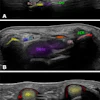
Young cancer patients treated with chemotherapy can be screened cost-effectively throughout their adult lives with echocardiography to help them live longer, according to a pair of just-released studies in the Annals of Internal Medicine.
In the first study, F. Lennie Wong, PhD, and colleagues used a model-based analysis to determine the cost-effectiveness of screening anthracycline-treated cancer survivors for asymptomatic left-ventricular dysfunction (ALVD). The second study, led by Jennifer Yeh, PhD, used a somewhat different model to look at the cost-effectiveness of echocardiography screening.
Both studies found that screening was cost-effective and could potentially save the lives of many cancer survivors. However, Wong and colleagues' analysis came in cheaper, with an incremental cost-effectiveness ratio (ICER) of $61,500 per quality-adjusted life year (QALY), while Yeh's group came in at $111,600 per QALY.
An accompanying editorial compared methodologies and found fault with Yeh et al's higher costs, which the editorialists attributed to a low estimation of echocardiography's sensitivity. But what's remarkable, they wrote, is how two studies using very different methods could arrive at such similar conclusions about the effectiveness of screening this at-risk population -- meaning that the researchers' conclusions are on track.
"Regular cardiac screening in cancer survivors will likely identify ALVD and lead to initiation of cardioprotective treatment earlier and at an [ejection fraction] greater than 35%," concluded Dr. Richard Steingart and colleagues from Memorial Sloan Kettering Cancer Center and Weill Cornell Medical College (Ann Intern Med, May 20, 2014, Vol. 160:10, pp. 731-732).
Treatment triggers risk
Childhood cancer survivors treated with anthracycline chemotherapy are at high risk for asymptomatic ALVD and eventually heart failure and death, Wong and colleagues wrote. The Children's Oncology Group (COG) long-term follow-up guidelines recommend lifetime echocardiographic screening for ALVD, but little is known about the effects of implementing these guidelines for a population at risk -- particularly with regard to costs (Ann Intern Med, pp. 672-683).
 F. Lennie Wong, PhD, from City of Hope.
F. Lennie Wong, PhD, from City of Hope.
"We didn't know if the screening recommended by the COG was really cost-effective or not," Wong, an associate research scientist in the City of Hope's department of population sciences in Duarte, CA, told AuntMinnie.com. "And we didn't know whether screening could be efficacious, and we don't have real live data, so we had to use a simulation. But using a lot of the data that are available, we were able to predict that, yes, doing screening on this population could reduce the risk of heart failure. Then the question is: If you're doing this echocardiogram quite frequently, is it going to be cost-effective?"
If anthracycline-related ALVD is detected, the guidelines recommend treatment with angiotensin-converting enzyme (ACE) inhibitors or beta-blockers to delay or prevent the onset of heart failure. The frequency of echo screening -- ranging from every one to five years -- depends on the status of 12 risk characteristics related to anthracycline dose, age at cancer onset, history of chest irradiation, and more.
Wong and colleagues measured lifetime risk for heart failure, as well as the lifetime costs of care and quality-adjusted life expectancy, expressing the results in incremental cost-effectiveness ratios.
When they compared the COG guidelines with no screening, they obtained an ICER of $61,500 for the cohort. Following the guidelines would increase life expectancy by six months and QALYs by 1.6 months, and the cumulative incidence of congestive heart failure would decrease by 18% at 30 years after the cancer diagnosis. However, reducing the frequency of screening would increase the cost-effectiveness and maintain 80% of the benefits, they noted.
"Screening every five years, recommended for 3% of survivors, could be maintained, but the frequency could be reduced to 10 years for an additional 12% of the survivors," Wong and colleagues wrote. "This study provides a rationale for decreasing the screening frequencies in the COG guidelines."
Yeh et al find higher costs
In their study, Jennifer Yeh, PhD, a research scientist at the Harvard School of Public Health, and colleagues modeled the cost-effectiveness of interval-based echocardiography every one, two, five, or 10 years. They also used ACE inhibitor and beta-blocker treatment for patients with positive ALVD results (Ann Intern Med, pp. 661-671).
With no routine screening, the group's case-based analysis showed a lifetime risk of 18.8% for systolic congestive heart failure in five-year childhood cancer survivors, with an average age of 58.8 years at onset. Serial echocardiography every 10 years cut this lifetime risk by 2.3%, whereas annual screening reduced the risk by 8.7%. Compared to no assessment, ICER was $111,600 per QALY for 10-year screening, and it exceeded $165,000 per QALY for exams more frequent than five years.
Treatment was quite expensive for patients who didn't receive anthracycline, with an ICER of at least $196,000. For the high-risk subgroup who received larger doses of anthracycline (≥ 250 mg/m2), assessment every two years was preferred. No assessment was preferred for those receiving low doses, according to the authors. Annual assessment wasn't cost-effective for either subgroup, with an ICER of more than $139,000 per QALY.
The likelihood of evaluation every five or 10 years being the preferred method at a $100,000-per-QALY threshold was 0.33 for the overall cohort, Yeh and colleagues wrote, ultimately recommending less frequent screening as the more cost-effective choice.
"Our findings suggest that current recommendations for cardiac assessment may reduce systolic [congestive heart failure] incidence, but less frequent screening than currently recommended may be preferred and possible revision of current recommendations is warranted," they concluded.
One big difference
"The sensitivity of echocardiography used for the models was a key difference between the studies," Steingart and colleagues wrote in their editorial.
Wong et al used a sensitivity of 75% to 94% based on noncancer population studies comparing ejection fraction by echocardiography with radionuclide scans, they wrote. Meanwhile, Yeh et al used a sensitivity of 25% based on a single study of adult survivors of childhood cancer that compared echocardiography with cardiac MRI. The editorial called this 25% sensitivity figure the critical difference between the studies -- one that likely affected the cost estimates.
Agreeing with that criticism, Wong told AuntMinnie.com that a sensitivity of 25% echocardiography is way too low and potentially drove up Yet et al's cost estimates. In any case, there are now better ways to perform echocardiography, Steingart et al noted, such as 2D speckle-tracking echocardiography or strain imaging.
Another methodological difference between the studies is that Wong et al evaluated the 12 risk profiles from the COG guidelines to determine screening frequency, whereas Yeh et al categorized persons as either low or high risk based on their cumulative anthracycline dose.
Steingart and colleagues also cautioned that few data are available on the natural progression from ALVD to heart failure in young cancer survivors, which forced both groups to extrapolate progression from data on patients who developed heart failure secondary to other medical conditions. Regardless, the time between ALVD and heart failure is strongly dependent on the cause and degree of ALVD, and neither group included detailed clinical information in its models, they added.
Childhood cancer patients "are cured of primary cancer because of the treatment with anthracycline, but that's not the end of the story," Wong told AuntMinnie.com. "There is a chance that especially the kids treated with high levels of anthracycline can develop heart disease later on, and that can compromise quality of life and longevity. Curing the first disease does not end the story; we have to follow them so that we can maintain quality of life."