
AuntMinnie.com presents the ninth in a series of columns on the practice of ultrasound from Dr. Jason Birnholz, one of the pioneers of this modality.
Fellow UltraSounder,
The "why" of doing ultrasound is easy to express. It is to help patients and their referring physicians, be it looking for disease, monitoring therapy, or excluding problems and establishing some level of wellness. The "how" part has always been the big problem for ultrasound.
 |
| Dr. Jason Birnholz. |
The big picture
No matter what applications you tend to focus on or what segment of the general patient population you may see, everything depends on image quality. The pictures you see when you are scanning are the core of ultrasound, and this is critical, whether you are acquiring an image as a technologist, interpreting the image as a physician, or combining both functions.
For most initial exams in most applications, the choice of adjunct modes used during the exam, like Doppler, elastography, or some form of image analysis, depends on what is seen in the B-mode images as the exam proceeds. Radiologists are, or should be, fanatical about image quality, because the archived images support the interpretation and provide the means by which the radiologist convinces the referring physician of that slice of diagnostic truth. One of the basic problems with ultrasound is that there really aren't standards for image quality that all of us follow in all of our work.
I have always thought of medical image acquisition as a form of photography, where we use sunlight or an artificial light source instead of a gust of x-ray photons, a storm of electromagnetism, or a stream of phonons (the theoretical indivisible building blocks of acoustic waves). I spend a lot of free time taking photos.* There are some basic things such as sharpness and exposure that are easy to judge, but in complex scenes, there are other factors in the eye of the beholder that become equally important.
Let's try to look at some ultrasound examples as if they were photographs. There will be some technical factors first, and then something more subjective as we contemplate what the image shows in the context of an individual patient.
Noise
Noise has always been the big enemy for ultrasound, just like photon scatter for radiography. There are a few principal forms of scatter in the x-ray world, where they occur at an atomic level. The ultrasound situation is more complex because the physical interactions are between acoustic wavelets at a certain wavelength and the macrostructure of tissues in the same size range. As a result, scatter varies with the depth of penetration at any frequency range and upon the properties of the tissue, such as surface roughness, anisotropy, and motion.
There is also random or semirandom electronic and computational noise associated with signal transmission and processing, unstructured noise known as "speckle" that appears like granular dust on the image. There are also forms of structured noise that arise from transducer construction, transducer materials, the way the transducer is excited, and the sampling rate, as well as electronic or computation noise that occurs throughout the signal transmission and processing. Manufacturers are pretty good about suppressing structured noise (except for multiple reverberations), but speckle reduction is a lot trickier.
One of the simplest ways to decrease noise is to average image frames. I feel a lot of pride about this because I came up with it for Varian, which created one of the first electronic scanning phased-array devices in 1975, and it was incorporated into the Acuson XP scanner in 1982. The signal-to-noise ratio is improved by the square root of the number of repetitions but at the cost of contrast reduction. The idea is that real things superimpose in an image, and random noise is distributed evenly across the field. Four frames may be best. In many devices this is the "persistence" control.
Let's take a little detour into the realm of information theory, which is not so strange since this topic has become central throughout all of the sciences after Claude Shannon's landmark paper on communications issues in 1948.
The basic problem was how to transmit a signal faithfully from one spot to another. Information has a probabilistic definition, and it is closely related to entropy. Using a wave to transfer the information implies some form of signal encoding, which is decoded or reconstituted when it is received. Noise in transmission degrades the information transfer. It is a basic precept that there is always a way to maximize information transfer through a specific channel.
In the ultrasound case, let's say we want a faithful representation of tissue anatomy to appear in an image. The display surface is an important part of the information-carrying channel. Its capacity (in bits) is the product of the number of gray shades, the width of the display matrix (in pixels), and the height of the matrix. This value is the total number of separate images that can be shown.
So, the first thing we would want is an ultrasound system that uses something equal to or better than high-definition digital television, and the second is that we want the target area to fill the display matrix. Put another way, big field-of-view images have less information than when the region of interest fills the image, which is why magnification is an essential system feature.
Next, we want to have a system where the capacity of the ultrasound wave portion of the channel does justice to the display. With some mathematical handwaving that has to do with energy, the main conclusion is that we want to operate in the highest frequency range that we can.
In the 1990s, there was a big advance -- chirp signal processing -- in moving up the usable frequency range for clinical ultrasound. For simplicity, we will act like ultrasound pulses have a single frequency, even though in the real world, we are always dealing with a range and distribution of frequencies. Early transducers were blasted with a powerful, very brief excitation, causing them to ring at their natural frequency. High-frequency transducers are thin and delicate and much less amenable to shock excitation.
Chirping, which is what bats do, involves sending out a signal that is long in time, with frequency increasing from low to high during the pulse. While lengthy pulses have very low spatial resolution, the proper type of decoding (or inverse filtering) enables the received signal to be squished digitally into one that is exactly equivalent to a massive shock excitation at the main frequency of the transducer.
Chirp signals (long in time with a range of frequencies) were originally ramp-like, with a linear increase in frequency over time. However, there are many ways to encode the signal, some of which have error-correcting features. Others excel in computational speed for decoding. This is the heart of "presets" in a lot of newer systems.
The forms of encoding are closely guarded secrets, and the U.S. Food and Drug Administration (FDA) ensures that whatever is selected conforms to safety criteria both for exposure and for transducer heating. The concern that I have always had with presets is that they tend to be labeled by an organ or an application. The problem that all of you will perceive is that what some engineer thinks might be best for a normal kidney or a normal thyroid is hardly likely to be optimal for searching for different kinds of pathology within those organs.
Two manufacturers unveiled new noise reduction techniques at RSNA 2012. Zonare Medical Systems preprocesses raw acoustic data before it enters the display chain, taking advantage of the expanded processing time from blasting a zone instead of building an image line by line. Siemens Healthcare now has a postscan image fix. Photographers routinely apply noise reduction filters to pictures, which is readily available for all kinds of digital imagery, but this is not done too often in ultrasound after the exam, as far as I know.
Images speak for themselves
My style of scanning is to zip around a lot of places while talking to patients about their symptoms and past history, zooming in to magnify something that catches my interest, filling the display matrix with the target region.
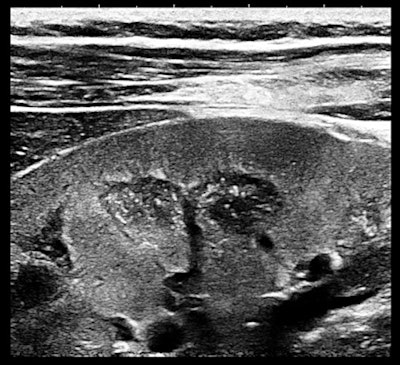 |
| Magnification view of a portion of the right kidney of a 32-year-old woman with ductal carcinoma in situ (DCIS) and a bicornuate uterus. All images courtesy of Dr. Jason Birnholz. |
The finding is a very early form of medullary sponge kidney. The vascular arcades at the corticomedullary borders (normal) and the punctuate nonshadowing reflectors within the pyramids are visible due to noise suppression.
The information content of this image is high. Frequency components are predominantly high, which can be seen here in the 2D fast Fourier transform (FFT) of this same image.
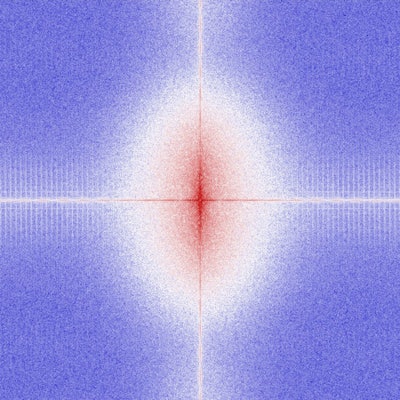 |
| Fast Fourier transform (FFT) of the same image as above. |
Contrast
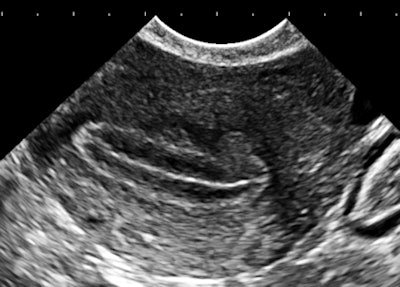
The importance of image contrast is demonstrated in these endovaginal images of a 36-year-old nulliparous woman with heavy and irregular periods due to adenomyosis.
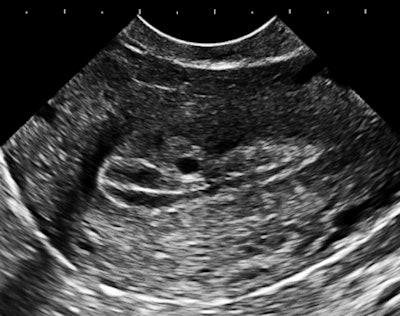 |
| Above and below: Endovaginal images of a 36-year-old nulliparous woman with heavy and irregular periods due to adenomyosis. |
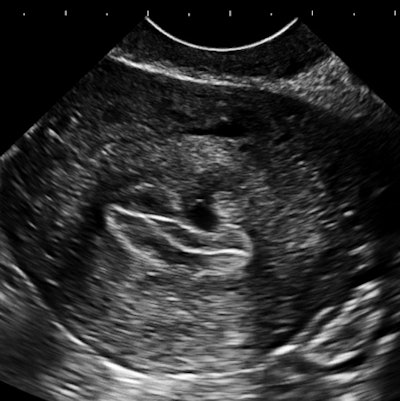 |
 |
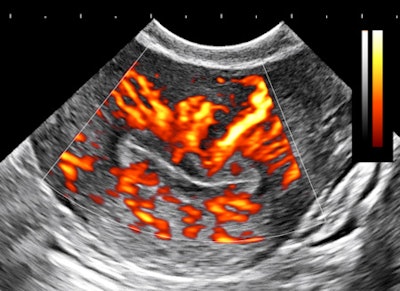 |
Adenomyosis (i.e., gland tissue in muscle) occurs when the integrity of the endometrial boundary is disrupted and rapidly growing, vigorous endometrial cells migrate from the city to the myometrial suburbs. Glandular tissue is highly vascularized, leading to the typical 2D Doppler findings with the clinical presentation of heavy, often painful menstruation with clots. There may be small secretory cysts.
The border zone irregularities reconcile the ultrasound findings with pathology and with the classic sign of hysterosalpingography for this condition. This is a grayscale contrast issue. Over the years, I have come to regard contrast as the most important determinant of image quality for all applications of ultrasound.
Contrast relates to the visibility of a structure against its background field. A glass stirring rod has zero contrast in a beaker of water; it is invisible. In ultrasound, there is the inherent contrast of target and background (i.e., very high for cysts versus "solid" tissue or very low for a well-differentiated hepatoma within a field of normal hepatic parenchyma). Contrast is always maximized when the display range goes from jet black to bright white, and it is influenced by pulse bandwidth (i.e., frequency spectrum, path length) and options such as grayscale assignment.
A lot of the early grayscale workers made a big mistake, which many people still continue to practice and, I presume, prefer. They tended to turn up the dynamic range setting to high values. This makes organ fields smooth, uniform, filled-in, and visually pleasing, if you don't know any better. The problem is that it increases noise and lowers contrast at the same time.
Most of the really powerful information that ultrasound can reveal resides in the subtle variations in reflectivity within parenchymal fields, like the adenomyosis example. Anything that ups noise or decreases contrast has to be avoided. A new esthetic that has to do with image content and diagnostic utility will quickly replace the low-info, smooth look of the 1980s. Another way of looking at too-high dynamic range is that it tends to convert a potentially revealing exam in a slender patient into the limited one that may be the best you can do when there is morbid obesity.
I tend to use harmonic imaging as my default because there is usually a slight improvement in contrast. When you are scanning and you find something that seems significant, the best course is to take a lot of images with a variety of settings and then use those that best show the lesion. This is a lot like a photographer bracketing exposures to get the best image with available light. Our job is not just to take a series of pictures; it is to make a diagnosis utilizing the best images possible.
Another big picture
The last case is a 19-year-old runner who had been experiencing localized right lower quadrant pain in her practice sessions. The diagnosis does not need ultrasound, but I am glad that the referring physician sent this patient (for rule-out chronic appendicitis, of all things).
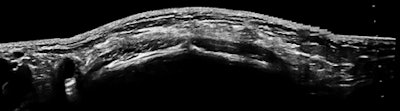 |
| Ultrasound image and photo of 19-year-old runner with localized lower right quadrant pain. |
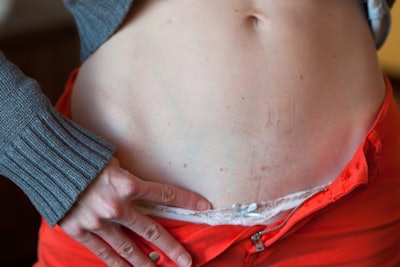 |
The only trick here is to begin the exam with the patient upright after walking. I won't say much about inguinal hernias, except that they occur in perhaps 2% of children, more often in boys (not her, obviously), more often with premature birth (didn't ask), and there is a familial pattern (which there was). I thought it might be fair to match a big field-of-view image with the magnified small field of the first case. When you are providing images to referring physicians, who are not imaging experts, let the image fit the pathology, or should that be punishment and crime?
These three cases were all from one afternoon in my little, suburban office. I tend to concentrate on early diagnosis and preventive medicine issues because that most suits my referral pattern. I don't mind admitting that this is a form of showing off, as is a lot of publishing and lecturing. But I hope that does not detract from my contention that there are a lot of things to be found if you look for them and if you aim for best possible image quality every time you view the screen or make an exposure.
*My photo website is VisualJason.com. It's a fun place, devoid of things medical. If you do visit, I hope you will at least find one picture in any of the topic galleries that brings you a little viewing pleasure.
Dr. Jason Birnholz is a graduate of Johns Hopkins School of Medicine and did his diagnostic radiology residency at Massachusetts General Hospital. He was awarded an advanced academic fellowship from the James Picker Foundation and has been a professor of radiology and obstetrics. He is a fellow of the American College of Radiology and the Royal College of Radiology
The comments and observations expressed herein do not necessarily reflect the opinions of AuntMinnie.com, nor should they be construed as an endorsement or admonishment of any particular vendor, analyst, industry consultant, or consulting group.



















