Augmented reality (AR) systems may enhance image-guided tumor ablations by improving the accuracy of needle placements, according to a study published January 29 in the Journal of Medical Imaging and Radiation Sciences.
In a medical literature review, a group at McMaster University in Ontario, Canada, said they found compelling evidence that AR can offer interventional radiologists real-time guidance and enhanced visualization during these procedures, noted first author Yousif Al-Naser and colleagues.
“These findings collectively support the potential benefits of AR systems in enhancing image-guided tumor ablations,” the group wrote.
Interventional radiologists use minimally invasive image-guided procedures for diagnosing and treating various conditions, including alcohol and thermal tumor ablation techniques. Yet these procedures present challenges such as increased procedure time, radiation dose, and risk of tissue injury, the authors noted.
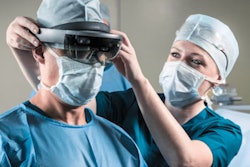
AR technology presents virtual objects to the real environment by overlaying digital content onto a user's real-world view. The technology can display target lesions and adjacent tissues directly onto procedural zones and thus eliminate the need for clinicians to alternate between patient and image displays, for instance.
Recent accomplishments with performing the first AR-assisted shoulder replacement demonstrate progress and indicate that the translation of AR technology into the interventional radiology suite may be approaching, the group added.
In this review, out of an initial search that yielded 1,676 articles, the authors focused on five studies published from 2009 to 2022 that specifically assessed AR's efficacy in tumor ablations. Three studies were conducted in Italy, one in the U.S., and one in France.
Two studies compared an optical-based AR system with CT guidance. Two studies used a head-mounted AR device, while one used a dual-camera setup. Various tumor types were examined, including bone, abdominal soft tissue, breast, hepatic, renal, colorectal, and lung lesions, the researchers wrote.
“All studies showed positive results, including reduced radiation exposure, shorter procedures, and improved navigation, and targeting assistance,” the authors noted.
For instance, in one of the studies in Italy, researchers used a SIRIO AR system and compared it with conventional CT guidance in patients who underwent bone or lung ablation procedures. The researchers gauged the accuracy of needle placement, procedure duration, and radiation exposure levels and found that the implementation of the AR system exhibited superior accuracy in needle placement.
“This was attributed to the real-time guidance and enhanced visualization offered by the AR system, enabling precise and optimal needle positioning,” the group wrote.
Ultimately, the review is also useful in part for the study limitations it identified in the field so far, which included small sample sizes, non-randomized lesion selection, and technical challenges, which underscore the necessity for further research and development, the authors wrote.
Future investigations should address these limitations and encompass larger and more diverse patient cohorts to ensure comprehensive findings, they suggested.
“Nevertheless, these findings collectively support the potential benefits of AR systems in enhancing image-guided tumor ablations,” the group concluded.
The full article is available here.