Contrary to perceptions that it's a disease of the past, tuberculosis is still a very real threat. Every year about 2 million people die from TB, and 6 million develop the active disease, according World Health Organization (WHO) estimates. In addition, approximately one-third of the world's population harbors the TB-causing bacterium, Myobacterium tuberculosis, although they may remain asymptomatic.
Developing countries record the highest TB occurrences, but developed countries such as the U.S. are not immune either. About 15 million people in the U.S are infected with the bacteria, according to WHO estimates quoted in a study published earlier this year (RadioGraphics, January-February 2004, Vol. 24:1, pp. 251-256).
The resurgence of TB can be attributed in part to the human immunodefiency virus (HIV) epidemic. Other culprits are adverse social conditions, inadequate infection control practices in healthcare settings, and finally, the emergence of drug-resistant strains of M. tuberculosis.
African countries have the highest rates of the disease, while India and China account for the largest number of TB cases. Together India and China account for 39% of the world’s TB burden with an estimated 1.8 million and 1.4 million TB cases, respectively. For 2001, WHO estimated 8.3 million new cases in the world, although only 2.4 million were reported.
The TB comeback has thrown radiologists a fresh set of challenges. The radiographic features of HIV-related tuberculosis can be quite different. With the HIV pandemic leading to a resurgence of TB, an understanding of the imaging findings can quicken the diagnosis and treatment of the life-threatening disease.
HIV and TB: A dangerous mix
The HIV and TB pathogens interact synergistically at the cellular, host, and population levels. TB trends have been observed to increase in populations with worsening HIV epidemics. Nine percent of all new TB cases in adults between the ages of 15-49 years can be attributed to HIV (Seminars in Respiratory Infection, December 2003, Vol. 18:4, pp. 225-240).
Among AIDS patients, TB is the single leading cause of death. According to WHO estimates, TB accounts for approximately 11% of deaths in AIDS patients. And in Africa, where the HIV epidemic is widespread, TB is responsible for 31% of AIDS deaths.
"HIV infection has both an amplifying and accelerating effect on the natural history of TB ... furthermore, M. tuberculosis infection tends to rapidly progress to active TB diseases among persons with HIV infection," according to the authors of the study published in Seminars in Respiratory Infection. The problem is compounded by delayed TB diagnosis because of the unusual clinical manifestations (such as noncavitary, extrapulmonary, and disseminated TB) in HIV-infected people.
Chest radiograph
The chest radiographic findings of TB vary depending on the severity of the immune deficiency. Cavitary lesions that are classic in HIV-negative adults are very unusual among patients with advanced HIV disease. In contrast, intrathoracic adenopathy, which is not very common, is a fairly common feature in HIV-related tuberculosis, as is pericardial involvement, nodular infiltrates, and lower and middle lobe infiltrates.
Interestingly, patients with HIV-related pulmonary tuberculosis have lower rates of sputum smear positivity, but comparably high rates for culture positivity. When adjusted for chest radiographic pattern, the yield of sputum smear is the same in both patient categories.
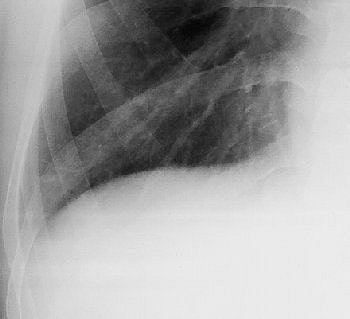 |
| Image A. Paradoxical response to antituberculous medication for tuberculous pleural effusion in a 29-year-old man. Magnified frontal chest radiograph, obtained a month after detection of right pleural effusion, shows that the pleural fluid has disappeared. No lung nodule or mass is evident in the right lower lung. |
Chest radiography can also be used as a screening tool for prevention. In high-prevalence countries, an x-ray exam is recommended by WHO/UNAIDS before starting isoniazid preventive therapy for HIV-related TB.
"HIV is recognized as the strongest risk factor for progression of the latent Myobacterium tuberculosis," wrote Dr. Barudi Mosimaneotsile and colleagues with the Centers for Disease Control and Prevention (Lancet, November 2003, Vol. 362:9395, pp. 1551-1552).
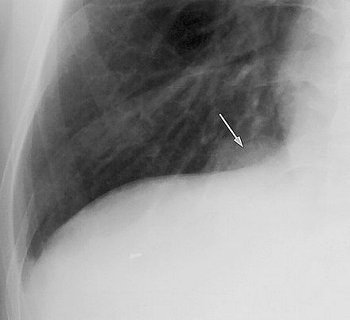 |
| Image B. Magnified frontal chest radiograph, obtained eight months after image A, shows an ill-defined mass (arrow) above the right side of the diaphragm that is not evident in image A. The lesion was classified as radiographically uncertain in origin. |
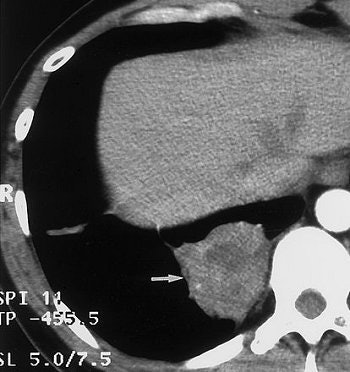 |
| Image C. Transverse contrast-enhanced chest CT scan (5-mm collimation), obtained through the right half of the diaphragm at the same time as image B, shows that the mass in image B results from an inhomogeneously enhancing pulmonary lesion (arrow) abutting the pleura. The mass disappeared nine months later with use of antituberculous medication. Figures 2a, b, c, Choi, YW, Jeon SC, Seo HS, et al, "Tuberculous pleural effusion: New pulmonary lesions during treatment," (Radiology 2002; 224: 493-502). |
However, Mosimaneotsile's group noted that radiography may not be feasible in countries with limited resources. For those developing countries where radiologists are short in supply, telemedicine can be an alternative.
The diagnostic accuracy of chest x-rays acquired with a digital camera for low-cost teleradiology was explored in a multicenter study out of Boston. The study concluded no statistical difference existed in the overall performance between the original film and the JPEG and JPEG 2000 images used for telemedicine.
"Our preliminary results show the potential usefulness of this technique particularly for tuberculosis and lung disease," said Dr. Agnieszka Szot and colleagues (International Journal of Medical Informatics, February 2004, Vol. 73:1, pp. 65-73).
CT
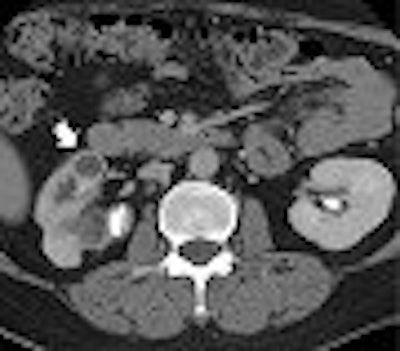
In extrapulmonary involvement cases, the genitourinary system is one of the most common sites of involvement, and CT can facilitate diagnosis. CT is the most sensitive modality for identifying renal calcifications, which occur in over 50% of genitourinary tuberculosis cases (RadioGraphics, February 2004, Vol. 24:1, pp. 251-256).
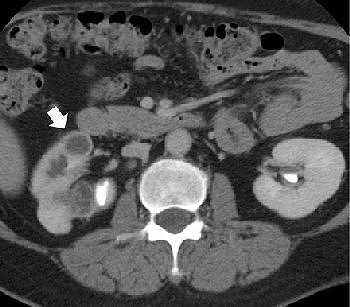 |
| Image A. Contrast-enhanced nephrographic-phase CT scan shows dilated calices and thinning of the renal cortex (arrow). |
With conventional radiography, renal calcifications are a common manifestation of tuberculosis occurring in 25% to 44% of patients. CT is useful in determining the extent of renal and extra renal spread of the disease. Coalesced cortical granulomas and parenchymal scarring is apparent at CT, while fibrotic structures of the renal pelvis and ureters may be seen on contrast-enhanced CT, suggesting tuberculous infection.
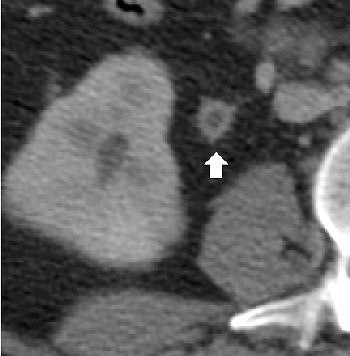 |
| Image B. Magnified view from a contrast-enhanced nephrographic-phase CT scan, obtained caudad to image A, shows mural enhancement and thickening of the proximal ureter (arrow). Figures 2a, b, Gibson MS, Puckett ML, Shelly ME, "Renal Tuberculosis," (RadioGraphics 2004; 24: 251-256). |
Abdominal tuberculosis, usually a manifestation of disseminated disease, on CT or ultrasound shows enlarged retroperitoneal and mesenteric nodes, often with hypodense lesions. Disseminated disease, or the involvement of two more noncontiguous extrapulmonary sites, is associated with advanced HIV disease, according to the study in Seminars in Respiratory Infection.
CT is also ideal for evaluating tuberculous chest wall lesions because it demonstrates the nature and extent of soft-tissue collections and accompanying adenopathy and bone erosion, according to a research paper in the British Journal of Radiology (May 2004, Vol. 77:917, pp. 449-457).
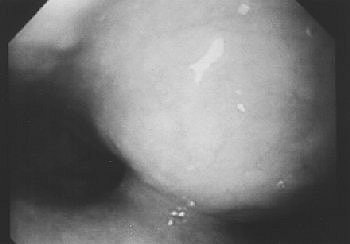 |
| Fifty-year-old woman with submucosal tuberculous abscess in esophagus. Endoscopic image shows smooth-surfaced extraluminal mass of distal esophagus protruding into lumen with overlying mucosa intact. Lee KH, Kim HJ, Kim KH, Kim HG, "Esophageal Tuberculosis Manifesting as Submucosal Abscess," (AJR 2003; 180: 1482-1483). |
CT scores over ultrasound in this aspect. The BJR study cites a case in which abscesses on the inner surface of the parietal wall indented the contour of the liver and was mistaken for a diseased gall bladder on initial ultrasound.
In congenital tuberculosis, CT and x-ray can help in tracing the infection route without surgery or autopsy. If an infant has a proven tuberculous lesion and a primary hepatic complex on imaging, diagnosis of congenital TB can be made (American Journal of Roentgenology, January 2004, Vol. 183, pp. 253-256).
MRI
Pericardial abscess occurring as a complication of tuberculous pericarditis can be studied both on CT and MRI. Information on the location and extent of the pericardial abscess can be useful inputs for deciding the surgical approach and in selecting the optimal path for guided needle aspiration (Clinical Radiology, June 2004, Vol. 59:6, pp. 514-519).
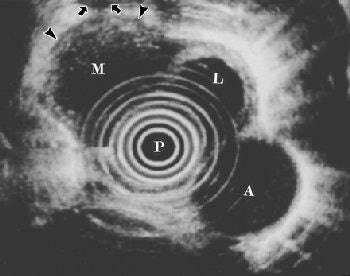 |
| Fifty-year-old woman with submucosal tuberculous abscess in esophagus. Esophageal endosonogram shows relatively well-demarcated heterogeneously hypoechoic mass (M) containing scattered echogenic debris in esophageal wall. Surrounding adventitia (arrowheads) appears somewhat irregular. Note small hypoechoic periesophageal lymph node (arrows) external relative to esophagus. L = fluid-filled esophageal lumen, P = center of probe, A = descending thoracic aorta. |
Imaging on MRI and CT have the advantage of being less operator-dependent, and are not limited by a poor acoustic window compared with echocardiography. MRI, in addition to having no radiation risk, is sensitive especially for detection of small effusions. However, MR findings do not provide any disease-specific image morphology.
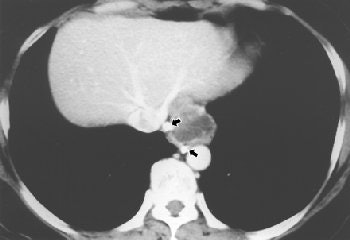 |
| Fifty-year-old woman with submucosal tuberculous abscess in esophagus. Contrast-enhanced axial CT scan shows relatively well-marginated cystic mass at distal esophagus. Thick, partially calcified enhancing rim is noted at periphery of mass. Calcified small periesophageal lymph nodes (arrows) are adjacent to mass. Lee KH, Kim HJ, Kim KH, Kim HG, "Esophageal Tuberculosis Manifesting as Submucosal Abscess," (AJR 2003; 180: 1482-1483). |
Line scan diffusion-weighted MR images, as well as contrast-enhanced CT and esophageal endosonogram, can be used for diagnosis and evaluation of esophageal tuberculosis, which is relatively rare and found in less than 1% of patients who die of TB (AJR, May 2003, Vol. 180:5, pp. 1482-1483).
A stronger strain of TB
Deficient infection control practices have resulted in the appearance of drug-resistant strains of M. tuberculosis. Multidrug-resistant TB (MDR-TB) does not respond to the two most potent anti-TB antibiotics (isoniazid and rifampin), and it is complicated and more expensive to treat.
Because of limited public health infrastructure and expertise, many countries with a high TB burden cannot reliably treat MDR-TB, resulting in the generation and transmission of new strains of M. tuberculosis. The highest rates of drug resistance and MDR are found in certain provinces and states of China and India, in Mozambique, and in some of the newly independent states of the former Soviet Union.
But help is on the way. Most recently, the Bill and Melinda Gates Foundation bestowed a $45 million grant to study the HIV/TB connection on the Consortium to Respond Effectively to the AIDS-TB Epidemic (CREATE). The group is led by scientists at the Johns Hopkins Center for Tuberculosis Research in Baltimore. Earlier in 2004, the Gates foundation donated $82.9 million for research into a TB vaccine.
Devising a better way to diagnose TB is also paramount. The Mantoux skin test, the current gold standard for TB testing, has been around since the 19th century, and wields only a 50% success rate in detecting TB in HIV patients, according to Médecins Sans Frontières, or Doctors Without Borders. And WHO's Directly Observed Treatment, Short-course (DOTS) strategy for assessing TB is already a decade old, the group noted (Reuters Health, March 23, 2004).
Whether imaging can provide the definitive TB screening test remains to be seen. While a lack of funding and resources may preclude experimentation in the countries that contend with the highest TB infection rate, radiologists in developing nations may get the chance to fire up better TB screening methods in their own backyard. The Centers for Disease Control and Prevention recently reported that patients who take TNF-alpha antagonists -- widely prescribed to treat rheumatoid arthritis and Crohn's disease -- have an increased risk of TB, and should be closely monitored for the disease (Morbidity and Mortality Weekly Report, August 6, 2004).
By N. Shivapriya
AuntMinnie.com staff writer
August 12, 2004
Related Reading
CT, MRI aid pericardial abscess evaluation, July 21, 2004
SARS screening reveals TB in Taiwanese healthcare workers, April 23, 2004
Chest x-ray not necessary to detect active TB in HIV-infected patients, November 7, 2003
Indian doctors tend to rely on x-rays for diagnosis of pulmonary tuberculosis, January 13, 2003
Copyright © 2004 AuntMinnie.com