Two studies from Mount Sinai School of Medicine in New York City are shedding light on the role of FDG-PET in analyzing plaques in carotid arteries and the aorta as a precursor to cardiac health.
Researchers said the studies are important because as much as 70% of all myocardial infarctions are due to the rupture of nonsclerotic lesions.
Atherosclerotic plaques appear in different forms. High-risk plaque, the kind frequently linked with clinical events, consists of a large lipid core, has a very thin fibrous pad, and often is infiltrated with macrophages. By comparison, the more stable plaque has a small lipid core, a thicker fibrous pad, and generally contains fewer inflammatory cells.
"Patients with the kind of plaque with heavy microphage infiltration are most likely to develop clinical syndromes," noted Dr. James Rudd, a cardiologist with Mount Sinai's Imaging Sciences Laboratory. "It would be a distinct advantage to get a handle on the microphage content of plaques in vivo noninvasively."
Assessing risk factors
One study took 41 patients and collected risk factor information, including sex, age, body mass index (BMI), individual histories of diabetes, coronary artery disease, smoking, and ethnicity. All 41 patients underwent a PET/CT scan with carotid artery image acquisition 150 minutes after injection of 10 mCi of FDG. A subset of 28 patients also underwent imaging of the aorta with a distribution time of 90 minutes after injection.
To estimate FDG uptake into the plaque, mean standard uptake values (SUV) were calculated using the region-of-interest (ROI) applied to each PET/CT image obtained in the carotid artery territory. The study also obtained a tissue-to-background ratio (TBR), which is reflective of arterial FDG uptake. Researchers then correlated the TBR with the risk factors in the carotid and the aorta.
In analyzing the images, the study viewed CT, PET, and the fused PET/CT images in the axial plane, highlighting the ROI in the right carotid arteries. After the PET scan, the study recorded the maximum SUV within the ROI and repeated the process for all axial images of the scan, averaging the values to obtain one SUV for each artery.
Gender influence
Partial correlations were performed for each risk factor to determine the unique contribution of each to SUV. One major correlation was found between male gender and high FDG uptake, with the average (standard deviation) of FDG uptake in males 1.6 (0.28) vs. females 1.4 (0.1).
The study found no significant independent contribution of age, diabetes, history of coronary artery disease, history of smoking, BMI, use of statins, or ethnicity to carotid artery FDG uptake. However, combining the risk factors of gender, use of statins, and Caucasian or Indian ethnicity into a predictive model using multivariate analysis provided a better predictive model of SUV than any other single risk factor or combination of risk factors.
For the 28-patient subset, there were "significant associations again with male gender in all sections of the aorta," said Kelly Myers, from Mount Sinai's Imaging Science Laboratory, in her presentation at the 2007 SNM meeting in Washington DC. "We also found significant associations with BMI in all aortic segments. In contrast to the carotid arteries, there was no significant association between uptake in the aorta and coronary artery disease, although there were trends in the ascending aorta and the aortic arch."
The study noted some potentially confounding factors, such as the majority of coronary artery disease (CAD) patients were male. "But within our group," she added, "we found that males and those with CAD do have more highly inflamed plaques and perhaps other conventional risk factors are not sensitive markers of inflammation."
Researchers also noted that only carotid FDG uptake -- and not aortic FDG uptake -- was associated with known CAD. Although again the study must rule out the confounding factor of gender, Myers said the finding "implies that carotid inflammation may be more reflective of CAD than aortic inflammation.
More questions
"The conclusions allow us to set the groundwork for what may be the most interesting question," Myers continued. "Can FDG-PET identify those at-risk for a future cardiovascular event?"
In the second study, researchers reviewed FDG-PET's ability to image inflammation within atherosclerotic plaque and differentiate symptomatic from asymptomatic lesions. The ultimate goal is to determine reproducibility of the technique and short-term variability of SUV signal.
If successful, FDG-PET imaging would help improve the risk stratification of patients and determine appropriate therapy for them. The findings, said Rudd, also might lead to novel drugs and therapies and determine the efficacy of those treatments.
The study took 11 asymptomatic patients with a mean age of 65 years. Patients with vascular disease underwent PET/CT imaging (Discovery LS, GE Healthcare, Chalfont St. Giles, U.K.). About half of the patients were diabetic and about two-thirds were male. Ascending, descending, arch, and abdominal aortic images were acquired 90 minutes after injection of 10 mCi FDG, while carotid images were acquired after 150 minutes after injection of the same dose of FDG.
Blind interpretations
To estimate interscan reproducibility, all patients repeated the same scan after 14 days, using identical imaging parameters. To assess inter- and intra-observer reproducibility, two readers separately read the first scan and on two separate occasions the scans were interpreted by one reader. Both readers were blinded to the patient demographics.
The results found that the mean (standard deviation) SUV for the aorta images were: Ascending aorta 1.39 (0.18), aortic arch 1.31 (0.16), descending aorta 1.23 (0.16), and the abdominal aorta was 1.30 (0.12). The mean SUV for the carotid was 1.59 (0.26).
Rudd said one area that did not fare well in reader agreement was the aortic arch. "It is probably due to the fact that this is a geometrically difficult structure to place regions-of-interest on," he added. "I think one reader may decide the borders of the structure differently from another reader."
The study determined that because reproducibility is good, PET is a beneficial technique to detect change in plaque inflammation and that drug trials will require only small patient numbers to show efficacy. The research also suggested that the aortic arch "be avoided for reproducibility and drug testing studies, because of the factors mentioned above," Rudd said. "The most reproducible areas are the carotid arteries and ascending and descending aortas, which should be the focus of the technique."
By Wayne Forrest
AuntMinnie.com staff writer
August 2, 2007
Related Reading
Rubidium PET/CT shows potential for coronary artery disease diagnosis, March 30, 2007
Automated emission correction shows potential for cardiac PET/CT, March 9, 2007
PET identifies inflammation severity in carotid plaques, November 21, 2006
PET perfusion can predict cardiac events, March 15, 2006
PET, SPECT measures of LVEF have superior predictive value, March 13, 2006
Copyright © 2007 AuntMinnie.com





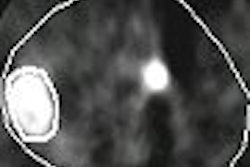







![A 53-year-old patient (patient number four) with a recurrent pituitary adenoma with extension of a cystic component of disease to the medial temporal lobe apparent on MRI (contoured in blue), and extension of disease to the left sphenoid bone and orbital apex apparent on [68Ga]Ga-DOTA-TATE (contoured in yellow).](https://img.auntminnie.com/mindful/smg/workspaces/default/uploads/2026/04/pituitary-tumor.QGsEnyB4bU.jpg?auto=format%2Ccompress&fit=crop&h=112&q=70&w=112)