Standard MDCT is an increasingly important modality for breast imaging, helping to find lesions that ultrasound, MRI, and even mammography can miss and increasing the utility of biopsy techniques. From incidental to interventional breast cancer imaging, there is much radiologists can do to exploit CT's abilities.
The benefits of breast CT begin when radiologists open their eyes to the lesions that appear on chest CT images, according to radiologist and informatics consultant Dr. Jeffrey Mendel, former chair of radiology at Caritas St. Elizabeth's Medical Center in Boston.
"While tomosynthesis in mammography is still a long way off ... we do breast tomography scanning every day at very high resolution," Mendel said at Stanford University's 2009 International Symposium on Multidetector-Row CT, held in San Francisco in May.
Incidental findings
Incidental breast cancer findings on CT comprise most of the modality's breast cancer detections, Mendel said. What the radiologist looks for is similar, but not identical, to that of a mammogram.
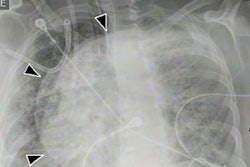
You look for the mass, "for asymmetry; skin thickening that is focal, not diffuse; enhancement; architectural distortion; or radiating spicules," Mendel said. "Don't look for microcalcifications on CT as they're rarely seen. If you see a calcification on CT, it's almost invariably a macrocalcification."
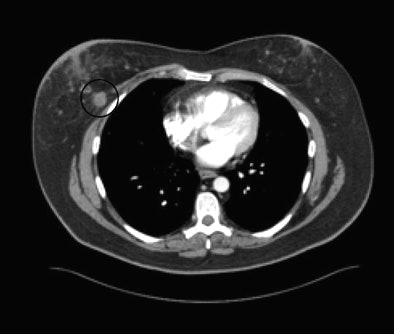 |
| Incidental breast lesion visible at CT (circled) could not be seen at repeated mammography targeted for this finding. All images courtesy of Dr. Jeffrey Mendel. |
Why are so many breast cancers seen for the first time on CT? For one thing, mammography at its best sees only 85% of breast lesions, he said. Many patients, particularly those with recurrent illness, don't undergo routine screening mammography. To find breast cancers, radiologists should remember that every chest CT is also a breast tomogram. Contrast enhancement can reveal more lesions.
"The problem is that our scanners are getting so fast," Mendel said. "Most breast cancers enhance in about two minutes; a lot of our [chest scanning] patients are off the table by then. So don't use a lack of enhancement to reassure you" that breast cancer is not present, "especially if the patient has had a rapid scan, such as for CT angiography," Mendel said.
Check for secondary findings such as axillary adenopathy, he noted. Look for thick, rimlike ductal or segmental enhancement, and use the American College of Radiology's (ACR) BI-RADS language to describe the findings whenever possible.
Also be sure to look at the old mammogram, he advised. "A lot of the things that look suspicious on CT have been on the mammo for years -- scarring and benign lesions -- and you can save yourself some time."
Adjunct to MR-guided biopsy
MR-guided breast biopsy has all the limitations of standard MRI, and then some, Mendel said. First, with MRI, patients spend long periods prone -- a difficult position to maintain. It's difficult to biopsy lesions near the chest wall because they're very superficial, and finally, it's difficult to sedate and monitor patients in the MR environment, he said.
There are also patients going to CT who have stereotactic biopsies scheduled, but the lesion cannot be accessed. With CT-guided biopsy, it can. If you've never run into these situations, it may be because you're not in an institution that performs breast MRI, a major source of referrals for breast CT, Mendel said.
"You have to bother to look -- if you don't think of it you won't," he said. "You'll be surprised at how many cancers you pick up in your chest imaging section. It startled me when we first started to look for these."
In highly specialized institutions, mammographers may be unaware of CT's breast imaging utility. If this is the case, "they may not be trying to enlist your help in problem-solving when they have a tough case," he said.
Easier imaging
But CT has some definite advantages: supine imaging, visualization of the entire breast, and an easy sedation and monitoring environment. And breast CT "can be easily performed with adjunctive ultrasound, something that is not available in the MR suite," Mendel said. The main challenges with CT are breast mobility and the rarity of the procedure.
The helical acquisition is straightforward: a typical chest CT protocol using 3-mm collimation and reduced kV (for example, 90 kVp without changing the mAs) for lower radiation dose, which increases signal-to-noise and contrast-to-noise ratios in the chest.
Although the standard breast CT exam is triphasic, often a single pass is sufficient, he said. If the lesion is visible on the first, noncontrast scan, the biopsy can begin. If contrast is needed to see the tumor, a postcontrast series can be acquired two minutes after the start of injection, and if questions remain, a third scan can be acquired at four to five minutes postcontrast, Mendel said. Dual-phase contrast injection and 40-cc saline flush are used to minimize artifacts.
CT-guided breast interventions
Two interventions performed with CT are:
- Automated core needle biopsy, for patients whose lesions cannot be safely accessed by MRI, or who cannot tolerate MRI
- Needle localization for surgical excision, for lesions that can be seen only at MRI or CT
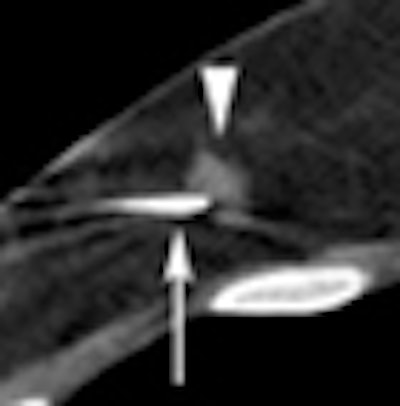
A typical inaccessible lesion found at MR was "a slightly irregular lesion picked up on MR that's at the back of our [biopsy] grid," he said. "That's as far back as we can accurately position a needle, and even if we could put the needle farther forward, we're getting very close to the chest wall." CT visualized the small infiltrating ductal carcinoma, and a hookwire localization biopsy was performed.
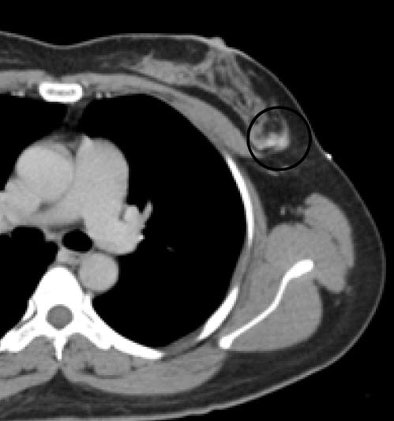 |
| Breast lesion (circle) was biopsied using CT guidance. |
CT allows for supine imaging, and the patient can be positioned obliquely. CT also allows for adjunctive ultrasound, an option not possible in the MR suite.
"Even with second-look ultrasound after breast MR, your ability to know precisely where the real image is in the breast is limited," Mendel said. "The advantage of CT is that you can put in a skinny needle and take a quick look with ultrasound." If the lesion is visible, the biopsy can be completed with ultrasound guidance.
After the biopsy, always place a marker clip to allow for future needle localization with mammography, Mendel said, and do a postprocedure CT to confirm that the marker is within the biopsy bed.
Postprocedure mammography documents the location of the marker immediately after the biopsy, he said. If the marker clip is not detectable by mammography, future needle localization should be scheduled using CT guidance.
Despite its limitations, CT performs several tasks in which other modalities fall short, Mendel said. MRI is limited by lack of availability, long exam times, contraindications, and prone positioning. Ultrasound doesn't work well in large or tender breasts.
The three-phase CT acquisition can help answer difficult diagnostic questions -- such as distinguishing breast cancer from infection or inflammation. Following enhancement, breast cancers tend to plateau or wash out in the third phase, whereas enhancement tends to persist in infections or inflammatory lesions, Mendel said, adding that the most important thing is to be aware of the breast cancers that appear on CT every day.
"My fellow countryman Wayne Gretzky says you miss 100% of the shots you don't take," Mendel said. "The breast is part of the chest and we have to look for [lesions] if we're going to find them. Keep the mammographers involved. Make sure they're aware of our abilities as chest imagers with CT, and also remember that we can solve clinical problems."
By Eric Barnes
AuntMinnie.com staff writer
September 2, 2009
Related Reading
Breast imagers, ahoy: New technology on the horizon, August 20, 2009
Study: MRI may cause more harm than good in breast cancer, August 13, 2009
Digital breast tomosynthesis cuts recall rate by 30%, August 4, 2009
CARS report: Novel conebeam CT cuts breast dose, improves accuracy, June 29, 2009
Italian study backs tomosynthesis over DR for lung pathology, February 18, 2009
Copyright © 2009 AuntMinnie.com