Can musculoskeletal ultrasound obviate the need for MRI in adult patients with shoulder pain? Perhaps, as most of the time the combination of radiography and ultrasound is all that's needed, according to research published in the July issue of the Journal of the American College of Radiology.
In a retrospective review, a team led by Dr. Scott Sheehan of William S. Middleton Memorial Veterans Hospital and the University of Wisconsin found that nearly half of the shoulder MRI exams at their institution were inappropriately ordered. Although not yet offered at the Veterans Affairs (VA) hospital, ultrasound could have been the indicated modality for two-thirds of shoulder MRI orders.
What's more, the authors estimated that the combination of ultrasound and radiography would have been sufficient to characterize the relevant pathology 85% of the time. Musculoskeletal ultrasound would also have yielded significant cost savings, as well as improved patient wait times for all MRI exams, according to the group (JACR, July 2016, Vol. 13:7, pp. 780-787).
"We conservatively estimate that if musculoskeletal ultrasound had been available within our center in 2013, we could have saved $57,243, with an associated 6% reduction in scheduling delays for all MRI examinations," the authors wrote. "These annual savings should be magnified if musculoskeletal ultrasound were similarly instituted at additional VA healthcare facilities."
A cost-effective alternative?
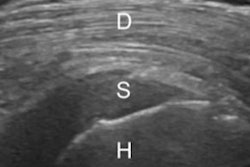
Radiography is often the preferred initial exam for shoulder pain, as stipulated in established guidelines such as the American College of Radiology (ACR) Appropriateness Criteria and the Society of Radiologists in Ultrasound (SRU) consensus conference statement. The guidelines also frequently recommend ultrasound instead of MRI as the next step for diagnosing soft-tissue shoulder injuries. Because ultrasound and MRI often demonstrate similar efficacy for diagnosing soft-tissue shoulder injuries in adults with shoulder pain, ultrasound could be a more effective first advanced imaging modality, according to the researchers.
As a result, they sought to assess whether shoulder MRI exams ordered within a capitated healthcare system adhered to imaging guidelines. In addition, they wanted to see whether ultrasound could be a complementary and cost-effective alternative to MRI.
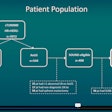
They retrospectively reviewed all 237 shoulder MRI exams performed at their VA tertiary care hospital in 2013 and found that 106 were inappropriately ordered, after applying a consolidated version of the ACR and SRU guidelines. Of these 106, 98 (92%) were inappropriately ordered due to the absence of a preceding radiograph.
Ultrasound would have been the indicated imaging modality in 157 (66%) of the cases, according to the guidelines. Based on the reported efficacy rates for radiography, ultrasound, and MRI in the literature for the various pathologies, the researchers estimated that ultrasound would have -- in combination with radiography -- been sufficient to characterize all relevant pathologies in 133 (85%) of 157 cases.
Delving deeper into the data, the researchers found that nonorthopedic providers ordered shoulder MRI exams inappropriately 44% of the time, compared with 17% of the time by orthopedic specialists. The difference was statistically significant (p = 0.016). They also found that ultrasound could have been sufficient in 80% of all cases ordered by nonorthopedic providers and in 50% of exams ordered by orthopedic specialists. That difference was also statistically significant (p = 0.07).
"Our data suggest that efforts to improve ordering practices targeting both primary care and other nonorthopedic providers would yield the highest returns toward ordering appropriateness, though orthopedic providers would also benefit from such interventions," the authors wrote.
Clinical decision-support (CDS) and computerized physician order-entry (CPOE) software directed at nonorthopedic providers could also help prompt them to order a radiograph as well as provide the most relevant clinical findings, according to the researchers. In the study, 51% of the MRI indications were for "nonspecific pain, weakness" and did not include any additional relevant clinical history. More information would lead to better decision making in ordering advanced imaging studies.
"Capturing more relevant patient history through CPOE could improve both imaging appropriateness and communication of critical clinical findings," they wrote.
Substantial cost savings
Using 2013 relative value units (RVUs) published by the U.S. Centers for Medicare and Medicaid Services, the researchers estimated $321.59 in savings for each case in which ultrasound would be substituted for MRI. In 2013, that would have added up to $57,243 in annual savings for their institution.
In addition, the researchers estimated there would have been a 6% improvement in patient wait times for other indicated MRI exams. Decreased utilization of MRI resources would also decrease waiting times for indicated MRI examinations, the authors noted.
They acknowledged a number of limitations in their study, including its reliance on retrospective review and image analysis. In addition, it's possible that important clinical context might have been missed during electronic medical record reviews.
"Regardless, future prospective studies might elucidate MRI ordering once [ultrasound] is available and highlight why there are differences in ordering appropriateness between provider specialties," the authors wrote. "Finally, because shoulder [ultrasound] is not yet widely offered at our center, an accurate assessment of cost savings or impact of increase in ultrasound imaging utilization is not currently feasible."