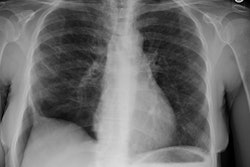
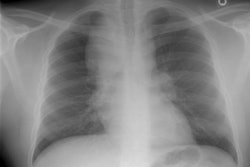
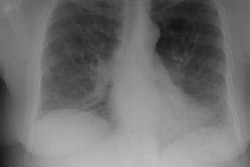
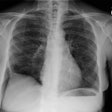
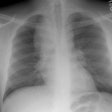
Pulmonary alveolar proteinosis: clinical features and outcomes.
Goldstein LS, Kavuru MS, Curtis-McCarthy P, Christie HA, Farver C, Stoller JK
INTRODUCTION: Pulmonary alveolar proteinosis (PAP) is a rare disease of unknown etiology and variable natural history. To date, the largest series from a single institution has consisted of 68 individuals. To extend the understanding of the clinical features and natural history of PAP, we present a series of 24 patients with PAP from a single institution. METHODS: Patients with PAP were identified by a review of The Cleveland Clinic Foundation discharge database from 1965 to 1995. After identification, a chart review of the 24 selected patients was conducted. Charts were abstracted for historical, diagnostic, and therapeutic features. Diagnosis was confirmed by a review of the lung biopsy, where it was available, by a lung pathologist. Follow-up by telephone was performed with 19 patients. RESULTS: Most patients (70%) were male, and smoking was common (75%; mean pack-years, 29) in the group. The mean age at initial evaluation was 43 years. Presenting symptoms were as follows: 19 patients (79%) reported dyspnea, 19 patients (79%) reported a cough, 4 patients (17%) reported hemoptysis, and 3 patients (13%) reported chest pain. The earliest available spirometry after presentation of symptoms showed a prediction of mean FEV1 of 74% (range, 45 to 99%) and a prediction of mean FVC of 76% (range, 41 to 99%). The diagnosis of PAP was established by transbronchial biopsy alone in 7 patients (29%) and by open-lung biopsy alone in 17 patients (71%). Whole lung lavage was deemed necessary in 13 patients (54%); 3 patients underwent lavage of one lung only, and 10 patients underwent bilateral whole lung lavage. Whole lung lavage was required only once in 46% of patients, and from two to four times in the remainder of patients. During the follow-up period (mean length of follow-up, 8.5 years; range, 5 months to 21 years), 25% of the patients died, but none as a result of sequelae of PAP. Half of the survivors reported persistent symptoms. CONCLUSIONS: In this series, which represents one of the largest single institutional experiences with PAP reported, the clinical features are largely consistent with previously reported cases. However, contrary to early reported experiences in which open-lung biopsy was frequently required to establish PAP and in which whole lung lavage was needed, transbronchial biopsy established the diagnosis in 29% of patients and whole lung lavage could be deferred in 46% of patients.