Advocates of breast MRI screening won a major victory in 2007, when the American Cancer Society (ACS) published new guidelines recommending that women at high risk for breast cancer augment their annual mammogram with an annual breast MRI. But breast MRI proponents shouldn't rest on their laurels, as more work remains to ensure that breast MRI screening is available to all women who would benefit from it.
The ACS guidelines are applicable to an estimated 1.4 million to 1.6 million women in the U.S., and in general state that MRI screenings should be provided in addition to annual mammography for women with certain risk factors, such as BRCA1 or BRCA2 genetic mutations or a lifetime risk of breast cancer of 20% to 25% (see sidebar for additional criteria).
ACS based its decision on a growing body of evidence pointing to the effectiveness of breast MRI in a screening environment for high-risk women. The first data published, in 2000, about multimodality screening at the University of Bonn in Germany of women at high genetic risk, demonstrated that the sensitivity of breast MRI was more than double that of mammography and ultrasound combined. This pioneering work by Dr. Christiane Kuhl, vice chairman and professor of radiology, stimulated other researchers to conduct similar studies that validated these findings.
One of the university's most recent prospective studies revealed that breast MRI doubled the sensitivity of diagnosing ductal carcinoma in situ (DCIS) and high-grade DCIS in particular, as compared to digital mammography. MRI was positive in 92% of cases, while mammography was positive in only 56%, according to Kuhl, who presented the study in 2007.
Research has yet to prove that breast MRI screening impacts the morbidity or mortality of a patient diagnosed with breast cancer. But from the perspective of a high-risk woman, breast MRI screening that detects a cancer at an earlier stage may allow the option of a lumpectomy instead of a mastectomy, and adjuvant treatment that is less debilitating.
Some 5% to 10% of all breast cancers are attributed to mutation in a breast cancer susceptibility gene. Women with BRCA1 and BRCA2 mutation genes have an average lifetime risk of between 60% and 85% for breast cancer, and have an estimated risk for a second primary breast cancer of up to 60%. This cohort represents up to 50% of all familial cancers, the others occurring in women with a strong family history of breast cancer who are suspected as having yet-to-be identified gene mutation. By comparison, the average woman has a 10% to 12% lifetime risk of acquiring breast cancer.

“Breast MRI exams, used in conjunction with mammography and ultrasound on a
case-by-case basis, make screening of young high-risk women much more effective.”
— Dr. Christiane Kuhl,
University of Bonn, Germany
Because familial and hereditary breast cancer tends to occur when women are young and tends to be aggressive, frequent screening is recommended starting at age 30, or as early as 25 if a family member had breast cancer at age 30. For these women, mammograms may not be as diagnostically accurate, and the cumulative radiation dose may be more detrimental than with the average woman.
Clinical trials conducted between 2000 and 2007 in the U.S., the U.K., and other countries in Europe demonstrated that multimodality surveillance programs for these high-risk women substantially improve the early diagnosis of breast cancer.
Women at the age of 30 will have much denser fibroglandular tissue, and high parenchymal density is linked to a higher absorption rate of x-rays compared to involuted breasts, Kuhl said. Also, the BRCA1 mutation is believed to be associated with increased radiosensitivity. Because familial breast cancer tends to exhibit aggressive biologic behavior, short screening intervals are recommended. In addition to the difficulty of interpreting mammograms of dense breasts, BRCA1-associated breast cancers tend to have benign morphologic features and only rarely exhibit calcifications.
Breast MRI can counteract most of these issues. "Breast MRI exams, used in conjunction with mammography and ultrasound on a case-by-case basis, make screening of young high-risk women much more effective," Kuhl said.
Building momentum
For some breast specialists, the ACS guidelines justified the recommendations they had been making all along to their high-risk patients. At Breast Imaging of Oklahoma in Edmond, breast MRI screening had been an integral component of a pioneering high-risk program from its inception in February 2003, according to Melissa Craft, R.N., Ph.D., program director and clinical oncology nurse.
But in some cases, word has been slow to get out about the availability of breast MRI as a screening tool. Breast imaging center administrators report that many high-risk women presenting for mammograms or other procedures say that the ACS breast MRI guidelines were never discussed with them by any other medical professional prior to their arrival. The majority of referrals that originate from the medical community are originating from genetic counselors, breast surgeons, and gynecologists.
The situation is different at facilities or radiology practices with renowned experts in breast MRI. These sites are experiencing a surge of interest from patients, a trend that first became evident several months after the release of the ACS guidelines.
Dr. Steven Harms, a breast imaging specialist who started using breast MRI in the early 1990s, reports that the number of independent inquiries from both regional patients and those from out of state have increased dramatically at his facility, Breast Center of Northwest Arkansas in Fayetteville.
In addition, easy Internet access to information and increased media coverage are educating women independent of their physicians. Celebrities such as actress Christina Applegate, who publicly attributed a breast MRI exam to the early detection of familial breast cancer, are also increasing public awareness.
Radiology practices are educating referring physicians by including the ACS guidelines within their mammography reports, but are not marketing breast MRI screening directly to patients. The procedure currently is not recommended for the majority of women with an average risk of 10% to 12%, or even women with a moderate risk of up to 20%.
Even among some high-risk women, breast MRI screening sometimes can be a tough sell. As part of a substudy of the American College of Radiology Imaging Network (ACRIN) digital mammography clinical trial, participants were invited to have a breast MRI at no cost -- and 40% declined, according to Dr. Wendie Berg, Ph.D., a breast imaging specialist at American Radiology Services in Baltimore.
Berg and colleagues will present their findings in detail at the 2008 RSNA meeting in Chicago, but she noted that claustrophobia and fear of potential side effects of contrast agents were among the primary reasons ACRIN participants declined the offer.
Ramping up
Demand for breast MRI screening is still projected to rise, however, and breast imaging facilities are ramping up to meet it, as well as significantly increased use of breast MRI for diagnosis and staging. Breast MRI training courses proliferating throughout the country are filled to capacity.
"Only sites with significant experience in diagnostic breast MRI should accept patients for screening MRI."
— Dr. Constance Lehman, Ph.D.,
University of Washington
School of Medicine and
Seattle Cancer Care Alliance, Seattle
The clinical and administrative team of Mount Carmel Imaging Center in Columbus, OH, headed by medical director Dr. Dan White, developed an online computer-based program containing teaching files, a comparison of equipment and breast MRI computer-aided detection (CAD) software, an overview of scanning and hanging file protocols for diagnostic workstations, and comprehensive information about establishing a breast MRI program.
"When we started eight years ago, there was no place to go to learn how to set up a breast MRI program," White said. "It requires lots of hours, particularly in private practice, to keep up with the workload, both with respect to performing and interpreting the studies and managing all the documentation and paperwork required to maintain patient records and to obtain reimbursement."
White believes it is important for private practices to offer breast MRI as a women's imaging service, but it needs to be done correctly. He does not recommend that a center initiate a high-risk screening program at start-up; instead, it should move into screening after first getting experience in diagnostic breast MRI.
That opinion is echoed by Dr. Constance Lehman, Ph.D., vice chair of radiology and head of breast imaging at the University of Washington School of Medicine in Seattle and director of radiology of the Seattle Cancer Care Alliance. "Only sites with significant experience in diagnostic breast MRI should accept patients for screening MRI," she said.
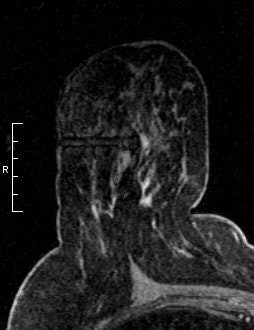 The ability to offer MR-guided biopsy is key to any screening program. In this case, MR-guided biopsy helped identify a 5-mm invasive ductal cancer and high-grade solid-type in situ carcinoma. The patient elected mastectomy.
Image courtesy of Dr. Bruce Porter, |
She and other breast imaging experts recommend that the availability of MR-guided intervention should be a mandatory prerequisite for offering breast MR imaging. In 2001, lack of access to MR-guided biopsy was identified as the single major reason for the delayed adoption of breast MRI in clinical practice.
Technology and equipment innovations of the past seven years have minimized this roadblock. If a facility is not equipped to perform an MRI-guided biopsy, it should partner with a local facility that is.
Workflow of breast MRI screening
Breast MRI equipment is typically scheduled at capacity, and the "tag team" approach used at Memorial Hospital West in Pembroke Pines, FL, may be typical. While one technologist is preparing one patient, another technologist is performing the scan on another.
One MRI technologist interacts with the patient to complete the patient questionnaire, asks the patient if she has questions and answers them, reviews MRI safety protocol to verify that the patient doesn't have a pacemaker or aneurism clips, and verifies that all prior mammograms, ultrasounds, and/or breast MRI films or DICOM CDs have been received.
"We want our patients to be comfortable, and if we sense that the patient is claustrophobic, we need to address that issue, too," explained Aymet Guerrero, chief MRI technologist. "If a patient is claustrophobic, we would prefer to determine this in advance."
A breast MRI scan takes 30 to 60 minutes, according to Guerrero. She and her colleagues perform up to 10 scans per day, a volume they say has nearly doubled in the past 12 months.
Reading workflow is a matter of preference, according to the radiologists interviewed. Exam worklists are configured as shown below:
- All breast imaging -- mammography, ultrasound, and breast MRI
- Diagnostic mammograms and all breast MRI
- Breast MRI only -- both screening and diagnostic intermingled
- Breast MRI diagnostic only and breast MRI screening only, segmented by category
It takes an experienced reader an average of five to 10 minutes to read a breast MRI screening study. If cancer is suspected or diagnosed, review and interpretation, even with the assistance of breast MRI CAD, increases to 20 to 60 minutes.
Reducing recalls and false positives
Conventional wisdom is that high recall rates and a high level of false positives are the Achilles' heels of breast MRI. But the prevalence of both can be reduced when studies are read by more experienced radiologists.
In one study, led by Dr. Ellen Warner at Toronto-Sunnybrook Regional Cancer Centre in Ontario, researchers documented a decline in the breast MRI recall rate from 26% in the first year of screening to 13% in the second year, and a leveling out of 10% in the third year. A recall rate ranging from 8% to 17% was reported in the results of clinical studies between 2000 and 2007. A 10% recall rate is comparable to the recall rate of mammograms.
Harms at Breast Center of Northwest Arkansas recalls approximately one patient out of every 100 who is screened on an annual basis. Recall rates of 10% are more common, especially with patients having their first breast MRI, which often reveals potentially suspicious findings that were not visible on mammograms.
 Breast MRI can detect pathology not found on conventional mammography. Breast MRI scan (right) shows ductal carcinoma in situ not found on mammography image (left). Images courtesy of Dr. Christiane Kuhl, University of Bonn, Germany. |
"Breast MRIs should be read by experts in breast imaging. Radiologists who do not have this experience will be making their interpretations in a vacuum," said Dr. Stephen Feig, director of breast imaging at Aurora Breast MRI of Orange County in California. "It is important to compare prior mammograms, prior breast ultrasounds, and prior breast MRI. This helps keep the callback rate lower."
As compared to textbooks and image databases of mammograms, reference material for consultation is much more limited for breast MRI, Feig noted. "Interpreting a breast MRI, even with the use of breast MRI CAD which helps with the diagnosis, is an art as well as a science, based on clinical knowledge, practical experience, and intuition," he said.
Mount Carmel Imaging Center maintains an average sensitivity of 95%, a specificity of 97.8%, a positive predictive value (PPV) of 89.2%, and a negative predictive value (NPV) of 99% for all the breast MRIs it performs. That compares to statistics in the literature pointing to an overall a sensitivity range of 85% to 95%, a specificity range of 88% to 98%, a PPV of 24% to 71%, and an NPV of 95% to 99%.
At Memorial Healthcare System of Hollywood, FL, all new mammographers are asked to read five to six breast MRIs a week, according to Dr. Daisy Frau-Reyna, a radiologist specializing in breast imaging. Frau-Reyna reviews their findings before reports are submitted.
"As with mammography, the volume you read increases your proficiency and efficiency," she said. "It's important that mammographers become experienced with this procedure. It's becoming an intrinsic component of breast imaging."
What about lower-risk women?
Given breast MRI's utility in high-risk women, to what extent should it be used for women of average and moderately high risk? On this issue, opinions diverge.
"In view of the greatly superior diagnostic power of virtually all possible clinical scenarios, it is not justifiable to discourage the use of breast MR as an adjunct to mammography for individualized screening of women at average risk," Kuhl said.
But this application is not considered feasible, for numerous reasons:
- There are not enough qualified radiologists to interpret breast MRIs, nor the facilities to perform them to meet the needs of even women at high risk.
- The procedure averages at least $1,000, and the cost would be borne by the patient.
- Positive predictive value will be lower, with higher risk of unnecessary biopsies.
“I believe that mammography is going to be replaced by MRI
as the standard for
breast screening.”
— Dr. Ferris Hall,
Beth Israel Deaconess Medical Center and Harvard Medical School, Boston
Another proponent of greater access to breast MRI screening is Dr. Ferris Hall of Beth Israel Deaconess Medical Center and Harvard Medical School, both in Boston. "I believe that mammography is going to be replaced by MRI as the standard for breast screening," he wrote in the June 2008 issue of Radiology.
In an interview with AuntMinnie.com, he noted that the use of a 20% lifetime risk of cancer for referring women to breast MRI screening was arbitrary, and that a woman with a lifetime risk of just 12% should deserve the same treatment.
Hall predicts that new technology will make breast MRI easier to interpret and reduce the cost of the equipment. "Clinical trials may prove that screening is needed only in 24- versus 12-month intervals," he said. "We just don't know."
What is known is that breast MRI screening guidelines are sound, and while new technologies may supersede this, if the U.S. is serious about early breast cancer detection for high-risk women, breast MRI is a vital tool.
By Cynthia Keen
AuntMinnie.com staff writer
September 2, 2008
Copyright © 2008 AuntMinnie.com