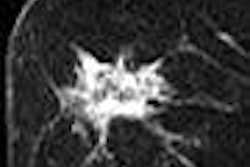
Like other major imaging modalities, mammography has gone digital. But full-field digital mammography (FFDM) most often utilizes a different setup for reading than other digital modalities. While these other modalities are read on PACS, many facilities have chosen to read FFDM studies on standalone dedicated workstations (DWs), manufactured by FDDM vendors. This setup was the initial paradigm required by the U.S. Food and Drug Administration (FDA) up until several years ago.
The advantage to the vendors is clear: DWs list for about $150,000 per unit. But integrating the FFDM unit with a PACS is a far superior option in my opinion. At the Sansum Clinic, a multispecialty outpatient clinic in Santa Barbara, CA, we were early adopters of FFDM and have had digital units in place for just over four years.
Moreover, we've been 100% filmless since going live with FFDM. We started out with two units from Fischer Imaging that replaced five analog ones. A third unit from Hologic of Bedford, MA, was added nearly two years ago. We now perform about 20,000 FFDM screening exams annually. Our archiving is 100% filmless with exams and immediate reports available over the Web -- all via the PACS -- since going live with digital mammography.
I began reading digital mammograms on our DW, but switched to PACS-based reading in early 2006. I made the switch for several reasons -- the shortcomings of the DW approach were apparent from the start (described in detail later on). In addition, my vision was to integrate FFDM with PACS, including primary interpretation, to create a single, fully integrated system, which was paperless and still equal to -- if not more efficient than -- a film-based viewer. Finally, our enterprise PACS network vendor (DR Systems, San Diego) offers full integration with FFDM (also discussed later on).
At Sansum, we're pleased with our FFDM and PACS integration, as well as its ease-of-use for archiving and Web distribution of images and results. If you are considering following in our footsteps, here is a top 10 list of things to keep in mind, based on my own experiences.
1. Deciding for or against DW
An FFDM vendor may try to convince you that its DW is the best way to maximize the value of FFDM, but don't give in too easily. Some of the reasons why PACS is a better bet than DW are obvious, while others become clear when you actually read mammograms on both systems.
Let's start with the most apparent reasons for the FFDM/PACS approach. Presumably, your facility already has a PACS, so reading mammograms on your existing technology leverages your investment and saves you the considerable expense of purchasing a standalone, single-purpose workstation, not to mention saving physical space.
Using DWs can also negatively affect productivity and workflow as radiologists must physically move from the FFDM workstation to another piece of equipment, especially if they are reading multimodality studies. The user interfaces on the DWs, historically have been very inefficient for reading digital mammography, resulting in a 50% to 100% drop in radiologist productivity, reported from our experience, and by others in the literature.
Speaking of workflow, the FFDM/PACS approach cuts down on any jostling to use the single resource of a DW, allowing a radiologist to read screening exams completely uninterrupted while another radiologist manages the workflow of an add-view interruption on a different PACS workstation. With mammograms read off one DW, there is competition for this single resource, between reading screening exams and managing add-view patients, interrupting the screening mammographer multiple times per day -- a frustrating and inefficient experience. A site could purchase more than one dedicated workstation, but that brings us back to the issues of cost and physical space.
In addition, DWs forces your radiologists to learn a new user interface just to read mammograms. This is true at go-live, as well as with annual software upgrades -- requiring the radiologist to master the nuances of multiple user interfaces.
In contrast, physicians trained to use the general PACS can read FFDM studies via the same interface they use to access studies done with other modalities. As a bonus, radiologists who read mammograms on PACS can compare multiple studies for the patient -- FFDM, MRI, ultrasound, PET -- on one workstation.
Another bonus of PACS: Web access. Referring physicians can directly access mammograms, and associated reports, from the PACS without having to constantly call your facility to request information. We have found that this kind of Web access resulted in a sixfold drop in calls from referring physicians for results.
Finally, if an interface is in place between the PACS and billing system, electronic billing is an option.
2. Expand the network to gigabit capacity
The FFDM systems available today offer a broad range of file sizes. Regardless of vendor, all digital mammography files are large enough to make a gigabit network preferable. Simply put, you need larger pipes to move these large files easily and quickly through the system. Even at gigabit speeds, a significant delay can occur when a digital mammography exam is opened along with comparison studies. Of course, interpreting the digital mammograms off a worklist allows for the preloading of the exam and any comparison studies, which provides instantaneous access to both.
In the (hopefully not-too-distant) future, a gigabit network may be less essential after the FDA approves lossy compression for digital mammograms. However, hospital and enterprise IT groups are moving in the direction of gigabit capacity already, mostly because of large multislice CT file sizes, so the overall PACS performance will be optimized with a gigabit network. Upgrading to this level will create advantages no matter what happens with digital mammography and data compression down the line. In our practice, we utilize gigabit infrastructure at both enterprises that we cover on the PACS.
3. Scale your archive capability appropriately
Ask yourself the following questions when calculating your archive needs:
- What is your average file size per modality?
- How many exams do you do per year?
- How many years must you keep an exam archived?
- Are you employing the lossless versus lossy data compression allowed by the FDA for all modalities besides digital mammography?
4. File size and the FFDM vendor
Take file size into consideration when choosing an FFDM system. If the images on two different digital mammography systems are diagnostically equivalent, I strongly urge you to purchase the system with the smaller file size. This will result in smaller archive volume requirements and less network traffic overhead. Most importantly for the radiologist and breast surgeons, the smaller images are much easier to navigate through at full resolution when looking for microcalcifications.
5. Make a comprehensive conversion to digital mammography
If your facility's financial resources permit it, it's far more efficient, from a workflow standpoint, to make a total conversion to digital rather than to convert partially or in phases. If you convert all studies at one time based on a certain deadline, the calendar division between digital studies and film-based studies will be clear. That means study searches can be accomplished in one database rather than two different databases that would result from a partial conversion. Also, a total conversion will make all exams and reports immediately available on the Web-based PACS, for the referring physicians.
6. Read-ready format
For greater efficiency and fewer interruptions, make sure your vendor sets up the equipment so that digital mammograms are in a read-ready format. The equipment should be preset so that the radiologist only has to window or adjust contrast on a study in rare instances (I sporadically adjust window and level settings on less than 5% of exams).
7. Digitize prior exams
For the sake of efficiency, having both current and prior exams available on the PACS is certainly preferable. If possible, digitize the desired film-based prior exams onto PACS for instant access and comparison, typically the day before the patient comes in for her screening exam. Otherwise, the radiologist will have to shuttle back and forth between digital images on PACS and film images on a neighboring viewbox. This brings up issues with siting, space, and ergonomics. Digitizing prior exams also gives direct access to your colleagues, such as breast surgeons and oncologists, who can view all the pertinent images via the Web-based PACS.
Digitizing prior exams will also save staff time as they'll no longer be required to pull prior film-based studies, physically bring them to the reading room, and post them on a viewbox.
Yes, there are both capital and labor costs involved with purchasing a digitizer, converting film-based studies to digital, and uploading to PACS. But those costs must be weighed against the frequent, ongoing labor costs associated with film.
8. But don't toss out the viewbox
Even if you do digitize film-based exams, you still need to keep a film viewbox onsite next to the PACS workstation. Occasionally, a patient may show up with prior film-based studies in hand, so a film viewer should be located conveniently next to the radiologist workstation.
9. Tool time
Select a PACS that has useful tools for reviewing mammograms. For example, we are able to apply a feature called image shuffling, which permits radiologists to quickly and easily compare images from multiple prior exams. Image shuffling also enables physicians to simply scroll between images to compare an area of concern on one image to the same area on another image. To do the same operation on another system requires multiple keystrokes, drag-and-drop functionality, or the use of specialized keypad keys.
I read mammograms using image shuffling to compare a current exam with prior studies, and I believe most radiologists will do the same within the next five years. The PACS should also provide a scenario-based approach for those who are used to reading off a DW and may initially demand this reading paradigm. Finally, with regard to paging, the PACS should give the reader flexibility when selecting a series of images to pair and view on the fly, all with a simple click of the mouse.
Another desirable tool is pixel tracking, which lets the reader know if he's viewed all pixels at full resolution. Finally, the PACS should have a "watchdog" capability so that if a radiologist mistakenly tries to mark unviewed images as "read," the system will ask him if this is really what he wants to do.
10. Full-feature PACS
If you are in the market for a PACS, select a full-featured model that can efficiently integrate with FFDM. Here are features that should be included:
- Integrated resource-based scheduling, including Web-based scheduling
- Electronic billing integration
- Structured template reporting
- Voice recognition
- Mammography report coding
- Automated report faxing
- Radiologist assessment/recommendation tracking
- Mammography-related management reports
Finally, we can present, manipulate, and review FFDM images on the PACS.
Ideally, you find a PACS that can do the same for you because the alternative is much messier and extremely inefficient -- either trying to integrate subsystems that weren't designed to work together, or forgoing integration and missing out on many important functions.
By Dr. Michael Trambert
AuntMinnie.com contributing writer
October 4, 2007
Disclosure notice: Dr. Michael Trambert is a medical advisor to DR Systems.
Dr. Michael Trambert is the lead radiologist for PACS re-engineering at the Sansum Clinic and Santa Barbara's Cottage Health System in Santa Barbara, CA. He is subspecialty trained in MRI, CT, and sonography, and has been in clinical practice in Santa Barbara since 1992. He is also involved in residency training at Cottage Hospital. Trambert has an undergraduate degree in computer science from Boston-based Tufts University and a graduate degree in computer science that he earned while in medical school at the University of California, Los Angeles.
The opinions expressed in this article are those of the author, and do not necessarily reflect the views of AuntMinnie.com.
Related Reading
Digital technology makes headway for breast cancer screening, August 29, 2007
Managing the transition to digital mammography, March 1, 2007
Digital mammography: Not just plug-and-play, October 23, 2006
A road map for integrating FFDM with generalized PACS, December 14, 2004
Referring physicians give thumbs up to PACS , June 11, 2002
Copyright © 2007 AuntMinnie.com