The results of virtual colonoscopy trials have been all over the map, with reported sensitivities for detecting clinically significant polyps (1 cm and larger) ranging from approximately 50% to 90%.
Variations in equipment, (such as single vs. multidetector-row scanners), differences in interpretation methods (such as 2-D vs. 3-D primary read), and the rapid evolution of CAD, have confounded attempts to compare recent trials with older studies.
Then there are the VC study cohorts, which have included everyone from low-risk screening populations to symptomatic adults to individuals with a history of polyps or cancer. According to a study published in the November Radiology Online, much of the variation in results can be attributed to the wide mix of patients who have chosen to participate in virtual colonoscopy trials. But more detailed and consistent results will be needed to move VC into the mainstream.
"Radiologists face the important transition from early advancements in imagery and feasibility studies in academic institutions to validation of this technique in generalizable environments," wrote lead investigator Dr. Elizabeth McFarland and colleagues from the Washington University School of Medicine in St. Louis. Also participating in the study were researchers from Yale University in New Haven, CT, and the University of Vermont in Burlington.
"This critical transition will be enabled, in part, by clearly defining the current status of diagnostic performance and the factors that influence it. Such results may help focus future efforts in diagnostic evaluation and community implementation," they wrote.
To that end, the goal of the study was the prospective evaluation of multiobserver diagnostic performance and reader agreement for colorectal polyp detection in a cohort of polyp-rich patients, using conventional colonoscopy as the reference standard.
The 70 individuals recruited for the study (26 women, 44 men, ages 28-82, average age 62 years) underwent same-day virtual and conventional colonoscopy. All of the patients were suspected of having polyps or had proven polyps on recent flexible sigmoidoscopy, and were scheduled for conventional colonoscopy.
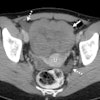
One day before the procedures, subjects underwent standard bowel cleansing with the recommended dietary restrictions. Then, following manual colon insufflation, the subjects underwent virtual colonoscopy in both the prone and supine positions on a single-detector spiral CT scanner (either Somatom Plus 4, Siemens Medical Solutions, Malvern, PA; or Proscan, GE Medical Systems, Waukesha, WI) using 5-mm collimation, 8-mm table increment, 200 mAs, 120 kv, and a 2-mm reconstruction interval.
Following CT image acquisition, the subjects went directly to conventional colonoscopy, performed by two experienced gastroenterologists who recorded the size and location of each polyp.
CT image analysis was performed by four experienced abdominal radiologists with a mean of 12.3 years of faculty-level body CT experience. Each of the readers had been extensively trained and tested in virtual colonoscopy interpretation.
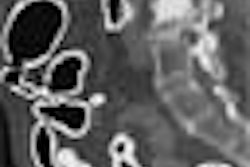
Each radiologist reviewed all 70 datasets (reading prone and supine together) using 2-D multiplanar reformations that provided interactive viewing of the entire dataset, combined with 3-D endoscopic views to further characterize individual findings.
"The window display setting was chosen empirically to provide high contrast for polyp detection while preserving some soft-tissue detail to discriminate extraluminal findings, including diverticula, lipomas, and wall abnormalities," the authors wrote. A soft-tissue window display was used occasionally for problem-solving.
The readers rated image quality and confidence for the presence of a polyp on a scale of 1-5, 5 meaning a polyp was definitely present. The results were correlated with the CT findings with regard to both true- and false-positive lesions, and the results analyzed quantitatively.
The gastroenterologists found 157 colorectal lesions at colonoscopy, including 72 polyps 4-5 mm, 45 polyps 6-9 mm, and 40 lesions 1 cm and larger. Of the larger lesions, 29/40 occurred in the rectosigmoid, and three lesions were advanced wall cancers, including two sigmoid and one cecal, the authors wrote.
Excellent CT visualization was noted for most segments, with the lowest visualization scores (16% poorly visualized) in the sigmoid colon.
Pooled results showed that virtual colonoscopy had a per-polyp sensitivity of 68% for the detection of lesions 10 mm and larger, with 75% agreement among the four readers. Per-patient results were better: 88% for patients with lesions 10 mm and larger, with 94% reader agreement, which peaked at the 10-mm polyp size.
"Interobserver agreement per patient was 79% for all patients, 73% for patients with 6-9 mm polyps, and 94% for patients with 10-mm or larger polyps," according to the authors. "Variability in interobserver agreement did not appear to be related to differences in image quality (e.g., collapse or fluid retention) but may have been due to differences in reader style or persistence of detection with multiple findings."
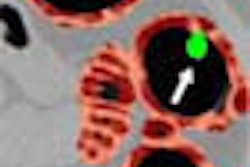
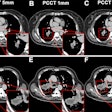
The addition of 3-D perspective volume rendering with color was found to be helpful in identifying true positives. Among 157 colorectal lesions 4 mm and larger, there were 13 cases in which the addition of 3-D PVR to 2-D MPR changed the positive or negative status of a lesion.
"In the majority of these cases, the additional use of 3-D PVR correctly changed the finding from false-positive to true-negative," the authors wrote, noting that further developments in 3-D image processing such as automated flight paths, extended field-of-view displays, stool tagging and subtraction, and CAD, will require further evaluation.
The group also considered the possibility that a priori knowledge of the polyp-rich cohort might skew the results toward positive diagnoses. However, they found that just 2 of 98 positive diagnoses were based exclusively on a false-positive polyp.
Based on good sensitivity and high interobserver agreement for clinically significant polyps, the results are promising, and are a much-needed effort to assess multiobserver performance of the technique.
However, the authors noted, "each study represents only one stage of assessment along a curve of continual change of acquisition and image-display advances." Moreover, the expectations of the test also need to be evaluated. Should virtual colonoscopy screening be designed to detect every clinically significant polyp?
"Multidisciplinary collaboration will be useful to develop clinical management algorithms, which could help define the lower limits of polyp sizes that are clinically relevant in different patient cohorts, stratified by age, a priori risk, and comorbidity," the group concluded. "Evidence-based outcome analyses can then provide a framework for implementing efficient study designs and help assess cost-benefit considerations. Ultimately, future evaluations will determine the role of CT colonography among diagnostic tools intended to reduce colorectal cancer mortality."
By Eric BarnesAuntMinnie.com staff writer
November 27, 2002
Related Reading
VC screening trials find good sensitivity, high patient acceptance, October 30, 2002
Future looks bright for virtual colonoscopy, June 3, 2002
Copyright © 2002 AuntMinnie.com