Percutaneous cryoablation is comparable to surgery for treating kidney cancer, offering similar 10-year survival rates and lower rates of complications, according to a study published June 9 in Radiology.
The study results suggest that there's a less invasive way to treat kidney cancer, wrote a team led by Dr. Christos Georgiades, PhD, of Johns Hopkins University in Baltimore.
"We have been doing cryoablation with increasing frequency at Johns Hopkins," Georgiades said in a statement released by the RSNA. "It's an outpatient procedure that takes about 30 to 40 minutes to perform. We observe the patient for three hours, and then they can go home."
For the procedure, an interventional radiologist inserts a hollow needle into the tumor using imaging guidance, then administers argon gas to freeze it. Georgiades' team compared 10-year outcomes from 134 patients who underwent cryoablation for early-stage kidney cancer with those of patients who had a radical or partial nephrectomy.
The group found that disease-specific survival of the patients who had cryoablation was 94% at both five and 10 years after treatment -- comparable to results from radical or partial nephrectomy. They also found that cryoablation had a low 10-year risk of hemodialysis and a complication risk of 6%, compared with 15% to 20% for surgery.
"For certain patients, cryoablation is equivalent to surgery with fewer side effects," Georgiades said.










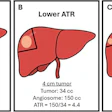



![Overview of the study design. (A) The fully automated deep learning framework was developed to estimate body composition (BC) (defined as subcutaneous adipose tissue [SAT] in liters; visceral adipose tissue [VAT] in liters; skeletal muscle [SM] in liters; SM fat fraction [SMFF] as a percentage; and intramuscular adipose tissue [IMAT] in deciliters) from MRI. The fully automated framework comprised one model (model 1) to quantify different BC measures (SAT, VAT, SM, SMFF, and IMAT) as three-dimensional (3D) measures from whole-body MRI scans. The second model (model 2) was trained to identify standardized anatomic landmarks along the craniocaudal body axis (z coordinate field), which allowed for subdividing the whole-body measures into different subregions typically examined on clinical routine MRI scans (chest, abdomen, and pelvis). (B) BC was quantified from whole-body MRI in over 66,000 individuals from two large population-based cohort studies, the UK Biobank (UKB) (36,317 individuals) and the German National Cohort (NAKO) (30,291 individuals). Bar graphs show age distribution by sex and cohort. BMI = body mass index. (C) After the performance assessment of the fully automated framework, the change in BC measures, distributions, and profiles across age decades were investigated. Age-, sex-, and height-adjusted body composition reference curves were calculated and made publicly available in a web-based z-score calculator (https://circ-ml.github.io).](https://img.auntminnie.com/mindful/smg/workspaces/default/uploads/2026/05/body-comp.XgAjTfPj1W.jpg?auto=format%2Ccompress&fit=crop&h=112&q=70&w=112)


