CHICAGO - Stem cells injected transurethrally under ultrasound guidance have shown promise in treating urinary incontinence. Initial research results by Dr. Ferdinand Frauscher and colleagues from the Medical University of Innsbruck in Austria show stem cells developed from the patient's own muscle can reconstruct and strengthen the lower urinary tract.
Urinary incontinence is a problem affecting nearly 30% of people over 60 years of age, and recent studies have shown it is caused by lack of bladder and urethral muscle regenerative, Frauscher said in a 2004 RSNA presentation on Sunday.
In the study, 20 women ages 36-84 who suffered from mild to severe urinary stress incontinence were treated with stem cells derived from skeletal muscle in their arms.
Two kinds of cells were used in the study: muscle cells or myoblasts, and connective tissue cells or fibroblasts. The fibroblasts were mixed with collagen as a carrier for the cells, and injected into the urethral submucosa and the myoblasts were directly injected into the urethral sphincter.
The cells were obtained from skeletal muscle biopsy of the left arm, and disassociated using a modified cell dispersion technique to grow myoblasts and fibroblasts.
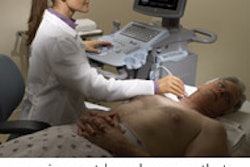
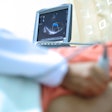
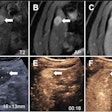
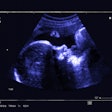
The aim was to strengthen the urethral muscle and the contracting capacity of the sphincter. Real-time transurethral 3D ultrasound helped in placing the stem cells in contact with the urethra and sphincter tissue, and was critical to the success of the procedure.
The ultrasound unit used was a Hitachi 6500 and Sequoia 512. The endoluminal transducer was 15 MHz.
Transurethral and 3D ultrasound were also used in the run-up to the procedure to investigate the lower urinary tract. A defined incontinence score; urodynamic, electromyographic, and laboratory parameters; quality of life; morphology; and function of the urethra and rhabdosphincter were among the other parameters evaluated one year before the therapy and one year after.
According to Frauscher, some patients showed immediate results and were continent within 24 hours of the 15- to 20-minute outpatient procedure. Eighteen of the 20 patients were continent in the one-year follow-up after the procedure. Results were more permanent, unlike the existing treatment with collagen injections.
"Transurethal US showed significantly increased thickness of urethra as well as improved contractility of the rhabdosphincter after therapy," Frauscher wrote in his scientific paper.
In the two patients in whom the cure was not complete, he explained the reason could be that the regenerative ability of stem cells was lower in older patients.
By N. Shivapriya
AuntMinnie.com staff writer
November 29, 2004
Related Reading
Ultrasound alters management of infants with genitourinary disorders, October 14, 2004
Copyright © 2004 AuntMinnie.com