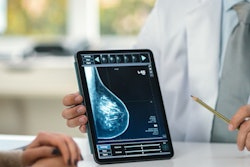
Some groups of women in recent years are less likely to undergo mammography, according to research published March 26 in JAMA Network Open.
While overall mammography use hasn’t significantly declined over the last 20 years, a team led by Adetunji Toriola, MD, PhD, from Washington University in St. Louis, reported significantly less mammography use among non-Hispanic white, Asian, and uninsured women ages 40 to 49 years from 2010 to 2022.
“These findings highlight the need for clear, risk-based screening communication and targeted strategies to promote guideline-concordant decision-making, particularly among younger women,” the Toriola team wrote.
Breast cancer screening guidelines in the U.S. have undergone several changes over the past two decades. The U.S. Preventive Services Task Force (USPSTF) in 2009 recommended biennial screening for women ages 50 to 74 years and informed decision-making for women ages 40 to 49 years. But in 2024, the USPSTF changed its guidelines to recommend biennial screening for women starting at age 40, a B-grade recommendation.
The American Cancer Society’s (ACS) 2015 guidelines meanwhile recommended beginning screening at 45 years, with the option to begin at 40 according to individual preference and informed decision-making.
Another factor to consider is the COVID-19 pandemic disrupting access to preventive services, including breast cancer screening. Experts have suggested this could have worsened existing barriers to care.
Toriola and colleagues studied trends in mammography use in U.S. women ages 40 to 49 and 50 to 74 years from 2002 to 2022, using data from the Behavioral Risk Factor Surveillance System (BRFSS) biennial cancer screening module. They included data based on sociodemographic, healthcare access, behavioral, and geographic factors, and analyzed potential associations with the 2009 USPSTF recommendations and the COVID-19 pandemic. Their final analysis included data from over 2.6 million women.
Mammography use overall trended downward during the study period. This included nonsignificant changes of -0.54% for women ages 40 to 49 years and -0.16% for women ages 50 to 74 years.
However, the team reported significant declines among the following women: young women without health insurance (-1.54%), current smokers (-1.36%), unmarried women (-1.10%), and non-Hispanic white women (-0.58%).
Following the 2009 USPSTF recommendation, mammography use decreased significantly among the following: younger non-Hispanic white (-0.88%), Asian (-2.45%), and uninsured (-2.39%) women. The researchers found no significant reduction among non-Hispanic Black women (-0.59%).
Finally, across both age groups, Western states showed consistently less mammography use than Eastern states.
The patterns observed in the study “suggest that changes in national guidelines can subtly yet meaningfully influence preventive care uptake,” the study authors highlighted.
“Observed declines among younger women may, therefore, represent guideline-concordant behavior, particularly among women who are more engaged with the healthcare system,” they wrote. “The observed racial difference in mammography use may reflect both differential responsiveness to guideline changes and the impact of community outreach or screening programs that support low-income and uninsured or underinsured non-Hispanic Black women.”
Read the full study here.