contrast to trends in recent Medicare data for reasons that are unknown, VA researchers report.
Another morsel gleaned from a pair of colonoscopy studies and an editorial that appear in the November 13 Archives of Internal Medicine is that sick people in the VA healthcare system may not live long enough to benefit from colorectal cancer screening, though, ironically, patients with significant comorbidities seem to have better access to screening.
The editorial suggests that part of the problem may lie in poor allocation of limited endoscopic resources, adding that virtual colonoscopy remains too unreliable at this time to be considered part of the solution.
Finally, leading virtual colonoscopy researchers who spoke to AuntMinnie.com see VC as an obvious solution to the capacity problem.
More FOBT at VA
Colorectal cancer exacts a grim toll on the population. An estimated 145,290 Americans were diagnosed with the disease last year, while 56,290 died of the disease.
"The past two decades have witnessed important advances in our knowledge of the potential benefits of CRC screening," wrote Dr. Hashem El-Serag, Dr. Laura Petersen, and colleagues in the first featured study. The researchers are from the VA Medical Center and Baylor College of Medicine in Houston, and Case Western Reserve University in Cleveland.
"Fecal occult blood testing followed by colonoscopy in those with a positive test result was shown to reduce CRC mortality by 15% to 33% in several randomized controlled trials," they wrote. "Follow-up results from one of these trials showed that FOBT also reduces incidence. In addition, case-controlled studies have shown that sigmoidoscopy is associated with a 59% to 80% reduction in CRC mortality in the distal colon and rectum. Furthermore, the National Polyp Study, a cohort study, showed that colonoscopic polypectomy is associated with a 76% to 90% reduction in CRC incidence compared with three reference populations" (Archives of Internal Medicine, November 13, 2006, Vol. 166:2, pp. 2202-2208).
The screening guidelines developed as a result of these studies are effective, of course, only to the extent that individuals of screening age comply with them. And in the VA population, patients who wish to be screened are generally given a choice of screening exams: annual FOBT with or without sigmoidoscopy, colonoscopy, and the double-contrast barium (DCBE) enema. Colonoscopy may not always be available; and FOBT, the easiest and cheapest exam, nearly always is.
The researchers examined national VA inpatient and outpatient databases for codes indicative of these exams among patients age 49 to 75 over a five-year period between 1998 and 2003.
According to the results, the frequency of CRC screening tests rose from 432,778 in 1998 to 1,179,764 in 2003. Among patients who were screened, only the proportion of patients screened with FOBT increased, from 81.7% to 90.4%. Over the same period, screening colonoscopy declined from 5.7% to 4.7% of all screening exams (though the total number of screening colonoscopy exams rose from 24,955 in 1998 to 55, 199 in 2003). Flexible sigmoidoscopy dropped from 8.3% to 3.6%, and DCBE declined from 4.1% to 1.3% of all exams. DCBE declined from 4.1% to 1.3% of screening exams.
"A bimodal age distribution was observed, with colonoscopy as the more likely screening modality for persons between the ages of 49 and 55 years, and for those 65 years and older than for those between the ages of 55 and 64 years," the authors wrote.
At the same time, the mean age of VA patients undergoing screening dropped slightly from a median of 64 years in 1998 to 63.2 years in 2003. The age didn't drop as much for FOBT users, and Caucasians constituted a larger proportion of patients undergoing colonoscopy, the most accurate and costly screening exam studied. Women were likelier to have colonoscopy than men, though men comprised 97% of the VA cohort.
"Colorectal cancer screening has dramatically increased in the VA, but unlike in other practice settings, fecal occult blood testing is the dominant mode of screening," El-Serag et al wrote. "Although screening colonoscopy more than doubled in frequency, it constitutes a small proportion of the total CRC screening procedures used in the VA healthcare setting."
Colonoscopy is, of course, the test of choice, while FOBT has been criticized for its low sensitivity, "especially if performed on rectal examination and not serially," the authors noted. For its part, sigmoidoscopy detects only distal lesions, while some studies have noted an increase in the incidence of proximal lesions over time.
In contrast with the VA results, "reports from the Medicare population and endoscopic databases have all documented temporal increases in colonoscopy as a screening modality," they added.
Moreover, the effect of predominant FOBT use in the clinical setting rather than in controlled trials is unclear, and therefore not necessarily worse than colonoscopy, the authors wrote. "It does, however, call for closer examination of the process and outcome of this practice in VA settings," they wrote.
One reason for FOBT's greater use may be the ease of providing it. "More resources are likely to be needed to implement colonoscopy screening compared with FOBT," the authors wrote. "There are trade-offs involved with all CRC screening methods, and individuals have different preferences for screening methods."
"We speculate that some of the differences may be accounted for by patient preferences and characteristics of the healthcare systems, including endoscopic capacity and financial incentives," they wrote.
Screening may be futile in the setting of serious comorbidities
Younger CRC screening patients in poor health with a high risk of comorbid diseases have less chance of deriving a survival benefit from CRC screening, according to the authors of the second study. The researchers sought to examine the relationship between CRC screening, self-reported health status, and comorbidity in patients between the ages of 50 and 64.
The single-center study retrospectively examined data from 861 outpatients who completed a 36-question health survey and the Kaplan-Feinstein Index (comorbidity score) between 1996 and 2004.
Screening rates were examined by age, physical component summary score, and severity of comorbid illnesses, wrote Dr. Shahnaz Sultan, Dr. Jason Conway, Dr. David Edelman, and colleagues from the Duke University Medical Center and the Durham VA Medical Center, both in Durham, NC; the Medical University of South Carolina at Charleston; and the University of Florida College of Medicine in Gainesville.
Among the veterans studied, 45.9% had undergone colorectal cancer screening within five years of their index visit, and screening rates were high among patients with moderate (44.9%) and severe (45.8%) comorbidities, according to the authors.
"When stratified by age group and physical component summary quartile, there was a trend toward increasing screening rates with better health status in the 50- to 54- and 55- to 59-year age groups," they wrote. "In the 60- to 64-year age group, high screening rates for patients with poorer health were observed: physical component summary quartiles 1 and 2, 55% and 54.2%, respectively. Fifty-two patients died during the five-year follow-up; 37 (71.2%) had undergone screening for colorectal cancer" (Archives of Internal Medicine, November 13, 2006, Vol. 166:2, pp. 2209-2214).
Screening rates did not vary by the degree of comorbid illnesses reported, the authors reported.
"While the impact of screening on prolonging life expectancy is demonstrable in healthy patients, in individuals with significant comorbid disease and poor health status, the benefits of screening are not clear," they wrote.
Moreover, screening rates were relatively high among patients with poor health status on the SF-36 PCS scale, a measure of health function and quality of life that has been strongly associated with mortality.
At the VA, colorectal cancer screening is being performed at relatively high rates among younger patients of screening age with potentially reduced life expectancy, the authors concluded.
"This study underscores the importance of incorporating health status in screening decisions for young patients," they wrote. "Individuals with poor health status and diminished life expectancies should potentially not be referred for screening," they added, acknowledging that no guidelines currently exist to accomplish this goal in younger screening-age patients.
A matter of allocation
Encouraging signs of higher screening rates can be found in the comparison of 2002 and 2004 data from the Behavioral Risk Factor Surveillance Series, which showed an increase in the use of endoscopy for screening, wrote Dr. Hemant Roy and colleagues from Evanston-Northwestern Healthcare in Evanston, IL, in an editorial accompanying the two studies (Archives of Internal Medicine, November 13, 2006, Vol. 166:2, pp. 2177-2179).
Unfortunately, "many estimates suggest that entire population would exceed screening capacity. Not only that ... if colonoscopies were actually performed on the entire population of more than 70 million Americans older than 30 years, the annual costs would exceed $10 billion," they noted.
And at this time, virtual colonoscopy cannot be counted on to help fill in the gap in colorectal cancer screening capacity, they stated.
"The exact sensitivities of CT for advanced neoplasia are unclear, with single-center and multicenter estimates vastly differing (> 90% versus 55%)," Roy et al wrote. "Preliminary studies with newer reconstruction techniques have been encouraging, although multicenter validation studies are still pending (ACRIN 6664)."
"However, given the need for bowel cleansing and colonic air insufflation, there was no clear advantage in patient preference between (VC) and colonoscopy," they wrote. "Moreover, because 20% to 30% of patients have adenomas, performing colonoscopy for polypectomy on all patients harboring adenomas would render (VC) noncost-effective. On the other hand, leaving small adenomas in situ may not be acceptable for physicians or patients given the premalignant nature and the occurrence, albeit uncommon, of invasive malignancy (especially in flat and depressed lesions). Because (VC) is expensive, it may be unable to provide CRC screening in a resource-constrained society."
Nevertheless, performing invasive colonoscopy on every individual of screening age is "an inelegant solution," they wrote. Moreover, repeat colonoscopy screening of patients with colonoscopy has a low yield of potentially dangerous polyps, while wasting finite colonoscopy resources that could be better used in patients who are likelier to have advanced adenomas.
Roy et al went on to suggest that various risk stratification techniques, such as genetic modeling, for example, could someday provide accurate assessment of the true risk of invasive malignancy. And if such tests can be developed, the door may be open to less invasive and less accurate screening techniques for screening subjects at lower risk. Experimental models have shown remarkable accuracy for such risk stratification schemes, they report.
"In the interim, we need to encourage more of our patients to be screened," they wrote. "Colonoscopy is clearly the best test, but to make it more widely available, we need to be prudent about repeating studies given the low yield and long-term (10-20 years) lower risk designation achievable with a single negative colonoscopy result."
VC weighs in
Dr. Abraham Dachman, a virtual colonoscopy researcher who is a professor of radiology at the University of Chicago, commented on Roy et al's assessment of VC in an e-mail to AuntMinnie.com.
As for patient preference, "Gluecker et al (Gastroenterology, April 2003, Vol. 124:4, pp. 911-916) have shown a strong willingness of patients to be rescreened with (VC) over optical colonoscopy or barium enema," Dachman wrote.
Still, Roy responded in an e-mail, inasmuch as exam preferences to date have been mixed, it's reasonable to say that there is no clear advantage in patient preference between VC and colonoscopy.
For example, Roy noted, in the landmark study by Pickhardt et al (New England Journal of Medicine, December 4, 2003, Vol. 349:23, pp. 2191-2200), "more patients thought virtual colonoscopy had greater pain then standard (colonoscopy) (54.3% versus 38.1%)," Roy wrote. "With regard to convenience, virtual fared better than standard (68.3% versus 24.1%). For future screening there was a slight preference for virtual colonoscopy 49.8% versus 41.1%."
For his part, the lead investigator of that study, Dr. Perry Pickhardt from the University of Wisconsin in Madison, told AuntMinnie.com that the two exams cannot really be compared for pain because colonoscopy is performed with sedation. Dachman added that Gluecker et al wisely addressed the question of patient preference rather than pain.
Still, many lay people are under the mistaken impression that virtual colonoscopy is essentially like a regular CT scan and discomfort-free, Roy noted in his e-mail.
As for VC's sensitivity, Dachman wrote that "the oft-quoted lower limit sensitivity of 55% for (VC) is based on a trial whose methodology has been seriously questioned by the radiologist" (Radiology, April 2005, Vol. 235:1, pp. 13-16).
"Gastroenterologists and administrators of limited resources can help make cost-effective colorectal cancer screening with (VC) a national reality by accommodating patients who, if properly informed, might chose for (VC) with an option for same-day optical colonoscopy," Dachman wrote.
This practice model, described in the November Radiology by Pickhardt et al, showed a 6.4% referral rate for optical colonoscopy and a 92% positive predictive value for virtual colonoscopy (Radiology, November 2006, Vol. 241:2, pp. 417-425).
"I expect that follow-up data from this and similar screening programs will ultimately support the American College of Radiology practice guidelines and similar recommendations of the Boston Virtual Colonoscopy Working Group (Radiology, July 2005, Vol. 236:1, pp. 3-9) to report only polyps larger than 5 mm, and to consider seven- to 10-year follow-up rather than immediate polypectomy," Dachman wrote.
Dr. Judy Yee, chief of radiology at the San Francisco Veterans Affairs Medical Center in California, agreed with the Roy et al's assessment that colonoscopy capacity is limited, and said that radiology has been similarly constrained.
"Basically, there is lack of manpower (gastroenterologists) to perform screening colonoscopies," she wrote in an e-mail to AuntMinnie.com. "There has also been difficulty recruiting and retaining radiologists throughout the VA system. This hopefully is changing on both fronts with enactment of the VA Physician Pay Bill (January 2006), which helped to increase VA physician salaries particularly addressing those specialties which are difficult to recruit for (radiology) and procedure-oriented specialties (GI) who were very undersalaried."
Yee said that she has worked very hard to encourage the development of VC in the VA system, and that there has been some interest by radiologists to perform VC, particularly at the more academically oriented facilities.
"I have gone out of my way to help (radiologists) get started," Yee wrote. "I have seen much more positive movement over the past year, but it has been a real struggle."
By Eric Barnes
AuntMinnie.com staff writer
November 13, 2006
Related Reading
New data reveal higher efficacy for primary VC screening, October 18, 2006
VC gets long-awaited reporting standards, November 2, 2004
VC finds risky polyps, might reduce polypectomies, June 8, 2006
Gastroenterologist surveys target lesions, VC practice, March 20, 2006
VC would raise screening costs, study concludes, October 31, 2005
Copyright © 2006 AuntMinnie.com