A new study found that sonographers who performed cardiac ultrasound studies on patients who received nuclear myocardial perfusion imaging (MPI) scans were exposed to residual radiation from the patients. While the radiation levels were low, the researchers advised that sonographers modify their scanning techniques.
The group found that sonographers performing transthoracic echocardiograms (TTEs) on patients who had received MPI studies were exposed to measurable levels of radiation as the radionuclides in the patients decayed. Sonographers can minimize unnecessary radiation exposure, however, through simple steps, such as adopting a left-handed approach when scanning or, when possible, delaying the follow-up TTE study. The results were published online April 3 in the Journal of the American Society of Echocardiography.
"In institutions in which a relatively large number of patients may undergo both types of examinations, the sequence of performing TTE and MPI should be scheduled to reduce exposure," wrote lead author Dr. Samia Massalha and colleagues from Rambam Health Care Campus in Haifa, Israel.
Too close?
Approximately 15 million to 20 million MPI procedures with radioactive tracers are performed annually in the U.S. to diagnose heart disease and related abnormalities. The population's average exposure to radiation from medical imaging has risen sixfold over the past 30 years, with MPI accounting for 10% of that increase, according to the authors.
With the increasing use of MPI, occupational exposure to radiation has been a concern among healthcare professionals. In addition, while past research has produced reliable estimates of radiation exposure for many clinicians, there has been inadequate study of radiation exposure for cardiac sonographers who scan patients after MPI exams, the group wrote.
"The need for conducting this study came from my work in both nuclear cardiology and in the echo lab, where we had to perform echocardiograms on patients post-MPI," Massalha wrote in an email to AuntMinnie.com. "At Rambam Health Care Campus, we are very attentive to both patients and staff safety; we felt that this group of staff in the echo lab must be addressed for safety purposes."
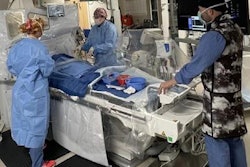
The problem is sonographers' proximity to patients who undergo TTE within hours of their receiving radiotracer injections for MPI stress and rest tests.
"During such studies, the examiners sit very close to and frequently wrap their arms and bodies over patients who may have been recently administered radioactive agents, which make them transiently radioactive," the authors wrote. "Proximity to the radioactive source, the relatively long duration of the exposure, and the short period of time after MPI are important determinants of potential radiation dose absorption by cardiac sonographers."
Different approaches
In this study, Massalha and colleagues included 30 patients scheduled for both MPI and TTE as part of their routine clinical cardiac workup. They also included 10 healthy subjects as controls who underwent TTE only and no MPI.
MPI rest and stress scans were performed on the same day; patients received 296 MBq (8 mCi) of technetium-99m (Tc-99m) sestamibi for the rest evaluation and 925 MBq (25 mCi) for the stress portion. TTE exams were conducted a mean of 3.61 (± 0.7) hours after MPI rest and 1.45 (± 0.48) hours after MPI stress studies.
The TTE scans were performed from two positions. In the right-handed approach, the echocardiographer and cardiac sonographer sat on the patient's right side and reached across the patient's body with the transducer in the right hand. With the left-handed approach, the cardiac sonographer sat to the patient's left and used the left hand to hold the transducer. The echocardiographer did not participate in the left-handed scenario.
To measure radiation levels, both examiners wore seven thermoluminescent dosimeter badges: These were located on the forehead and wrists, at the anterolateral right and left chest, at the sternal notch, and at the umbilical region.
With the right-handed approach, both the echocardiographer and cardiac sonographer had positive radiation readings at the right chest wall and right wrist. The cardiac sonographer also had a positive reading in the umbilical region, but the echocardiographer did not.
In the left-handed scenario, the cardiac sonographer had positive radiation readings at the left chest wall and the left wrist, but the levels were considerably less than with the right-handed approach.
| Radiation exposure to cardiac sonographer after MPI studies | ||||
| Scanning | Right chest wall | Right wrist | Left chest wall | Left wrist |
| Right-handed | 0.59 ± 0.12 mSv | 1.06 ± 0.21 mSv | NA | NA |
| Left-handed | NA | NA | 0.12 ± 0.02 mSv | 0.34 ± 0.07 mSv |
"The most important factor that contributes to the differences in the degree of staff radiation exposure when performing a left-handed TTE, compared to right-handed TTE, is mainly distance from the radiation source [the patient]," Massalha explained.
For example, the umbilical region had a positive reading for right-handed but not left-handed TTE because of the average distance between the thorax of the sonographer and the patient during left-handed TTE. Also, the radiation level at the right wrist was greater than at the right chest wall because the right hand was closest to the patient.
"Unlike with right-handed TTE, with left-handed TTE, the sonographer does not have to frequently lean over the patient, bringing the core of his or her body closer to the patient," the authors noted.
Safety first
Massalha and colleagues recommended that sonographers who perform more than 20 exams per year wear monitoring devices, especially if they are exposed to radiation of 0.05 mSv or more.
"A workflow of 20 such patients per week may lead to exposures exceeding standard annual occupational dose limits, such as those defined by the U.S. Nuclear Regulatory Commission (50 mSv)," they wrote.
In addition, they advised that clinicians consider delaying follow-up TTE scans until the day after MPI stress and rest tests to allow for the radiotracers to lose potency.
"For the commonly used radiotracers in MPI, other than thallium, a delay of 24 hours reduces possible exposure to less than 7% compared to a TTE immediately following an MPI," Massalha said. "This time should be extended when thallium is used due to its longer half-life."
The best-case scenario would be for TTE exams to be performed prior to injection of the MPI radiotracer. However, as the authors noted, this approach is not always an option because the need for a follow-up exam is often based on MPI results.
"In our center, we avoid performing an MPI first," Massalha said. "We do not routinely perform left-handed studies, so mainly we perform a TTE first or a next-day TTE, if that is not possible."
The researchers plan to continue their work by investigating the amount of radiation received by staff performing cardiac percutaneous procedures guided by echocardiograms, given the increasing number of these procedures.