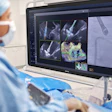
Treating early-stage breast cancer with balloon catheter brachytherapy is safe and effective, according to the initial research by the American Society of Breast Surgeons (ASBS).
The ongoing study examines the outcomes of 1,419 patients enrolled in the MammoSite Patient Registry. The trial was launched in 2002 by MammoSite maker Proxima Therapeutics of Alpharetta, GA. The ASBS took over in November 2003.
In a presentation at the 2004 Society of Surgical Oncology meeting in Atlanta, Dr. Peter Beitsch said that the technique was safe, had good cosmetic results, and gave excellent local control of cancer. Beitsch is with the Dallas Surgical Group in Dallas.
"We have had no true local recurrences," he said, although one patient had a distant new primary and there was one death in the study unrelated to breast cancer. "The test is, would I give it to my wife or mother, and I would."
The MammoSite balloon catheter was inserted into the cavity left after a lumpectomy. The balloon was inflated, and a radioactive source was introduced into the cavity through the catheter tube.
The cavity was irradiated twice a day for five days, for a total dose of 34 Gy in 10 fractions. In comparison, whole-breast irradiation uses 60 Gy over a six- to seven-week period.
The insertion can take place either at the time of surgery or later. More surgeons are opting to do it later, after they know the patient's margin status, Beitsch said.
Immediately after surgery and at two years, 95% of women reported excellent or good results, he said, adding that the technique had less cosmetic impact than whole-breast irradiation.
An important variable in the cosmetic outcome of the technique is the distance to the surface skin, or skin spacing, which tends to work better in women with larger breasts. When skin spacing was less than 7 mm, significantly more women reported fair to poor cosmetic outcomes. But even when skin spacing was less than 5 mm (only about 2% of the patients), 82% still reported excellent or good results, he said.
About 3% of patients reported radiation-related toxicity, such as radiation dermatitis, subcutaneous tissue changes, pain, and skin reddening.
Beitsch said the balloon brachytherapy technique appears to be comparable to whole-breast irradiation. "I feel that local control rates -- I don't like to use the word cure -- are just as good as with whole breast," he said.
Thus far, working with the balloon catheter has proved easier for clinicians than other brachytherapy applications, such as interstitial catheterization, 3D conformal external beam irradiation, and intraoperative radiation therapy, commented Dr. Henry Mark Kuerer from the University of Texas M. D. Anderson Cancer Center in Houston.
By Michael Smith
AuntMinnie.com contributing writer
March 30, 2005
Related Reading
MammoSite gets HCPCS codes, December 16, 2004
Fischer cleared for interstitial breast brachytherapy, December 2, 2004
Balloon brachytherapy suitable alternative to standard breast cancer radiation, June 15, 2004
Excision plus brachytherapy may obviate mastectomy for recurrent breast cancer, November 27, 2002
Copyright © 2005 AuntMinnie.com