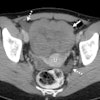
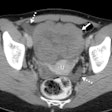
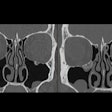
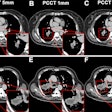
Automated CO2 insufflation improves colonic distension for virtual colonoscopy compared to manual CO2 insufflation, particularly in the left colon, researchers from the U.K. reported in the January American Journal of Roentgenology.
The study, by radiologists at St. Mark's and Northwick Park Hospitals in greater London, isn't the first to conclude that automated CO2 insufflation is superior, but may be the largest peer-reviewed study to date. And unlike most studies, the manual insufflation was performed with carbon dioxide rather than room air.
"Adequate distension is a fundamental prerequisite for CT colonography. A poorly distended colon may either hide or mimic neoplasia, reducing diagnostic confidence and increasing interpretation time," noted Drs. David Burling, Stuart Taylor, Steve Halligan, Louise Gartner, and colleagues (AJR, January 2006, Vol. 186, pp. 96-103).
An alternative method of improving colonic distension, the use of spasmolytic agents like hyoscine butylbromide and glucagon hydrochloride, remains controversial, they added.
"IV hyoscine butlybromide likely improves distension but remains unlicensed in the United States, whereas glucagon hydrochloriate, its licensed alternative, does not appear to be beneficial," the authors wrote.
For their study, the researchers examined 141 subjects with symptoms suspicious for colorectal neoplasia. The first 75 patients underwent virtual colonoscopy following the use of either an automated device (n = 47) (ProtoCO2l, E-Z-EM, Lake Success, NY) or a manual method (n = 94) of carbon monoxide insufflation.
An inexperienced operator was chosen to operate the automated insufflation device (after a one-hour demonstration), in an effort to mimic real-world operating conditions and the normal learning curve. Manual insufflation was performed by a different inexperienced operator using a standard enema bag attached to a rectal catheter, and filled with approximately 3 L of carbon dioxide. For both manual and automated insufflation, additional CO2 was introduced if the scout image suggested suboptimal distension.
The patients maintained a clear liquid diet 24 hours before the exam, and underwent a full bowel preparation using either two packets of magnesium citrate (Citramag, Pharmaserve, Manchester, U.K.) along with one packet of senna granules (Senokot, Reckitt Benckiser Healthcare, Hull, U.K.) (n = 36), or two packets of sodium picosulfate (Picolax, Ferring Pharmaceuticals, Slough, U.K.).
Prior to insufflation, all patients received 20 mg of hyoscine butylbromide (Buscopan, Boehringer Ingelheim, Ingelheim, Germany). A scout CT was obtained before both prone and supine data acquisition to assess the adequacy of distension, and provide for further insufflation when indicated.
CT images were obtained on a four-detector scanner (LightSpeed Plus, GE Healthcare, Chalfont St. Giles, U.K.) at 1.25-mm to 2.5-mm collimation, pitch of 1.5, 120 kVp, 50-100 mAs, and 50% slice overlap, with images reconstructed at half the nominal slice thickness.
The data were analyzed retrospectively by two observers using a dedicated workstation (Advantage Windows 4.0 and Colonography software, GE Healthcare), with prone and supine datasets displayed side by side. The observers, both competent in abdominal radiology but with little direct experience in VC except for a four-hour training session before the study, were blinded to the insufflation method and unaware that two systems were being compared. Distension was assessed on a four-point scale.
The overall distension scores (combining all segments and both scanning positions) showed that distension was significantly greater using the automated insufflator (odds ratio, 1.81 [95% CI, 1.29-2.54] (p < 0.0001).
In individual segments, distension was improved significantly in the sigmoid (p = 0.007) and descending (p < 0.001) colons in the supine data and in the sigmoid (p = 0.02), descending (p = 0.001), and transverse (p = 0.02) colons when supine and prone positions were combined.
"The odds of being in the next highest distension category were more than 2.5 times higher for the sigmoid, and more than four times higher for the descending colon, using automated insufflation," the authors explained.
On the 1 to 4 scale (1 = complete collapse, 4 = optimal distension), the mean distension scores for the automated insufflation group were 3.20 (SD 1.16) and 3.22 (1.12) for the supine and prone scans, respectively.
In supine scanning, no statistically significant association was found between CO2 volumes and luminal distension scores. In prone scanning, however, larger CO2 volumes were associated with significantly poorer distension grades in the sigmoid colon, descending colon, and cecum.
In terms of patient satisfaction, a previously validated questionnaire consisting of 24 questions relating to satisfaction, worry, and physical discomfort was completed by 47 study patients and 94 control patients after virtual colonoscopy. Participants were asked to cross off one box for each question among seven boxes spanning possible responses (ranging, for example, from "no bloating" to "severe bloating"), with a higher score indicating a more positive response.
The sole significant difference between the groups was that patients who received automated insufflation reported being more "weary" (p = 0.03"). The reason for this is unclear, the researchers stated, but may constitute a statistical error.
"We found significantly better luminal distension overall using automated administration than using the manual method," Burling and his team wrote. "The effect was particularly marked for the left colon when the patient was in the supine position and for the transverse colon when both supine and prone scans were combined."
As for the reasons, improved distension using automated insufflation "may be related to the more controlled method of carbon dioxide delivery, allowing greater volumes to be introduced before maximum patient tolerance is reached," they wrote, adding that the constant delivery associated with automated insufflation may also constitute an advantage, compensating for any CO2 absorbed into the bowel before scanning.
Their findings support those of Yee et al, presented at the 2002 RSNA meeting, the authors noted.
Distension is generally better in the prone position, and this advantage could be sufficient to eliminate any advantage for automated insufflation in this position, they suggested.
"Our study does have potential weaknesses," the group cautioned. "All patients but two received IV hyoscine butylbromide to avoid any confounding effect of spasmolytic on distension scores. Therefore, the study does show an advantage of the insufflator, even in patients in whom distension has been optimized in other ways." Still, the results may be less relevant in the U.S., where hyoscine butylbromide isn't licensed. The use of two relatively inexperienced observers to grade distension may have affected the results, the authors added.
"Using an automated carbon dioxide insufflation device is associated with significantly improved colonic distension.... Benefit is greatest in the left colon with the patient supine. No evidence was seen of a significant learning curve with the device," they concluded.
By Eric Barnes
AuntMinnie.com staff writer
December 30, 2005
Related Reading
Automated CO2 insufflation improves VC, December 1, 2004
Electronic CO2 insufflation beats air in virtual colonoscopy, March 12, 2003
Copyright © 2005 AuntMinnie.com