As radiology braces for a surge in imaging procedures in the aftermath of the COVID-19 pandemic, facilities must take steps to regain the public's trust that they can undergo imaging exams safely, according to Dr. Mahmud Mossa-Basha, chief of radiology at the University of Washington.
Radiology has already scaled back elective imaging in the time of COVID-19, taken measures to protect patients and healthcare workers, and absorbed a financial hit with a decrease in imaging volume. Moving forward, the discipline will have to reestablish trust with patients who need to feel assured they can undergo imaging without being at risk for infection.
Mossa-Basha spoke on May 1 at AuntMinnie.com's 2020 Virtual Conference about his facility's experience as one of the first in the U.S. to deal with COVID-19 patients.
On the other side
The University of Washington (UW) is now "on the other side" of the COVID-19 outbreak, having hit its peak in the number of cases on April 2. The surge in potentially infected patients had prompted a range of workflow changes at the department, which is now expecting another boom as non-COVID-19 cases that were postponed are rescheduled.
 Dr. Mahmud Mossa-Basha.
Dr. Mahmud Mossa-Basha.Inpatient imaging has been performed through glass or with glass partitions to separate radiologic technologists from patients, an arrangement that has conserved the use of personal protective equipment (PPE) at the hospital. Additionally, triage tents have been set up where outpatients can be seen.
In terms of testing for COVID-19, reverse transcription polymerase chain reaction (RT-PCR) testing has been the primary screening method, but its shortcoming is that false negatives do occur, Mossa-Basha said.
Imaging is not relied upon routinely for screening, as per guidelines from the U.S. Centers for Disease Control and Prevention (CDC) and the American College of Radiology. That said, imaging could be employed if there is limited access to RT-PCR testing and if there is an elevated progression due to health factors and/or exacerbation of clinical symptoms, Mossa-Basha said, noting that in Wuhan, China, when there was limited access to RT-PCR testing, providers turned to imaging.
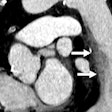
X-ray imaging has proven insensitive in detecting early or mild COVID-19 infection, but it has value in the detection of later presentation. CT offers high sensitivity but limited specificity. In addition, CT is more resource-intensive than RT-PCR testing or chest x-ray, he noted.
Solutions like portable CT scanners are a way of bringing imaging to the patient rather than the patient to imaging, avoiding transporting patients through hallways, and decreasing the need for imaging technologists to don PPE, he pointed out.
The creation on a national level of repositories of imaging data from COVID-19 cases may lead to the development of artificial intelligence algorithms to assist with diagnosis and prediction of patient outcomes, Mossa-Basha added.
When asked about using imaging to measure outcomes with remdesivir, which received U.S. Food and Drug Administration authorization on May 1 as a COVID-19 treatment, Mossa-Basha put forth that imaging could be helpful by evaluating progression of disease, and by extension, assessing medication efficacy.
"Imaging could serve as a marker for disease change over time," he said.
Ramping up postpandemic
For its part, UW plans a gradual ramp-up of elective imaging that will see appointments staggered to decrease waiting room exposures, as well as the reorganization of waiting rooms to maximize social distancing.
While some states are taking a similar approach to the University of Washington, others are diving in and returning to full capacity as stay-at-home orders expire, Mossa-Basha noted.
Regardless of how quickly or slowly institutions plan to ramp up, they need to regain the trust of the public, he believes. That means implementing a number of steps:
- Ensuring ample signage is targeted at patients to indicate precautions that need to be taken while in the hospital
- Universal masking
- Ample availability of hand sanitizer
- Hallway traffic that is one-way
- Online registration to schedule the time of an imaging test
- Text communication with patients to indicate when imaging is ready for them
- Waiting rooms with tape on the floor to denote safe distances from others
- Space out imaging exam times to permit adequate time to sterilize imaging suites
"We need to regain the patient's trust that we will do everything we can do to protect their health," Mossa-Basha said.
Without continuing precautions postpandemic, there will be a risk of "undoing of efforts" to limit infection, he warned. It will also be key to engage with the ordering physician and the patient to prioritize imaging orders according to time sensitivity.
The COVID-19 pandemic meant a significant drop in radiology volume, 52% at UW, pointed out Mossa-Basha. That drop has been accompanied by a decline in financial revenues. And to respond to that dramatic adjustment, UW has alternative revenue-generating activities in the works, such as increased contract research organization work, stand-alone outpatient imaging centers with shared revenue models, and population health and wellness services.
One positive change to come out of the pandemic has been an acceleration to working from home for UW radiologists. UW had begun to implement teleradiology prepandemic, and the pandemic created momentum toward working from home, Mossa-Basha said.
"We are now in stage II of the process," he said, noting that UW radiologists have been provided high-resolution screens to read high-resolution imaging when working from home.
To access 2020 Virtual Conference, click here. Presentations will be available for on-demand viewing for 30 days after the meeting concludes on May 1.