Autopsy misses injuries that can only be seen on postmortem CT for 17% to 21% of all injuries in those who died from firearms, pediatric trauma, or blunt force, according to a recent article on the National Institute of Justice website, NIJ.gov.
Researchers Sarah Lathrop, PhD, and Dr. Kurt Nolte worked with the New Mexico Office of the Medical Investigator to examine the potential of supporting or replacing forensic autopsies with postmortem CT.
They evaluated 174 blunt force injury deaths, 205 firearm deaths, 65 pediatric trauma deaths, and 460 drug poisoning deaths that occurred between June 2011 and December 2013. In each case, a full autopsy and complete postmortem CT were performed.
There was strong agreement between autopsy and postmortem CT in assigning the cause of death, they found. In 85% of blunt force injury deaths, 99.5% of firearm fatalities, and 81.4% of pediatric trauma deaths, the cause of death determined by CT was correct, matching the autopsy. Agreement on cause of death was significantly less in drug poisoning deaths, ranging from 34.2% to 77.9%, with significantly less agreement in the deaths of people older than 40.
"In an ideal world, all medical examiners would have access to not only a CT scanner, but an experienced radiologist to interpret the results from the scans for them," Lathrop and Nolte wrote in their grant report. "In the majority of cases included in this study, postmortem CT, when paired with a thorough external examination, could supplant autopsy and would be of particular value in cases of family, religious, or cultural objections," they added.





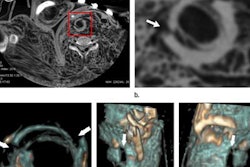










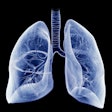

![Images show the pectoralis muscles of a healthy male individual who never smoked (age, 66 years; height, 178 cm; body mass index [BMI, calculated as weight in kilograms divided by height in meters squared], 28.4; number of cigarette pack-years, 0; forced expiratory volume in 1 second [FEV1], 97.6% predicted; FEV1: forced vital capacity [FVC] ratio, 0.71; pectoralis muscle area [PMA], 59.4 cm2; pectoralis muscle volume [PMV], 764 cm3) and a male individual with a smoking history and chronic obstructive pulmonary disorder (COPD) (age, 66 years; height, 178 cm; BMI, 27.5; number of cigarette pack-years, 43.2, FEV1, 48% predicted; FEV1:FVC, 0.56; PMA, 35 cm2; PMV, 480.8 cm3) from the Canadian Cohort Obstructive Lung Disease (i.e., CanCOLD) study. The CT image is shown in the axial plane. The PMV is automatically extracted using the developed deep learning model and overlayed onto the lungs for visual clarity.](https://img.auntminnie.com/mindful/smg/workspaces/default/uploads/2026/03/genkin.25LqljVF0y.jpg?auto=format%2Ccompress&crop=focalpoint&fit=crop&h=112&q=70&w=112)