Hormonal changes caused by a woman's menstrual cycle may put them at higher risk of developing cancer from exposure to medical radiation, according to a letter published July 10 in Radiology. Providers may want to consider menstrual phase when deciding when to perform studies -- particularly nuclear medicine exams -- in younger women, the researchers recommended.
It's common knowledge that younger women have a higher lifetime attributable risk of cancer from exposure to radiation, with a 1.5-times greater risk of developing solid tumors and a sixfold greater risk of developing thyroid cancer than men. But the mechanism behind this difference is not entirely understood, wrote lead author Anat Biegon, PhD, and colleagues from Stony Brook University.
Major strides have been made in reducing radiation exposure with modalities such as CT, along with the use of PET/MRI instead of PET/CT. However, such progress has been more difficult in nuclear medicine, where it's hard to reduce radiation dose from radiopharmaceuticals without affecting image quality.
"Therefore, there is a need for new guidelines for radiotracer development and use, which ... are evidence-based, sensitive, and responsive to the greater risk to reproductive organs inherent in exposing reproductively competent women to administered radiopharmaceuticals," Biegon and colleagues wrote.
In the letter, they focused on the relationship between radiation risk and the hormonal changes associated with a women's menstrual cycle, citing it as an "underappreciated but avoidable source of vulnerability and risk to female reproductive organs, specifically ovaries, endometrium, and breasts."
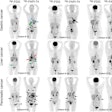
In an April 2015 study published in the Journal of Nuclear Medicine, Biegon et al performed a dosimetry study on men, postmenopausal women, and premenopausal women to measure the effect of exposure to the PET radioisotope carbon-11 vorozole on organs. The premenopausal women were imaged at two distinct phases of the menstrual cycle: midcycle and the menstrual-early follicular phase.
The researchers found that ovarian mean standardized uptake values were three times higher in young women at the midpoint of the menstrual cycle (ovulation), compared with values in the menstrual-early follicular phase or in postmenopausal women. They believe the increased uptake was related to ovulation.
Based on doses of 4 mCi to 8 mCi (148-296 MBq) per radiotracer injection, the researchers estimated that a conservative dose of 10 mCi (370 MBq) would exceed U.S. Food and Drug Administration (FDA) research study exposure limits for the ovaries (30 mSv for a single injection).
Therefore, more research must be conducted to find an optimum safety level for this patient population.
"At present, guidelines for performance of dosimetry studies do not specifically mandate inclusion of women at defined hormonal states, and consequently the information necessary for evidence-based assessment of exposure and risk in reproductively competent women is not available and unlikely to be without a policy change," the authors wrote.
To remedy the situation, Biegon and colleagues are calling for new guidelines for radiotracer development and use that include the potential risk to the reproductive organs of young women.