CHICAGO – AI technology trained on standard x-rays may help plan patient-specific hip replacements, according to research presented November 26 at RSNA 2023.
Presenter Pouria Rouzrokh, MD, of the Mayo Clinic in Rochester, MN, discussed a model named THA-Net, a deep-learning algorithm with potential for making the presurgical planning process for total hip arthroplasty (THA) more efficient.
“As a standalone technology, this tool enables patient-specific surgical planning and identifies the optimal postoperative target,” Rouzrokh said, in a session on musculoskeletal imaging.
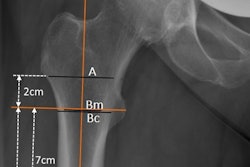
Traditionally, THA templating involves manual measurements and 2D implant renderings on preoperative x-rays. While a tedious process, optimal templating improves surgical efficiency and reduces complications by visualizing desirable surgical outcomes and anticipating challenges, Rouzrokh explained.
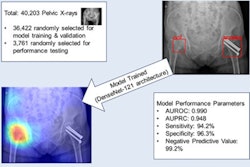
In this study, Rouzrokh and colleagues hypothesized that THA-Net would produce images as valid and realistic as actual x-rays, while requiring little to no input from surgeons. The model was trained on 356,305 x-rays from 14,357 patients who underwent procedures between 2020 and 2022.
THA-Net utilizes a pretrained YOLO (you only look once) model to crop the hip joint from an input preoperative pelvis x-ray and then employs a classifier-free conditional diffusion model for inpainting THA implants and generating realistic postoperative x-rays. In addition, the diffusion model was designed to offer two modes, an automated mode requiring only the input x-ray and and a hardware-aware mode that allows the user to specify the type of the hip replacement component.
To test THA-Net, two orthopedic surgeons assessed the realism of 100 real and 100 synthetic postoperative x-rays based on a 10-point Likert scale. Synthetic images generated by the algorithm were also assessed against software-based criteria.
 Pouria Rouzrokh, MD, of the the Mayo Clinic in Rochester, MN, discussed a model named THA-Net at RSNA on November 26 in Chicago. Image courtesy of the RSNA.
Pouria Rouzrokh, MD, of the the Mayo Clinic in Rochester, MN, discussed a model named THA-Net at RSNA on November 26 in Chicago. Image courtesy of the RSNA.
According to the findings, the surgical validity of synthetic postoperative x-rays (THA-Net “output”) was significantly higher than real ones, with mean difference among the reviewers of 0.8 points for the automated images and 1.1 points for hardware-aware generations.
Moreover, the reviewers couldn't differentiate between the real and synthetic x-rays, Rouzrokh said, with synthetic x-rays rated as realistic as their real counterparts in 95% of hardware-aware and 98% of automated generations. They exhibited excellent validity and realism when analyzed using validated software, he added.
Ultimately, future work on THA-Net will include external validation of the algorithm, with plans in place to deploy the model at the Mayo clinic, he said.
“Further refinement of this tool may allow it to interface with robotics, navigation, and AR/VR technologies to achieve desirable surgical execution while reducing dependence on 3D imaging data,” Rouzrokh concluded.