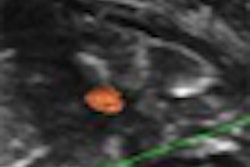
Performing successful carotid ultrasound studies requires awareness of pitfalls such as technical factors, patient limitations, and interpretation errors, according to Dr. John Pellerito of North Shore University Hospital in Manhasset, NY.
"The key to avoiding [carotid ultrasound] pitfalls is to review all three components [grayscale, color Doppler, and pulsed Doppler], integrate them together, and resolve your discrepancies," said Pellerito, director of the institution's peripheral vascular laboratory.
Carotid ultrasound studies involve the use of grayscale for plaque morphology, color flow for hemodynamics, and spectral analysis to grade degree of stenosis. Also, subtle changes in waveform shape can often lead to the correct diagnosis, Pellerito said. He spoke during a talk at the Leading Edge in Diagnostic Ultrasound conference, held earlier this year in Atlantic City, NJ.
"That's what separates the men and women from the boys and girls of vascular ultrasound," he said. "Anyone can make a diagnosis of stenosis, right or wrong, just by looking at velocity. But it goes much deeper than that."
A number of technical factors come into play during carotid ultrasound, including patient position and cooperation, misidentification of the internal and external carotid arteries, and improper settings of color flow, power Doppler, and pulsed Doppler parameters. Also, stenoses can be missed in unusual locations, such as the proximal common carotid artery or distal internal carotid artery, according to Pellerito.
"It's not enough just to look at the bifurcation," Pellerito said.
Improper settings of color-flow parameters (color gain, color velocity scale, and color-wall filter) can be a problem, he said. Possible pulsed Doppler pitfalls to be aware of include Doppler gain, pulse repetition frequency, sample volume size, spectral broadening, angle correction, and obtaining the highest velocity.
"If you have the Doppler gain too low, you're not going to be able to get correct amplitude," he said. "If I have it too high, I'll get a snowstorm appearance."
Spectral broadening could be produced by turbulence, a large sample volume, or an increase in the pulsed Doppler gain, he said.
Patient limitations
Carotid ultrasound users need to understand patient limitations, such as a high carotid bifurcation, deep vessels, vessel tortuosity, calcified plaque, and cardiac arrhythmia, Pellerito said.
Interpretation errors can also crop up in carotid ultrasound, stemming from errors in angle correction, the choice of Doppler criteria, and interpretation pitfalls. Users should attempt to employ a consistent Doppler angle, usually 60°, Pellerito said. "Never sample over 60°," he said.
The highest velocity is going to be in the stenosis or the jet, Pellerito said. Also, users should take advantage of pulsed Doppler and not rely on grayscale or color flow alone.
Occlusion versus stenosis
The difference between occlusion and severe stenosis is a crucial one. "If we say something is occluded, that patient has no therapeutic options," he said. "There's no endarterectomy in their future; there's no carotid stent. So you have to be sure."
This task requires excellent visualization of the internal carotid artery and very high color-flow sensitivity, which involves adjusting and optimizing color Doppler and using power Doppler, he said.
"And we always check everything with spectral Doppler," he said. "If we have a very high-resistance waveform, it's suggestive of obstruction distally and it's going to be low velocity, typically because there's nowhere to go."
It's also important to always scan transversely. "It's easy to miss things just in the sagittal plane," he said. "I always scan transversely, looking for things going on, collateral flow, where the veins are, [and so on]."
Sometimes a high-grade stenosis or occlusion may be accompanied by increased velocities on the contralateral side. Called compensatory flow, this is an important finding, he said. "It doesn't happen all of the time, but it happens enough that you should remember it."
Fine low-flow states can also be tricky.
Increased velocities are seen in stenosis, compensatory flow, a hyperdynamic state, and young patients. Decreased velocities stem from poor cardiac output, a distal stenosis or occlusion, and near-total occlusion ("string sign"), according to Pellerito.
High-flow states are characteristic of high cardiac output from thyroid disease or anemia, as well as contralateral disease. Low-flow states arise from poor cardiac output (congestive heart failure or cardiomyopathy), proximal or distal disease, or near-total occlusion.
"It's always important to integrate the clinical with the sonographic information and add all of the different pieces of the puzzle together to decrease your risk of misinterpretation," he said.
By Erik L. Ridley
AuntMinnie.com staff writer
September 9, 2009
Related Reading
How to provide great service in the ultrasound vascular lab, July 22, 2009
Future of ultrasound will require technology, educational gains, April 4, 2009
B-mode US shines in measuring carotid atherosclerosis, September 19, 2008
Vascular ultrasound QA requires consistency, validation, August 4, 2008
Ultrasound quality strongly affects ovarian cancer management, January 21, 2008
Copyright © 2009 AuntMinnie.com