While effective, high-intensity focused ultrasound (HIFU) treatment of solid cancerous tumors comes with risk for both major and minor complications, according to research from the Catholic University of Korea in Seoul.
From a 36-month period of using HIFU to treat patients with liver and pancreatic cancer, radiation oncologists at the university's St. Mary's Hospital found that approximately 9% of pancreatic cancer patients and 5% of hepatic tumor patients developed major complications from HIFU treatment.
HIFU treatment uses ultrasound beams with short wavelengths and megahertz (MHz) frequencies focused into small-volume target areas to cause immediate coagulative necrosis of the targeted tissue. In theory, damaged tissue is supposed to be confined within the area of intended ablation, with no harm to overlying and adjacent structures.
However, this did not prove to be the case for St. Mary's patients, none of whom escaped minor complications, according to lead author Seung Eun Jung, MD, of the department of radiology, and colleagues. The researchers described the types of complications and their potential causes in an article published online in Abdominal Imaging (May 29, 2010).
Between January 2006 and December 2008, 114 consecutive patients had 133 sessions of HIFU treatment in lieu of surgery, which they were ineligible to undergo or declined. Of the patients, 79 had malignant liver tumors, including 55 with hepatocellular carcinoma, two with primary cholangiocarcinoma, and 22 with liver metastases. Thirty-five patients had T4 stage pancreatic cancer.
All patients underwent general anesthesia for the procedure. Each target mass was ablated in multiple 5-mm sections with a 5-mm ablation margin. The HIFU treatment parameters included a therapy frequency of 0.8 MHz, a therapy power of 120-350 watts, a focus distance of 135 mm, and a mean focal field length of 9.8 mm and diameter of 1.1 mm.
All patients were hospitalized for at least two days following treatment, with a median time of five days for patients with hepatic tumors and six days for patients with pancreatic cancer. Two weeks after treatment, they were assessed with a contrast-enhanced MRI exam. Patients with primary hepatic tumors were followed for a median of almost eight years. Median follow-up for patients with metastatic liver tumors was seven months, and for patients with pancreatic cancer it was four months.
Complications
Hepatic tumor patients all had rib necrosis and skin redness. Two-thirds of the patients experienced grade 1 to grade 3 pain, and 10 patients had numb skin where the treatment was administered.
All pancreatic cancer patients developed vertebral body necrosis, and 29% of these patients developed subcutaneous fat necrosis. All cases were asymptomatic. All but two of the patients with pancreatic cancer also experienced erythematous changes and skin redness; the two other patients developed second- and third-degree burns on their skin. Seventy percent of the patients experienced grade 1 to grade 3 pain.
Four patients with hepatic tumors had major complications. These included fistula formation between an abdominal wall abscess and ablated hepatic tumors, a pneumothorax related to artificial pleural effusions, a periprocedural symptomatic pleural effusion, and a biliary obstruction. Additionally, two years after treatment, one patient had a rib fracture, and another patient had a diaphragmatic rupture.
Two patients with pancreatic cancer had tumor-duodenal fistulas with severe abdominal pain, and one patient had a third-degree burn of the anterior abdominal wall.
Jung and colleagues attributed the complications to artificial pleural effusion, and to thermal injury. They suggested that thermal injury at untargeted regions may have been caused by accumulating energy from reflected and absorbed ultrasounds. Reflection of ultrasound beams by the peritoneum, pleura, or hepatic capsules could accumulate on the abdominal wall, made easier by its layered structure; this could induce abdominal wall injury, the authors suggested. Similarly, the absorption and accumulation of ultrasound beams by the ribs could have caused injury to this area.
Complications were also attributed to cavitation, the formation of gas bubbles that grew and collapsed due to acoustic pressure waves, damaging both the target and surrounding tissue. Ultrasound beams passing through the target area were believed to have been absorbed by the vertebral body located posterior to pancreatic cancer, causing vertebral body necrosis.
The third-degree burn was caused by use of an improper water pack with a thick and rough wall. The authors blamed an internal metallic stent covering the duodenum for the development of a tumor-duodenal fistula in one patient.
By being aware of the types of complications that patients with liver and pancreatic cancer may experience, radiation oncologists can take the necessary precautions to avoid such complications, the authors wrote.
Careful selection of patients for HIFU treatment is essential, and patients whose tumors are adjacent to a bowel loop with a stent are not candidates for this treatment, they wrote. Proper positioning is essential, along with preoperative bowel cleaning, nasogastric tube insertion, and compressing the bowel loops with thin and floppy water packs.
By Cynthia E. Keen
AuntMinnie.com staff writer
July 12, 2010
Related Reading
High-intensity ultrasound alters prostate, but cancer often remains, May 10, 2010
Focused ultrasound burns away uterine fibroids noninvasively, March 17, 2010
SPIE: New uses for focused ultrasound to treat brain diseases defined, March 15, 2010
High-intensity focused ultrasound effective against high-risk prostate cancer, January 16, 2007
Copyright © 2010 AuntMinnie.com




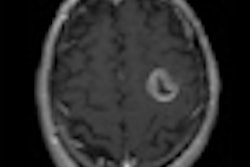







![A 53-year-old patient (patient number four) with a recurrent pituitary adenoma with extension of a cystic component of disease to the medial temporal lobe apparent on MRI (contoured in blue), and extension of disease to the left sphenoid bone and orbital apex apparent on [68Ga]Ga-DOTA-TATE (contoured in yellow).](https://img.auntminnie.com/mindful/smg/workspaces/default/uploads/2026/04/pituitary-tumor.QGsEnyB4bU.jpg?auto=format%2Ccompress&fit=crop&h=112&q=70&w=112)





