AuntMinnie.com presents the 17th in a series of columns on the practice of ultrasound from Dr. Jason Birnholz, one of the pioneers of the modality.
Fellow Ultrasounder,
This column is about the placenta, the most important factor neglected in routine ultrasound, and time, the weapon deployed by administrators to limit ultrasound's contribution to medical care.
When I started medical school I saw a quote attributed to Sir James Paget that I didn't understand at the time, but which has been lurking in my memory ever since. In presenting a surgical case to the chief of his service, a registrar whined about a lack of time; Mr. Paget replied, "You have all the time in the world."
This, of course, has been a complaint of house staff in all specialties forever, but I wondered what was so time consuming in the medical environment of the time, so free of paperwork and lab study. There is something essential about caring for and about patients in this pithy comment that is even more worthy of recollection now.
The migrating placenta
A new patient being seen for her second pregnancy told me that she was a "high-risk patient." I asked her to explain, and she replied that last time, in a faraway West Coast city, her doctor had diagnosed placenta previa at 16 weeks. She was placed on strict bed rest, except for weekly or bimonthly ultrasound exams. She was delighted that this form of therapy had worked, since there had never been any bleeding and the condition vanished in subsequent exams in the later third trimester.
 Dr. Jason Birnholz.
Dr. Jason Birnholz.The sad thing was that this conversation didn't happen 30 or more years ago; it was very recent. I'm assuming that the misdiagnosis was well-intentioned ignorance. The incidence of placenta previa is about 1 in 1,000 pregnancies, with at least 10% having a history of prior cesarean section.
Early ultrasound exams visualized the placenta transabdominally with a full bladder, and placenta previa was found in anywhere from 2% to 25% of patients in the early second trimester. Many of the exams done at the time were indicated by vaginal bleeding. Dr. Donald King tried to explain this discrepancy in 1973 with the notion that the placenta actively migrated within the uterus as the cavity expanded during the rest of gestation (Radiology, October 1973, Vol. 109:1, pp. 167-170).
We all recognize now that there is a band of thick muscle above the cervix early in pregnancy, removing the amnion from the internal os of the cervix. Placenta within this region can be misconstrued as being "low lying." No one wants to miss a true, complete placenta previa, so when in doubt, recheck without alarming the patient sometime in the middle of the third trimester (with endovaginal imaging and confirmation by visualizing vessels across the internal os with energy Doppler).
My point is not to explain the well-understood issue of placenta previa. Rather, I want you to think about the fact that some portion of every obstetric ultrasound exam is and has been devoted to placental localization, essentially since the beginning of widespread ultrasound itself, even though it is of (great) clinical significance in 1 in 1,000 pregnancies in the later part of the third trimester. There is usually nothing else about the placenta (or cord insertion) that gets any attention.
Chirp signals
Most of the previous articles in this series have hinted that higher-frequency, large-aperture, low-noise imaging conveys a lot more "information" than the low-megahertz "traditional" form of ultrasound that remains the community standard for transabdominal ultrasound. Updating ultrasound technique really pays off for the placenta.
The earliest forms of medical diagnostic ultrasound used transducers that were clamped in place and excited with an electrical jolt. Low-megahertz transducers were practical, but effective higher-frequency ones were difficult to manufacture in bulk because they were thinner and it was difficult to achieve shock excitation that would generate pulses with enough power to propagate, return, and be detected. We now have better transducer materials, and they are sliced or diced with incredible precision into 1D and 2D arrays. Our operational biases still reflect the early experience with regard to higher-frequency operation.
The idea of shock excitation is to get a pulse as short in duration as possible for maximal axial resolution; the shorter the pulse, the wider the bandwidth. We live in the real-world time domain, but there is an alternate version of reality in which explicit time vanishes as a dimension being replaced by frequency (of harmonic variables). The Fourier transform is an exact translation between these two domains. A fleetingly short pulse in time is one that has a massively wide range of frequencies. Think of a hologram as a frequency domain version of a picture. Both domains are real, but our direct perception is limited to just one.
One of the really cool innovations in ultrasound, previously developed for radar and then sonar, is to replace shock excitation with a long time pulse that ramps up continuously from low to high frequency. Returning pulses will be smeared in time, but they can be converted to the form they would have taken if the original pulse had been of short time duration.
This was simulated by analog means originally and is now done with digital filters utilizing Fourier or other more efficient transform rules. This is an amazing tool for achieving high-frequency, high-resolution imaging with conventional-array transducers. These kinds of pulses are called "chirp" signals, because this is exactly what bats do between 20 KHz and 60 KHz to find dinner on the wing.
A lot of current ultrasound development involves pulse coding and optimizing piezoelectric efficiency, the digital equivalent of tuning a piano for concert-level performance. Our practice techniques may not show it, but we have been living through technical sea changes like FM versus AM, high-definition digital video versus analog video, and various lossless compression schemes for transmitting high-quality audio and images.
Placental architecture
Some or most of the placenta is accessible transabdominally for 15- to 20-MHz scanning in the third trimester with modern ultrasound units, especially when the placenta is anterior or anterolateral, or fundal. Viewed in this way, a normal placenta is far from homogeneous. Neglecting fluid spaces, vascular voids, infarcts, or other anechoic or hypoechoic patches, the improvement in contrast enables seeing punctate reflectors, representing corked-off vessels, and later in the course of this pathology, patches of increased reflectivity that imply, as elsewhere, sclerosis (see figures 1 and 2). Small-vessel disease of the placenta is of the greatest clinical importance.
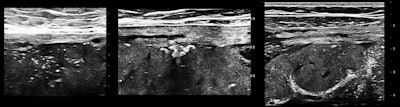
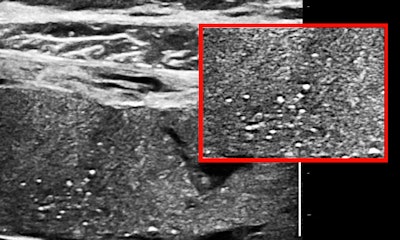 Punctate reflectors predominately on the fetal side of the placenta, the earliest indicator of emerging small-vessel disease.
Punctate reflectors predominately on the fetal side of the placenta, the earliest indicator of emerging small-vessel disease.The thrombophilia profile and an insight
Testing for hypercoaguability or the potential to form thromboses has been evolving for many years. The original concern in pregnancy was identifying the risk of deep-vein thrombosis, which can be prevented with support hose and a low dose of anticoagulant. The test has evolved into a panel of markers for a series of mutations predisposing to thrombosis.
Occult thrombophilia has emerged as a cause for implantation failure and miscarriage, which provides a link with risk factors in pregnant women with lupus, other collagen vascular diseases, and what might seem a familial predisposition for early pregnancy loss.
At about the time that thrombophilia was linked to miscarriage, more general concerns were already surfacing, including a paper published in the New England Journal of Medicine by Dr. Michael Kupferminc and colleagues on the increased frequency of genetic thrombophilia in women with pregnancy complications such as pre-eclampsia, fetal growth retardation, and fetal death in utero (NEJM, January 7, 1999, Vol. 340:1, pp. 9-13).
Several key works have addressed small-vessel disease of the placenta indirectly or directly, such as "Lower birth-weight in neonates of mothers carrying factor V G1691A and factor II A(20210) mutations" by Dr. Elvira Grandone and colleagues (Haematologica, February 2002, Vol. 87:2, pp. 177-181). Factor V is more commonly referred to as the Leiden factor.
So if you start seeing punctate reflectors in the placenta, you will think that a thrombophilia panel is a good idea, or, alternatively, if there is an abnormal maternal thrombophilia profile early in pregnancy, some sort of ultrasound surveillance for the emergence of small-vessel disease should be appropriate in the third trimester. The idea is to identify the risk and act to prevent placental sclerosis and its sequellae, growth retardation and/or hypoxic compromise of individual organs.
Hypoxic brain injury is a consequence of congenital cardiac malformations that can be potentiated by placental insufficiency. Grandone et al reported that birth weight was less than 2,500 g in about 14% of their two-factor thrombophilia panel-normal moms and about 28% of those with either of those two mutations.
Ultrasounders will know that the placenta is a fetal organ, not a maternal one, and that correlations will be improved when both maternal and paternal thrombophilia panels are reviewed together as an indication of fetal genotype.
Time warp
Let's add a pinch of time to this cauldron of concepts and placental soup and see what happens. The subtext of Sir James' rebuke has to do with the patient-physician relationship as it has been practiced continuously for hundreds of years. The inviolate kernel is that when a physician agrees to see a patient, he or she will do whatever the session requires regardless of the time it may involve.
We schedule some percentage of our interactions with the expectation that sometimes we will have to go well beyond the predicted allotment. I tend to think that the doctor's office that runs behind time is one where patient care comes first, although I doubt any patient having an indefinite delay would appreciate the paradox.
Nursing also has a similar, well-understood, tacit understanding of indefinite -- as necessary -- time commitment, especially in the context of around-the-clock shift coverage for inpatients. There does not seem to be anything similar or as binding ethically for technologists, who have come onto the scene of patient interactions very recently, a few tens of years in comparison with hundreds, and for whom relatively few exams are true emergencies.
In a typical practice, patients are scheduled for specified time slots, often fairly short ones, and the clinical intent of the exam is circumscribed. There is also usually a protocol identifying explicitly what series of views constitute an exam.
Blatant marketing
I started thinking about time after I saw a short article in the July-August 2014 issue of a major radiology trade magazine on the subject of the latest new technologies that speed ultrasound workflow. The article mentioned a survey of "providers" about workflow and purchase price of ultrasound systems; two manufacturers received scores of 90.6 and 89.9, which seemed to beat out the rest of what may have been a field of four manufacturers, each with multiple types of ultrasound equipment.
Then there was a statement indicating that one of the manufacturers had a "reduction of almost seven minutes per scan" and a quote from the author of the report, to wit: "Sonographers don't have the time to be tweaking buttons to get that perfect image. It's not just a different generation for ultrasound, but for sonographers as well."
That is about the time I lost it and filed the magazine where I thought it appropriate. Aside from the utter lack of anything that seemed to touch upon image quality, diagnostic content, or reliability, I just couldn't understand how anyone who actually knows anything about medicine or healthcare would ascribe any importance to some completely unsupported notion of shaving a few minutes off an exam. Certainly if a physician has ordered the exam, then having it streamlined is kind of insulting to the patient and demeaning to the operator as well. I tried unsuccessfully to get the report or any information about the data acquired for it or the basis of the scoring system.
The problem is that when exam time becomes an essential factor for ultrasound exams, contrary to one of the best established of medical practices, it becomes almost impossible to introduce new techniques like high-frequency imaging of the placenta or to engage in frivolous time-wasting things like "research." Picking the right probe and tweaking the system to (1) get the perfect image that (2) identifies or excludes a disease for (3) the patient is (4) at the heart of what we do.
Draw your own conclusions about marketing stuff intended for managers or administrators who are not providing direct patient care, even if it is labeled for those mythical "healthcare providers." I guess I will stick to peer-reviewed scientific papers and continue to hope for valid research on ultrasound practice issues, which are very difficult because our field is so balkanized by equipment, specialty, and levels of expertise and experience.
I have integrated high-frequency imaging into all the exams that I do with emphasis on the third-trimester placenta. I really don't mind seeing fewer patients per day to tolerate this whim in the knowledge that there are other resources in my community that can provide ultrasound exams with a similar monomaniac focus on the needs of the patient.
Dr. Jason Birnholz was one of the few advanced academic fellows of the James Picker Foundation, and he has been a professor of radiology and obstetrics. He is a fellow of the American College of Radiology and the Royal College of Radiology, and he was an associate fellow of the American College of Obstetricians and Gynecologists.
The comments and observations expressed herein do not necessarily reflect the opinions of AuntMinnie.com.