Have you ever pulled up an image and had a feeling that something wasn't right? You might not be imagining things, according to an August 29 study in the Proceedings of the National Academy of Sciences. The study indicates that radiologists may have a sense that cancer is present in an image even if there are no obvious signs of abnormality.
Researchers from the U.S. and U.K. tested the ability of radiologists to detect abnormalities in a set of mammograms, but they only gave them a half second to review each image rather than the normal amount of interpretation time. The radiologists were able to differentiate between normal and abnormal mammograms, but they didn't do so well at localizing abnormalities.
The results suggest that radiologists are sensing what the authors say is a global sense of abnormality -- what the authors call a "gist signal" -- that goes beyond specific anatomical signs or structures that would indicate pathology (PNAS, August 29, 2016).
Getting the gist of it
Radiologists have talked about how sometimes images just don't feel right when they are first pulled up on a workstation, according to Jeremy Wolfe, PhD, a professor of ophthalmology and radiology at Harvard Medical School and Brigham and Women's Hospital in Boston. Wolfe is the senior author on the PNAS paper, along with lead author Karla Evans, PhD, of the University of York in the U.K.
"Whenever we talk to experts, they say, 'When that image first comes up on the screen, I know it's bad; I just have a feeling,' " Wolfe told AuntMinnie.com. "We wanted to know if that feeling was real."
 Jeremy Wolfe, PhD, from Harvard Medical School and Brigham and Women's Hospital.
Jeremy Wolfe, PhD, from Harvard Medical School and Brigham and Women's Hospital.Indeed, research into visual perception has found that humans are able to rapidly extract details of a scene -- a gist -- when presented with new visual information. This ability is key for humans to allocate time and attention intelligently, such as determining whether a scene contains food or danger, the researchers noted.
This phenomenon also occurs for experts working with complex images within their domain of expertise, such as radiology. For example, previous research has found that radiologists can differentiate normal from abnormal mammograms in as little as a quarter-second, while nonexperts can't.
If it's indeed true that radiologists can sense the gist of cancer in an image, the question then becomes whether there is a subliminal phenomenon at work that could be harnessed, either to improve radiology training for interpreting images, or for fine-tuning computer-aided detection (CAD) algorithms. The researchers sought to find out.
They performed a series of experiments designed to test whether radiologists could detect abnormal mammograms using a gist signal at rates that were better than random chance. If the gist signal was real, the group then wanted to investigate which aspects of breast morphology -- such as changes in symmetry or tissue density -- might be playing the most important role.
They recruited 49 radiologists from centers in the U.S. and U.K. and had them review 120 full-field digital mammograms, half of which had cancerous lesions and half of which were normal. The researchers ensured that the abnormal mammograms had subtle pathology rather than obvious abnormal findings.
The mammograms were displayed for half a second to the radiologists to allow them to develop an overall perception of the image, instead of investigating it in detail. For some of the experiments, the radiologists were asked to rate on a scale of 0 to 100 whether they thought a mammogram was abnormal and the patient should be recalled. Meanwhile, other experiments had them indicate the most likely location of an abnormality by clicking on the computer screen.
The group found that radiologists were indeed able to differentiate the abnormal mammograms from the normal ones with a frequency better than just random chance, indicating the presence of a gist signal, Wolfe said.
The researchers then tried to figure out what factors might be leading to the phenomenon. Neither symmetry nor density was a major contributor to a correct interpretation. Also, the radiologists weren't able to pinpoint lesions on abnormal images at rates any higher than chance. This led Wolfe and colleagues to believe that the ability of radiologists to sense abnormality was based on a global signal spread across the breasts.
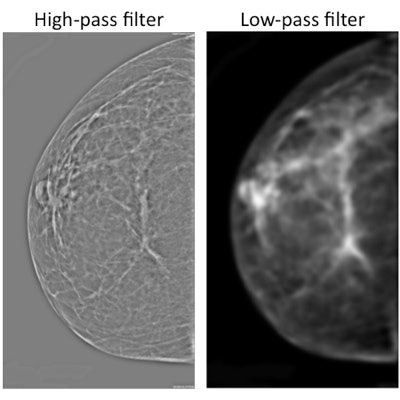
So the group tried applying image-processing filters to the images to see if these made a difference. In one experiment, they used a filter that allowed high frequencies to pass through (high pass), resulting in images in which grayscale levels were similar but fine details were more visible. They also employed a filter that allowed low frequencies to pass through (low pass), which produced fuzzy images with more grayscale variation.
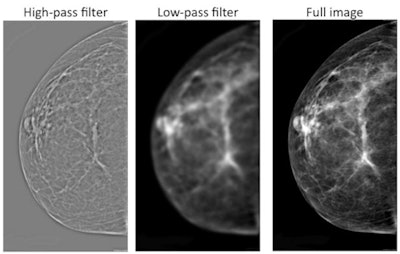 Images demonstrate mammograms with various levels of filtering, from high-pass image at left to unfiltered image at right. Courtesy of PNAS.
Images demonstrate mammograms with various levels of filtering, from high-pass image at left to unfiltered image at right. Courtesy of PNAS.Interestingly, they found that radiologists viewing either the high-pass images or the unfiltered images performed better than chance in detecting abnormal mammograms, while those viewing low-pass images did not. This led the group to speculate that something in the high-frequency images is contributing to the gist signal that radiologists are picking up on.
"It's not just some high-frequency detail of the tumor or the mass that is visible, it is something about the texture and parenchyma in both breasts that's letting radiologists beat this game of flash mammography in half a second," Wolfe said.
Future work
Wolfe and colleagues see a number of potential future avenues for following up on the findings. They plan to review the files of individuals who have been through multiple rounds of breast screening exams interpreted as normal, but who were later diagnosed with cancer. Could there be signs of future pathology on the earlier mammograms?
Another intriguing path could be using the information from the current study to fine-tune CAD algorithms. If high-pass information is really the key to the gist signal, could a CAD algorithm be programmed to focus on higher frequencies?
"I would like to know if you can use this signal to read the future," Wolfe said. "The practical piece is, if you can nail down what that signal is, that might be useful to someone who is trying to make a CAD that is increasingly more and more precise."



















