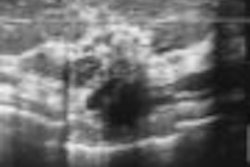
While a focused musculoskeletal sonographic exam can identify most abnormalities, a protocol-based exam allowed for identification of 98% of symptomatic abnormalities in a retrospective study, published in the January issue of the American Journal of Roentgenology.
"We advocate a protocol-based approach to musculoskeletal sonography supplemented with a focused evaluation at the site of patient symptoms to ensure a thorough and complete evaluation," wrote a research team from the University of Michigan Hospitals in Ann Arbor.
To evaluate the utility of a focused musculoskeletal sonography exam on the basis of patients' presenting complaints, the team retrospectively reviewed 602 patients evaluated over six months. The patients were all scanned with a routing protocol, employing a linear-array transducer (7-15 MHz) with either a MHDI 5000 (Philips Medical Systems, Andover, MA) or a Logiq 9 (GE Healthcare, Chalfont St. Giles, U.K.) scanner (AJR, January 2008, Vol. 190:1, pp. 5-9).
The systematic musculoskeletal sonography protocol consisted of a checklist of structures for each body part and joint. After the routine exam was completed, each patient was asked to indicate a focal point of discomfort and, if present, this area was rescanned.
The patients were then classified in one of five categories, depending on whether there was a focal point of discomfort and if an underlying sonographic abnormality was present or absent. All findings were confirmed by one of five supervising musculoskeletal radiologists with a mean of five years of experience.
Of the 602 patients, 83% had a sonographically detectable abnormality. Of these, only 2.2% had an abnormality undetectable by routine protocol-based scanning.
"The more peripheral the body part, the more likely that abnormalities detected by sonography correlated with focal symptoms," the authors noted.
They found 81% correlation in the wrist and hand, 73% correlation in the ankle and foot, 15% correlation in the shoulder, and 31% in the hip. Chi-square analysis showed a significant association between the body part scanned and a detectable abnormality (p < 0.0001).
"Because the proximal periarticular abnormality is often in the deeper tissues, exact localization by the patient and the pathophysiology of referred pain may make assessment more difficult and may partly explain these findings," the authors wrote.
The researchers acknowledged several limitations for the study, including a small sample size for several body parts, the retrospective nature of the study, and a lack of pathologic proof for all cases.
Nonetheless, the authors concluded that while focused sonography of the distal extremities at the site of symptoms correlated with an abnormality in most cases, a protocol-based approach identified 98% of symptomatic abnormalities.
By Erik L. Ridley
AuntMinnie.com staff writer
January 3, 2008
Related Reading
PACS offers direct access to MSK specialists without alienating rads, October 18, 2007
US-guided interventional procedures boost sports medicine performance, May 3, 2007
US shows full spectrum of shoulder injuries, September 29, 2006
Focused exams suitable for some musculoskeletal US studies, March 26, 2006
Copyright © 2008 AuntMinnie.com