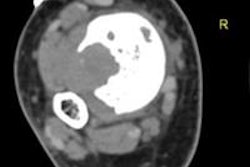
Ultrasound-guided biopsy of bone neoplasms yields similar accuracy to CT-guided biopsy for evaluating primary and metastatic bone lesions, while saving money, offering patient convenience, and avoiding radiation dose, according to research from the Henry Ford Health System.
In a retrospective study involving more than 100 patients, ultrasound-guided biopsy and CT-guided biopsy both had overall accuracy of 87.9%. Furthermore, there were no significant differences in performance based on type of lesion appearance on radiography, location, or size, according to Dr. Rounak Bafana. He presented the findings during a session at the 2014 RSNA meeting in Chicago.
The researchers set out to compare the diagnostic accuracy of ultrasound-guided biopsy with CT-guided biopsy for primary and metastatic bone lesions. They also wanted to determine if there were certain characteristics of lesions that make them more amenable to biopsy via ultrasound guidance, Bafana said.
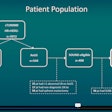
They initially performed a retrospective review of 206 patients with suspicious osseous lesions of the appendicular skeleton and shoulder girdle from February 2003 to May 2009. Ninety patients were excluded from the study because the biopsy target was located within the spine or the target was outside the spine and purely sclerotic.
Of the remaining 116 cases of lytic or mixed lytic/sclerotic lesions within the appendicular skeleton/shoulder girdle, 33 were biopsied by ultrasound and 83 were biopsied by CT. All patients received percutaneous core needle biopsy and/or fine needle aspiration (FNA) biopsy; eight patients had only FNA biopsy and 73 had only core biopsy.
Ultrasound- and CT-guided FNA biopsies were performed using 20- or 22-gauge needles, while core biopsies were typically conducted using spring-loaded core devices with a 14-18 gauge needle and two to four core samples.
The researchers calculated diagnostic accuracy by comparing the FNA and/or core samples with the results of the surgical pathology. In the cases that did not result in surgical intervention, accuracy was determined based on clinical outcome, according to Bafana.
The team considered a biopsy result to be a true positive or a true negative if the pathological results matched those of the surgical pathology or clinical outcome. Likewise, results were considered to be false negative if the biopsy results didn't match the surgical pathology or clinical course. The researchers did include biopsy samples that were inadequate or nondiagnostic in their accuracy analysis.
Biopsy accuracy was as follows:
- Overall CT-guided biopsy: 73/83 = 88%
- Overall ultrasound-guided biopsy: 29/33 = 87.9%
- CT-guided core biopsy: 64/79 = 81%
- Ultrasound-guided core biopsy: 24/29 = 82.8%
- CT-guided FNA biopsy: 19/25 = 76%
- Ultrasound-guided FNA biopsy: 10/18 = 55.6%
No statistically significant differences were found by modality with regard to general anatomic biopsy site, radiographic appearance, or lesion size.
| Biopsy accuracy by size | |||
| 0-3 cm | 4-6 cm | > 6 cm | |
| CT-guided biopsy | 21/25 = 84% | 39/42 = 92.9% | 13/16 = 81.3% |
| Ultrasound-guided biopsy | 8/9 = 88.9% | 12/14 = 85.7% | 9/10 = 90% |
The researchers acknowledged several limitations of their study, including its retrospective nature and selection bias; the decision to use ultrasound or CT guidance was operator-dependent, Bafana said.
In addition, apparent differences in accuracy between the modality-specific biopsies and lesion characteristics may not have been detected due to the small sample size of ultrasound-guided biopsies, he said. Bafana also noted that ultrasound is generally not selected for use with spine biopsies or purely sclerotic lesions due to acoustic shadowing. Those cases were excluded from the study.
Nonetheless, ultrasound-guided biopsies offer a number of benefits over CT-guided biopsies, including improved performance with smaller osseous lesions, superficial lesions, lesions with a soft-tissue component, and lesions adjacent to neurovascular structures requiring fine needle control, he concluded.
"It also avoids radiation," Bafana said.