A new computer-aided-detection (CAD) application is showing great promise as a companion to coronary CT angiography (CTA), recording both high sensitivity and low numbers of false-positive marks.
Researchers from the Medical University of South Carolina (MUSC) in Charleston clocked the investigational software at 100% negative predictive value (NPV) for ruling out significant stenosis in patients with chest pain.
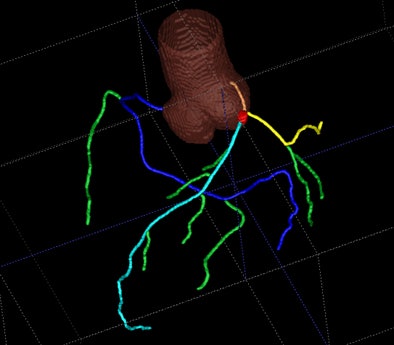 |
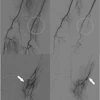
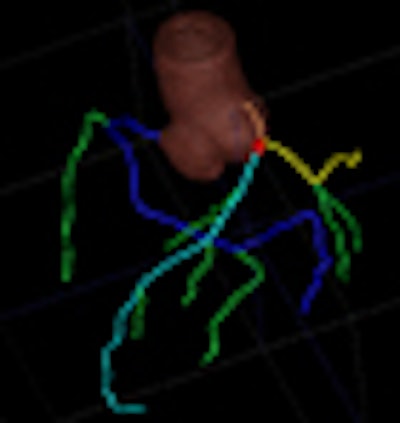
| CAD display shows axial CT image of coronary artery tree. All images courtesy of Dr. Joseph Schoepf. |
The system marks CAD's first foray into coronary artery stenosis detection, according to Dr. Joseph Schoepf and his colleagues from MUSC.
"Considering that coronary artery disease is the most important socioeconomic healthcare problem in the westernized world, the application of such techniques to this disease state is surprisingly rare," they wrote, noting an "urgent need" for new methods to improve timely and accurate detection while reducing costs (European Radiology online, November 5, 2009).
The study evaluated the performance of CAD for automated stenosis detection in 59 patients (38 men; mean age, 58 ± 12 years) presenting with chest pain, all of whom underwent both coronary CTA and quantitative coronary angiography, which served as the reference standard.
The day before angiography, all patients received coronary CTA scans: 30 patients were scanned using a 64-detector-row Somatom Sensation scanner (Siemens Healthcare, Malvern, PA), and the remaining 29 patients received dual-source scanning on a Somatom Definition (Siemens) scanner.
Patients received a contrast injection of 60-80 mL of a nonionic contrast medium (Isovue, 370 mg I/mL iopamidol, Bracco Diagnostics, Princeton, NJ) at 5-6 mL/sec, followed by a 50 mL saline chaser bolus using a dual-syringe injector.
Standard parameters for both modalities included (for 64-slice CTA) 64 x 0.6-mm collimation, pitch 0.2, 120-kV tube voltage, and 700-mAs tube current. Dual-source CT used 2 x 32 x 0.6-mm collimation, pitch 0.2-0.43, 120-kV tube voltage, and 560-mAs tube current.
Computer-aided detection
All images were analyzed using a software algorithm for automated complete detection of coronary artery stenosis (COR Analyzer, Rcadia Medical Imaging, Auburndale, MA). The performance of the algorithm for detecting stenosis of 50% or more was then compared with angiography.
The CAD system analyzes the four major coronary arteries: left main (LM), left anterior descending (LAD), left circumflex (LCx), and right coronary artery (RCA), for the presence and location of clinically significant (50% or more) coronary artery stenoses.
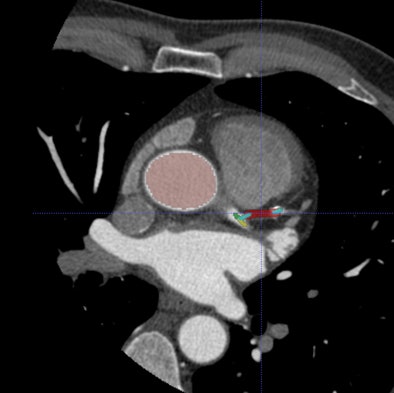 |
| Axial CT image with overlay coloring. |
The software begins by detecting and segmenting the aorta, and proceeds with the localization of the coronary artery ostia as contrast-filled structures connected to the aorta, Schoepf et al explained. Tubular components are tracked to build the coronary tree, which is then "pruned" of erroneously connected structures.
"The reconstructed coronary artery tree is split into disjoint vessel segments and analysis is performed for each segment separately," the authors wrote. "External boundaries and the lumen of the artery are delineated using an iterative model-based variation approach. Calcified lesions are detected and segmented. Noncalcified plaque is detected as a hypoattenuating area between the external vessel boundary and lumen without calcium."
Parameters are extracted for every cross-section of the vessel segment, including presence and size of plaques, bifurcations, noise level, and extent of artifacts. Finally, the algorithm "matches extracted features to the characteristics of lesions that were used to train the algorithm" and deploys a mark if the lesion features are likely to indicate a significant stenosis, they wrote.
Results
Quantitative catheter angiography detected 38 stenoses with ≥ 50% obstruction, of which the algorithm identified 28 (74%).
|
The CAD algorithm correctly identified 19/19 patients with 205 significant stenoses in any vessel and correctly excluded 206 significant stenoses in 26/40 patients.
CAD also marked 33 false positives (average 0.56 per patient), of which 19 were associated with stenotic lesions of less than 50% at angiography. Fourteen of the marks had no association with an atherosclerotic surrogate.
"These 14 false-positive detection marks were associated with high overall image noise (n = 1), stairstep artifacts from ECG misregistration and patient-related motion (n = 3), or had no obvious explanation (n = 10)," the authors wrote. On a per-patient basis, the software falsely identified 14 of 59 subjects (24%) as positive for significant stenosis of 50% or more.
"Accounting for the 19 detection marks that were deployed on stenotic lesions of less than 50% and considering only the detection marks that were not associated with an atherosclerotic surrogate as false positives, the number of false-positive patient studies was reduced to 5 (9%)," they wrote.
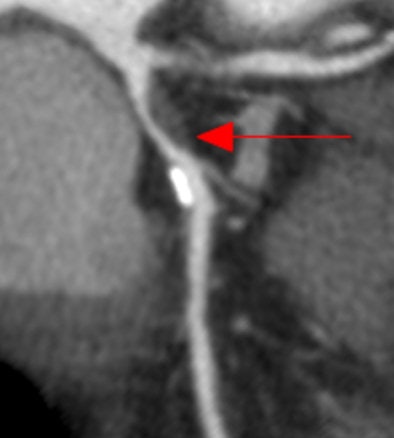 |
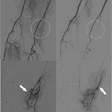
| Coronary CT angiography displayed as curved multiplanar reformation shows significant stenosis in the proximal left anterior descending coronary artery caused by noncalcified plaque. The lesion was correctly identified by the algorithm, and a true-positive detection mark (red arrow) was deployed. |
Relative to early algorithms and even commercial releases of CAD applications for other pathologies, this algorithm's performance was comparatively high.
"Particularly, the high NPV, in the range of 91-97% per vessel and 100% per patient, appear promising," Schoepf et al wrote. "Similarly, the comparatively low rate of false-positive detection marks sets this algorithm apart from computer-aided detection applications in other organ systems, which have traditionally struggled to find the right balance between high sensitivity and low false-positive rates. Furthermore, we found relatively high performance for diagnosing significant coronary artery stenosis on a per-patient level. However, per-vessel sensitivities showed considerable variation, with lower values than typically observed with human interpretation."
Still, considering the numbers, the algorithm in its current state of development appears more suitable for helping to exclude coronary artery stenosis in patient populations with a low likelihood and prevalence of disease, rather than establishing a diagnosis of significant coronary artery stenosis in populations with high likelihood and prevalence of obstructive lesions, the group wrote.
Quantitative coronary angiography, while a stronger reference standard than visual analysis at coronary CTA, is not perfect, Schoepf and colleagues stated.
If the CAD is "used as a second reader, the high negative predictive value may further enhance the confidence of excluding significant stenosis based on a normal or near-normal coronary CTA study," they concluded.
By Eric Barnes
AuntMinnie.com staff writer
November 19, 2009
Related Reading
Automated segmentation could improve fetal heart echo, November 6, 2009
CARS report: Fuzzy theory yields sharper CTA images, June 27, 2008
3D development outpaces facilities' readiness, June 23, 2008
Video game technology speeds beating-heart surgery, June 9, 2008
Preliminary study finds fMRI possible in fetal heart, October 7, 2005
Copyright © 2009 AuntMinnie.com