AuntMinnie.com is pleased to present a guest editorial by two heart imaging experts, Dr. John Rumberger and Dr. James Ehrlich, on the use of MDCT versus EBT in coronary CT imaging. If you're interested in writing an alternative viewpoint, please contact us at [email protected].
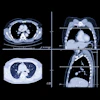
Radiology's enthusiasm for the vast capabilities of multidetector CT technology has grown exponentially with the increase in detector arrays. In many cases the excitement is completely justified: The spatial resolution of new spiral scanners is truly extraordinary, producing strikingly clear images of stationary organs in the body.
At the same time, the search for new radiologic applications for these high-throughput scanners has produced a flourishing cottage industry that was previously the sole domain of cardiologists and cardiac radiologists -- coronary calcium quantification. Now many general radiology groups, that may or may not have formal training in cardiovascular CT, offer "calcium heart score" exams, while others promote more advanced procedures including CT coronary angiography.
At the risk of throwing cold water on contemporary radiology practice, it appears to be an appropriate time to re-examine the value and limitations of the typical MDCT coronary imaging service, as well as the inherent benefit presumptions and risk that lie too quietly under the surface. Certainly lay publications and some physicians are questioning a procedure they believe (incorrectly) to be associated with numerous false-positives, and that exposes the unwary patient to a radiation dose equivalent to "hundreds of chest x-rays."
The question that needs to be asked is: Can calcium scoring conducted on a four- to eight-slice spiral CT (the most common scanner in the U.S. installed base) be justified from a risk/benefit ratio, and can it withstand scrutiny from outside entities like OSHA, medical task forces, and consumer groups?
It's not difficult to question the actual benefit of providing MDCT calcium scoring. One would be hard-pressed to find literature specifically demonstrating that a spiral CT calcium score predicts coronary events, provides value beyond office-based risk assessment, or has histopathologic, nuclear medicine, or angiographic correlations with disease.
On the other hand, there is impressive evidence that electron beam tomography (EBT) imaging provides an index of plaque burden (via the Agatston calcium score) that is a powerful predictor of future hard coronary events, while rampant progression of the calcium volume score on serial examination has independent and worrisome prognostic significance.
Meanwhile, the so-called science behind MDCT calcium scoring is based almost completely on the years of peer-reviewed literature validation from EBT technology, whose superior temporal characteristics are ideally, by design, suited for cardiac imaging applications. It has become commonplace for radiology reports to make clinical recommendations (without appropriate disclosure), borrowing guidelines and patient databases that were published solely for EBT and Agatston calcium-based data.
Acquisition speed is critical for accuracy of coronary imaging, and MDCT spirals are too slow to image the fast-moving coronary arteries without showing motion artifact, especially at heart rates above 70 bpm.
A study by Goldin et al compared 70 asymptomatic patients who were scanned with "sub-16-slice" spirals and EBT, concluding that "spiral CT has not proved to be a feasible alternative to electron-beam CT for coronary artery calcium scoring." There was also concern about high interscan variability and high interreader variability using MDCT. The mean interreader variability of 4.5% for EBT, compared to 41.5 % for spiral CT, prompted the group to suggest double-reading all studies to better assess coronary calcium scores (Radiology, October 2001, Vol. 22:1, pp. 213-221).
Another study demonstrated that four- and eight-slice MDCT scanners frequently mischaracterize true risk, especially when the CAC score is less than 100 (Becker et al, American Journal of Roentgenology, May 2001, Vol. 176:5, pp. 1295-1298).
On a positive note, it appears that the future of cardiac imaging with scanners that have 16 slices and higher may be exceptionally bright compared to those with eight detectors or fewer.
Radiation dose
What about risk? A presentation at the 2003 RSNA meeting revealed the effective radiation dose to sensitive structures (breast) from an MDCT heart scan averaged an alarming 3.7 rads. The presenting radiologist, questioned about the advisability of exposing patients to such doses, said that a careful individual consideration of the risk/benefit ratio should be made in each case before presenting the procedure to the patient ("CT screening exams deliver higher incidental radiation dose to breasts,"AuntMinnie.com, December 4, 2003).
In comparison, the more highly validated EBT heart scan exposes anterior radiosensitive structures to a fraction of that dose, certainly less than 0.5 rads. If one adheres to the ALARA ("as low as reasonably achievable") principle in communities where patients have access to both modalities, the choice of EBT coronary imaging for broad-based screening and clinical indications would be abundantly clear. The switch to EBT would ensure a dramatically improved risk/benefit ratio as compared with the spiral CT alternative.
The journal Progress in Cardiovascular Diseases recently devoted an entire issue (September/October 2003) to the choice of imaging modalities. For a concise discussion of the differences between imaging modalities, we especially recommend Dr. Matt Budoff’s article ("Atherosclerosis Imaging and Calcified Plaque: Coronary Artery Disease Risk Assessment," Progress in Cardiovascular Diseases, September/October 2003, Vol. 46:2, pp. 135-148).
Although radiation concerns are lower in true diagnostic settings, they are of potential relevance to the practice of CT coronary angiography. Patients undergoing MDCT coronary angiography will be exposed to a radiation dose that far exceeds that obtained in a cath lab (conventional angiography). Most patients will also need beta blockade, which introduces additional risks. Electron beam angiography is associated with a small fraction of the radiation dose, and the heart rate does not need to be slowed. The advent of 64-slice scanners should bring coronary calcium imaging at more acceptable radiation doses, as the imaging time shortens appreciably.
A good summary of the radiation exposure during coronary heart scans and CT angiography was published recently in Radiology (January 2003, Vol. 226:1, pp. 145-152).
Technologic considerations aside, radiology groups offering coronary imaging services should be well versed in the clinical significance of the coronary calcium score and how test results may alter conventional risk assessments and therapeutic decisions. Furthermore, the requirements for performing cardiovascular CT by individuals within a specific radiology group should be determined, as there will soon be strict accreditation requirements to practice as a "cardiovascular radiologist."
Since it is clear that a coronary calcium score has the potential to dramatically modify clinical decisions and positively influence patient lifestyle choices, we urge radiology groups to work closely with primary care physicians and cardiologists. The early radiographic identification of coronary disease provides a wonderfully powerful technique to help the referring physician set precise LDL cholesterol goals and provide necessary patient risk factor counseling or reassurance.
Efforts to establish more universal calcium scoring methods, such as "mass score" (integrated area above background) to define a method that would ultimately be machine-independent and accounting for issues such as spatial resolution, field of view, and most importantly, temporal resolution, should be encouraged. (For a further discussion, see Rumberger JA, Kaufman L: "A Rosetta Stone for Coronary Calcium Risk Stratification: Agatston, Volume, and Mass Scores in 11,490 Individuals," AJR 2003; 181: 743-748).
From the viewpoint of experienced EBT plaque imagers who function also as clinicians, we express cautious optimism about the future of 16-slice and higher MDCT calcium scanning procedures pending clinical validation and the development of uniform scanning protocols. Essential to MDCT as an accepted and useful modality for coronary evaluation will be an increased focus upon accuracy, reproducibility, radiation dose, and the formation of clinical standards.
By Dr. John Rumberger and Dr. James Ehrlich
AuntMinnie.com contributing writers
September 3, 2004
Copyright © 2004 AuntMinnie.com
Dr. John A. Rumberger, Ph.D., serves as a clinical professor of medicine at Ohio State University in Columbus, OH, and is medical director of Healthwise Wellness Diagnostic Center, also located in Columbus. Dr. James Ehrlich is adjunct assistant professor at the George Washington University School of Medicine in Washington, DC. He is also medical co-director of Colorado Heart and Body Imaging in Denver, HeartScan of Indiana in Indianapolis, and HeartCheck of Washington, DC. Dr. Ehrlich can be reached at [email protected].