Examining 3D virtual reality (VR) models during presurgical planning for robotic-assisted partial nephrectomy led to reductions in operating time, blood loss, and hospital length of stay compared with planning based on MRI and CT scans alone in a new study, published online September 18 in JAMA Network Open.
The researchers from the University of California, Los Angeles obtained patient-specific 3D VR models to facilitate preoperative planning for partial nephrectomy. They found that cases for which the surgical team had access to the 3D VR models in addition to conventional 2D medical imaging data consistently demonstrated improved surgical outcomes.
"Surgeons have long since theorized that using 3D models would result in a better understanding of the patient anatomy, which would improve patient outcomes," lead author Dr. Joseph Shirk said in a statement. "But actually seeing evidence of this magnitude, generated by very experienced surgeons from leading medical centers, is an entirely different matter. This tells us that using 3D digital models for cancer surgeries is no longer something we should be considering for the future -- it's something we should be doing now."
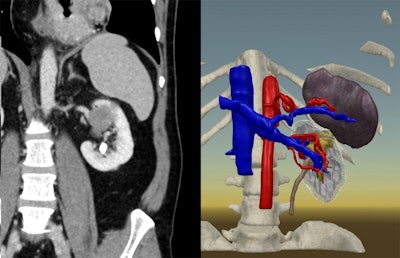 A 3D virtual reality kidney model (right) based on a patient's CT scan (left). All images courtesy of Dr. Joseph Shirk.
A 3D virtual reality kidney model (right) based on a patient's CT scan (left). All images courtesy of Dr. Joseph Shirk.Virtual reality improves kidney surgery
Recently, several groups have shown that studying virtual 3D models with VR and augmented reality (AR) devices can enhance clinicians' understanding of patient anatomy and help them determine the best surgical approach for glioma resection and kidney cancer surgery, among other procedures. Yet, few studies have validated the capacity of these advanced visualization technologies to improve surgical outcomes.
Highly complex operations such as partial nephrectomy likely stand to benefit the most from the integration of 3D VR models into presurgical planning because their success relies heavily on the surgeon's ability to identify small blood vessels and understand the spatial relationship between anatomical structures, the authors noted.
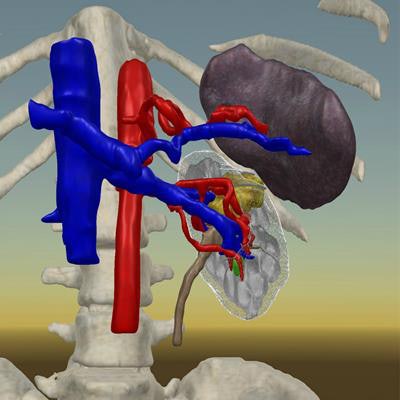
To determine the potential advantages of planning with 3D models, Shirk and colleagues obtained the MRI or CT scans of 92 kidney cancer patients scheduled to undergo robotic-assisted partial nephrectomy. They used the scans to generate individually tailored 3D kidney models for roughly half of the patient cohort. Each of the 3D models comprised at least the kidney tumors and renal vasculature, and most included several other structures such as the ureter, collecting duct system, and splenic vasculature.
The surgical team completed presurgical planning for each case either using the conventional method of inspecting just the patient MRI and CT scans or examining the MRI and CT scans in addition to viewing the 3D models on a smartphone and VR headset. The smartphone and VR devices allowed the clinicians to rotate and expand the 3D models as well as reveal or hide specific anatomical structures to better visualize the ideal surgical route.
 Dr. Joseph Shirk viewing a patient-specific 3D virtual reality kidney model on a smartphone.
Dr. Joseph Shirk viewing a patient-specific 3D virtual reality kidney model on a smartphone.Better outcomes?
Overall, the researchers found the VR group had reductions in several key metrics of surgery outcome, including the duration of surgery, estimated blood loss, and length of hospital stay. The initial raw data did not achieve statistical significance.
After controlling for several covariates, however, the researchers discovered that patients in the VR group were nearly three times more likely to have a short hospital stay (two days or less) and about two times more likely to lose less blood during surgery (200 mL or less) than those in the control group; the odds ratio was 2.86 for shorter hospital stay and 1.98 for less blood loss in the VR group. Those differences were indeed statistically significant (p < 0.05).
| 3D VR models vs. 2D imaging in presurgical planning for partial nephrectomy | ||
| MRI or CT | 3D VR models + MRI or CT | |
| Duration of operation | 173.3 min | 172.6 min |
| Estimated blood loss | 145.7 mL | 124.5 mL |
| % of patients who spent more than 2 days in the hospital | 7% | 4% |
What's more, Shirk and colleagues noticed the magnitude of the improvement in outcomes increased in accordance with increasing case complexity. By clearly displaying the spatial relationships among anatomical structures -- including size, distance, and configuration -- the 3D VR models may have helped improve surgical decision-making and minimize surgical challenges, they noted.
"Visualizing the patient's anatomy in a multicolor 3D format, and particularly in virtual reality, gives the surgeon a much better understanding of key structures and their relationships to each other," Shirk said. "This study was for kidney cancer, but the benefits of using 3D models for surgical planning will translate to many other types of cancer operations, such as prostate, lung, liver, and pancreas."