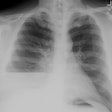
Localized Fibrous Tumor of the Pleura:
Clinical:
Solitary fibrous tumors most commonly arise from the pleura, but it can also occur in extrathoracic locations including the head and neck, soft tissues of the proximal extremities, and abdomen [8]. The lesion is a mesenchymal fibroblastic tumor with a prominent hemangiopericytoma-like branching vascular pattern [9]. Intracranial hemangiopericytoma has been reclassified as an extrathoracic solitary fibrous tumor due to the presence of the same gene fusion (NAB2-STAT6) [8]. There are two subtypes- fibrous and cellular [9]. The fibrous lesion is more common and contains an abundant fibrous stroma [9]. The cellular subtype is less common and demonstrates moderate to high cellularity, little intervening fibrosis, and is hypervascular with numerous thin-walled staghorn branching vessels [9]. The metastatic rate is much higher for cellular solitary fibrous tumors (25% vs 5% for fibrous lesions) [9].Localized fibrous tumors of the pleura are rare (accounting for less than 5% of pleural tumors), slow growing, encapsulated mass containing spindle cells and collagen which originates from submesoepithelial mesencymal cells in the visceral (70-80%) or parietal (20-30%) pleura, rarely the lesion can arise in the pulmonary parenchyma. Males and females are affected equally and most patients are over the age of 50 years. There is no relationship to asbestos exposure or cigarette smoking [6]. Most patients are asymptomatic (50%), but may present with cough, chest pain, or dyspnea. The lesion is generally benign (60-80%), but may behave malignantly (10-40%). Pedunculated lesions are typically benign, and pedunculated tumors (both benign and malignant) have the best prognosis. Note that metastatic disease can be seen with both benign and malignant solitary fibrous tumors [8]. Thoracic solitary fibrous tumors most commonly metastasize to the pleura, but peritoneal metastases are also common, particular in patients with pleural mets [8].
Approximately 20% of pleural lesions are malignant, but this does not imply a poor prognosis. Signs of malignancy and a greater risk for metastatic disease include: size larger than 10 cm, internal hemorrhage or necrosis, a sessile lesion, a child/adolescent, an ipsilateral pleural effusion, or high mitotic activity (≥ 4 mitoses per HPF [8]). Generally, malignant lesions are radiographically indistinguishable from those with benign histology [6]. Extrathoracic lesions are also more likely malignant [8].
Extrathoracic manifestations associated with the tumor have also been described and are more commonly associated with large tumors [6]. Hypertrophic osteoarthopathy (HOA) can be found in 4% to 35% of cases and its presence suggests a benign lesion. Finger clubbing can be found in 4%, and episodic hypoglycemia (also rare- 4% of cases). HOA and hypoglycemia both resolve following resection and recur with tumor recurrence. The fibrous and acellular nature of these tumors makes their diagnosis by transthoracic needle biopsy difficult. Treatment is complete excision and there is a 10-12% local recurrence rate (generally these are non-pedunculated lesions).
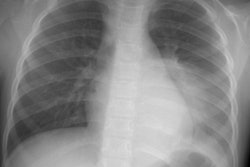
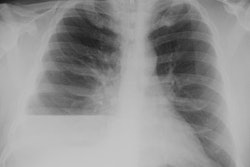
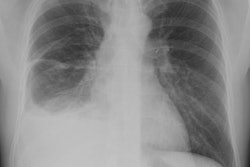
X-ray:
CXR: The lesion is generally a pedunculated (40%), rounded, solitary mass with a sharp, but incomplete border (characteristic of a pleural based mass). Pedunculated lesions may change in shape or position and may be located in a fissure. Obtuse angles with the pleural surface can be seen, but large or pedunculated lesions may form acute angles. The tumors predominate in the middle and lower half of the chest. The lesion can be very large- occupying the lower portion of the hemithorax and mimick diaphragmatic eventration or elevation [6]. Pleural effusion is found in 6-17% of cases [6] and is more likely associated with malignant tumors. Calcification in only 5-7% (mainly in large lesions).Computed tomography: On non-contrast exams the mass is of soft tissue attenuation, well marginated, and usually lobulated. The tumor displaces rather than invades structures. Contrast enhancement is usually intense and homogeneous due to rich vascularization. Non-enhancing areas may be seen and correspond to regions of necrosis, myxoid degeneration, or hemorrhage- particularly in larger lesions. In a review by the AFIP, 68% of lesions were heterogeneous on non-contrast CT and 88% on contrast enhanced imaging [6]. As with plain films, the angle between the mass and the chest wall may not be reliable in predicting the pleural origin of the mass. The lesion typically displaces, rather than invades adjacent structures- although sclerosis or pressure erosion may be seen on adjacent ribs in up to 8% of cases [6]. Calcification and pleural effusion are uncommon [7].
Magnetic resonance imaging: On MRI the lesions signal
characteristics
reflect its hypocellularity and abundant collagen stroma. The
lesion typically
has low signal intensity on T1 weighted images. Heterogenous, but
predominantly
low signal is also seen on proton weighted images and T2 weighted
images.
Areas of high signal intensity correspond to regions of necrosis
or myxoid
degeneration within the lesion. Intense lesion enhancement can be
seen
following the administration of gadolinium.
Cellular SFTs show high signal relative to muscle on T2 images
[9]. Following contrast administration, fibrous SFTs tend to show
little enhancement in the early phase and progressive enhancement
on delayed phase imaging [9]. Whereas cellular lesions show rapid
initial enhancement [9].
REFERENCES:
(1) J Comput Assist Tomogr 1997; Jan 21(1):115-120
(2) AJR 1997; Localized benign fibrous tumors of the pleura. 169: 683-686 (No abstract available)
(3) J Thorac Imag 1998; Desser TS, et al. Pictoral essay: Solitary fibrous tumor of the pleura. 13: 27-35
(4) Ann Thorac Surg 1999; de Perrot M, et al. Clinical behavior of solitary fibrous tumors of the pleura. 67: 1456-59
(5) AJR 2000; Truong M, et al. Localized fibrous tumor of the pleura. 174: 42
(6) Radiographics 2003; Rosado-de-Christenson ML, et al. Localized fibrous tumors of the pleura. 23: 759-783
(7) AJR 2011; Ginat DT, et al. Imaging features of solitary
fibrous tumors. 196: 487-495
(8) AJR 2017; O'Neill AC, et al. Metastatic patterns of solitary
fibrous tumors: a single-institution experience. 208: 2-9
(9) AJR 2017; Nagata S, et al. The value of MRI and clinical
features in differentiating between cellular and fibrous solitary
tumors. 208: 10-17